小干扰RNA沉默甲胎蛋白基因对HepG2细胞迁移及侵袭的影响
DOI: 10.3969/j.issn.1001-5256.2021.08.024
Effect of small interfering RNA silencing of the AFP gene on the migration and invasion of hepatocellular carcinoma HepG2 cells
-
摘要:
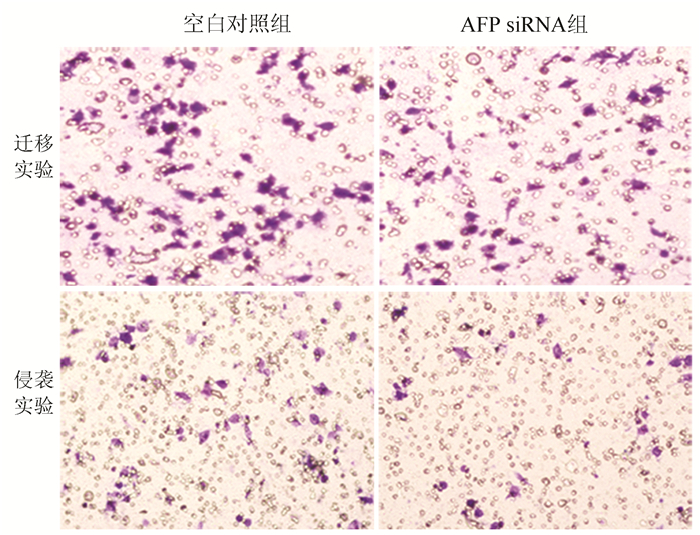
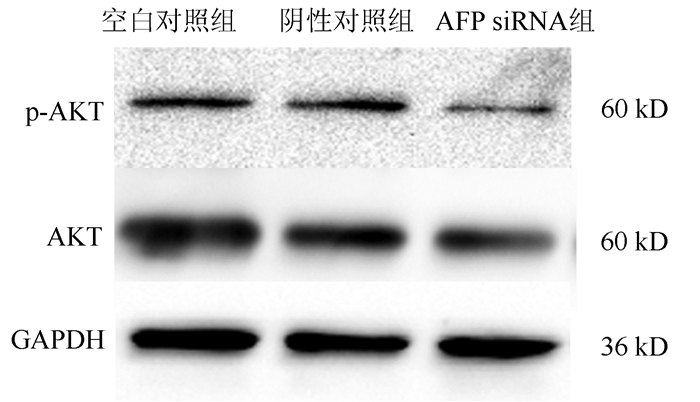
目的 研究甲胎蛋白(AFP)对肝癌HepG2细胞迁移和侵袭能力的影响及其机制。 方法 应用合成的靶向沉默AFP小干扰RNA(siRNA)转染肝癌HepG2细胞, 分为空白对照、阴性对照组及AFP siRNA组, 各组细胞干预48 h后, 采用实时定量PCR(qRT-PCR)和ELISA法检测细胞转染后的沉默效率, Transwell小室实验检测沉默AFP基因后HepG2细胞的侵袭、迁移能力, 用Western blotting法观察沉默AFP基因的表达对上皮-间质转化(EMT)相关蛋白(N-cadherin、Vimentin和E-cadherin)、AKT和p-AKT蛋白表达的影响。计量资料多组间比较采用单因素方差分析, 进一步两两比较采用LSD-t检验。 结果 转染沉默后, 与空白对照组相比, AFP siRNA组中AFP mRNA的相对表达量明显降低(P<0.01), 抑制率达86.440%, 同时AFP siRNA组细胞上清液中AFP蛋白表达水平同样明显降低(P<0.01)。与空白对照组相比, AFP siRNA组的迁移细胞数和侵袭细胞数显著下降, 差异具有统计学意义(P值均<0.01)。沉默HepG2细胞中AFP基因的表达后, 与空白对照组比较, AFP siRNA组EMT相关蛋白E-cadherin蛋白的表达水平升高(P<0.01), 而N-cadherin及Vimentin表达水平均明显降低(P值均<0.05), 且PI3K/AKT信号通路相关蛋白p-AKT的表达水平明显降低(P<0.01)。 结论 沉默AFP可抑制肝癌细胞转移, 基于HepG2细胞株的机制研究可能与阻断PI3K/Akt通路抑制EMT相关。 Abstract:Objective To investigate the effect of alpha-fetoprotein (AFP) on the migration and invasion abilities of hepatocellular carcinoma (HCC) HepG2 cells. Methods HCC HepG2 cells were transfected with synthesized small interference RNA (siRNA) for targeted silencing of AFP, and then HepG2 cells were divided into blank control group, negative control group, and AFP siRNA group. After 48 hours of intervention, quantitative real-time PCR and ELISA were used to measure the efficiency of silencing after transfection; Transwell assay was used to analyze the invasion and migration abilities of HepG2 cells after silencing of the AFP gene; Western blot was used to investigate the effect of AFP silencing on the expression of epithelial-mesenchymal transition (EMT)-related proteins (N-cadherin, vimentin, and E-cadherin), AKT, and p-AKT. A one-way analysis of variance was used for comparison of continuous data between groups, and the LSD-t-test was used for further comparison between two groups. Results After transfection and silencing, compared with the blank control group, the AFP siRNA group had a significant reduction in the relative mRNA expression of AFP (P < 0.01), with an inhibition rate of 86.440%, and the AFP siRNA group also had a significant reduction in the protein expression level of AFP in cell supernatant (P < 0.01). Compared with the blank control group, the AFP siRNA group had significant reductions in the numbers of migrating and invading cells (both P < 0.01). After the expression of the AFP gene was silenced in HepG2 cells, compared with the blank control group, the AFP siRNA group had a significant increase in the expression level of the EMT-related protein E-cadherin (P < 0.01) and significant reductions in the expression levels of the EMT-related proteins N-cadherin and vimentin (both P < 0.05), as well as a significant reduction in the protein expression level of p-AKT involved in the PI3K/AKT signaling pathway (P < 0.01). Conclusion Silencing AFP can inhibit the migration of HepG2 cells, possibly by blocking the PI3K/AKT signaling pathway and inhibiting EMT based on the mechanism of action of HepG2 cell line. -
表 1 沉默AFP在mRNA、蛋白水平表达以及肝癌HepG2细胞穿膜细胞率的变化
方法 空白对照组 阴性对照组 AFP siRNA组 F值 P值 AFP mRNA 1 0.927±0.041 0.136±0.0531) 466.70 <0.01 AFP(ng/ml) 235.500±19.340 217.400±11.750 33.930±11.6901) 172.60 <0.01 迁移实验(%) 100.000±7.420 93.660±6.140 58.570±10.4301) 36.92 <0.01 侵袭实验(%) 100.000±11.320 89.430±8.800 53.420±10.8101) 27.75 <0.01 注: 与空白对照组比较, 1)P<0.05。 表 2 各组细胞AFP、N-cadherin、Vimentin、E-cadherin、p-AKT蛋白相对表达量统计分析
组别 AFP E-cadherin Vimentin N-cadherin p-AKT 空白对照组 0.106±0.009 0.223±0.022 0.519±0.028 0.408±0.045 0.200±0.019 阴性对照组 0.103±0.011 0.222±0.014 0.430±0.063 0.355±0.062 0.194±0.010 AFP SiRNA组 0.015±0.0041) 0.375±0.0261) 0.151±0.0472) 0.102±0.0391) 0.116±0.008 F值 92.17 49.74 32.45 46.97 37.00 P值 <0.01 <0.01 <0.05 <0.01 <0.01 注: 与空白对照组比较, 1)P<0.01, 2)P<0.05。 -
[1] FORNER A, LLOVET JM. BRUIX J. Hepatocellular carcinoma[J]. Curr Opin Gastroenterol, 2006, 10(2): 339-351. DOI: 10.1016/S0140-6736(18)30010-2. [2] WANG S, WU QW, LI XK, et al. Interpretation of guidelines for the diagnosis and treatment of primary liver cancer in China (2019 edition)[J]. J Clin Hepatol, 2020, 36(5): 996-999. DOI: 10.3969/j.issn.1001-5256.2020.02.007.王姗, 吴庆旺, 李小科, 等. 《原发性肝癌诊疗规范(2019年版)》解读[J]. 临床肝胆病杂志, 2020, 36(5): 996-999. DOI: 10.3969/j.issn.1001-5256.2020.02.007. [3] YUAN SX, ZHOU WP. Progress and hot spots of comprehensive treatment for primary liver cancer[J]. Chin J Dig Surg, 2021, 20(2): 163-170. DOI: 10.3760/cma.j.cn115610-20201211-00776.袁声贤, 周伟平. 原发性肝癌综合治疗的进展和热点[J]. 中华消化外科杂志, 2021, 20(2): 163-170. DOI: 10.3760/cma.j.cn115610-20201211-00776. [4] WU M, LIU Z, ZHANG A, et al. Associated measurement of fucosylated levels of AFP, DCP, and GPC3 for early diagnosis in hepatocellular carcinoma[J]. Int J Biol Markers, 2019, 34(1): 20-26. DOI: 10.1177/1724600818812472. [5] BAI DS, ZHANG C, CHEN P, et al. The prognostic correlation of AFP level at diagnosis with pathological grade, progression, and survival of patients with hepatocellular carcinoma[J]. Sci Rep, 2017, 7(1): 12870. DOI: 10.1038/s41598-017-12834-1. [6] YANG X, ZHANG Y, ZHANG L, et al. Silencing alpha-fetoprotein expression induces growth arrest and apoptosis in human hepatocellular cancer cell[J]. Cancer Lett, 2008, 271(2): 281-293. DOI: 10.1016/j.canlet.2008.06.017. [7] CHEN SF, ZHAO LJ. Research progress on mechanisms for occurrence of liver cancer and its treatment status[J]. Chin J Gen Surg, 2018, 27(7): 910-923. DOI: 10.3978/j.issn.1005-6947.2018.07.016.陈世发, 赵礼金. 肝癌发生发展机制的研究进展及其治疗现状[J]. 中国普通外科杂志, 2018, 27(7): 910-923. DOI: 10.3978/j.issn.1005-6947.2018.07.016. [8] ZHANG J, CHEN G, ZHANG P, et al. The threshold of alpha-fetoprotein (AFP) for the diagnosis of hepatocellular carcinoma: A systematic review and meta-analysis[J]. PLoS One, 2020, 15(2): e0228857. DOI: 10.1371/journal.pone.0228857. [9] DING X, YANG LY, HUANG GW, et al. Role of AFP mRNA expression in peripheral blood as a predictor for postsurgical recurrence of hepatocellular carcinoma: A systematic review and meta-analysis[J]. World J Gastroenterol, 2005, 11(17): 2656-2661. DOI: 10.3748/wjg.v11.i17.2656. [10] MUEHLEMANN M, MILLER KD, DAUPHINEE M, et al. Review of growth inhibitory peptide as a biotherapeutic agent for tumor growth, adhesion, and metastasis[J]. Cancer Metastasis Rev, 2005, 24(3): 441-467. DOI: 10.1007/s10555-005-5135-2. [11] LI M, LI H, LI C, et al. Alpha-fetoprotein: A new member of intracellular signal molecules in regulation of the PI3K/AKT signaling in human hepatoma cell lines[J]. Int J Cancer, 2011, 128(3): 524-532. DOI: 10.1002/ijc.25373. [12] ZHENG L, GONG W, LIANG P, et al. Effects of AFP-activated PI3K/Akt signaling pathway on cell proliferation of liver cancer[J]. Tumour Biol, 2014, 35(5): 4095-4099. DOI: 10.1007/s13277-013-1535-z. [13] ZHANG CS, ZHANG XZ, HAN ZM, et al. Silence of cytoskeleton-associated protein 2 represses cell proliferation and migration and promotes apoptosis in liver cancer cell lines[J]. J Cent South Univ(Med Sci), 2020, 45(4): 365-371. DOI: 10.11817/j.issn.1672-7347.2020.180798.张昌生, 张学贞, 韩宗明, 等. 沉默细胞骨架相关蛋白2抑制肝癌细胞增殖和迁移并促进细胞凋亡[J]. 中南大学学报(医学版), 2020, 45(4): 365-371. DOI: 10.11817/j.issn.1672-7347.2020.180798. [14] ZHU MY, FU SG, LI MS, et al. Inhibited the activity of PTEN by α-Fetoprotein caused resistance to all trans retinoic acid of hepatoma cells[J]. Prog Biochem Biophys, 2011, 38(3): 227-238. DOI: 10.3724/SP.J.1206.2010.00546.朱明月, 符史干, 李孟森, 等. 甲胎蛋白抑制PTEN活性导致肝癌细胞耐受ATRA诱导的凋亡[J]. 生物化学与生物物理进展, 2011, 38(3): 227-238. DOI: 10.3724/SP.J.1206.2010.00546. [15] BRABLETZ T, KALLURI R, NIETO MA, et al. EMT in cancer[J]. Nat Rev Cancer, 2018, 18(2): 128-134. DOI: 10.1038/nrc.2017.118. [16] THIERY JP. Epithelial-mesenchymal transitions in tumour progression[J]. Nat Rev Cancer, 2002, 2(6): 442-454. DOI: 10.1038/nrc822. [17] WANG Y, GUO T, LI JH, et al. Biological function and regulatory mechanism of epithelial- mesenchymal transition-related long non-coding RNAs in liver cancer[J]. J Clin Hepatol, 2019, 35(3): 656-660. DOI: 10.3969/j.issn.1001-5256.2019.03.046.王元, 郭涛, 李靖华, 等. 上皮-间质转化相关长链非编码RNA在肝癌中的生物学功能及调控机制[J]. 临床肝胆病杂志, 2019, 35(3): 656-660. DOI: 10.3969/j.issn.1001-5256.2019.03.046. [18] CHAMBERS AF, GROOM AC, MACDONALD IC. Dissemination and growth of cancer cells in metastatic sites[J]. Nat Rev Cancer, 2002, 2(8): 563-572. DOI: 10.1038/nrc865. [19] SA R, SONG H, WEI M, et al. MiR-616 plays oncogenic role in hepatocellular carcinoma progression through suppressing PTEN expression and activating PI3K/AKT pathway[J]. Artif Cells Nanomed Biotechnol, 2020, 48(1): 728-734. DOI: 10.1080/21691401.2019.1596928. [20] THAPA N, CHEN M, HORN HT, et al. Phosphatidylinositol-3-OH kinase signalling is spatially organized at endosomal compartments by microtubule-associated protein 4[J]. Nat Cell Biol, 2020, 22(11): 1357-1370. DOI: 10.1038/s41556-020-00596-4. [21] GOLOB-SCHWARZL N, KRASSNIG S, TOEGLHOFER AM, et al. New liver cancer biomarkers: PI3K/AKT/mTOR pathway members and eukaryotic translation initiation factors[J]. Eur J Cancer, 2017, 83: 56-70. DOI: 10.1016/j.ejca.2017.06.003. [22] LEE S, CHOI EJ, CHO EJ, et al. Inhibition of PI3K/Akt signaling suppresses epithelial-to-mesenchymal transition in hepatocellular carcinoma through the Snail/GSK-3/beta-catenin pathway[J]. Clin Mol Hepatol, 2020, 26(4): 529-539. DOI: 10.3350/cmh.2019.0056n. -



 PDF下载 ( 2480 KB)
PDF下载 ( 2480 KB)

 下载:
下载: