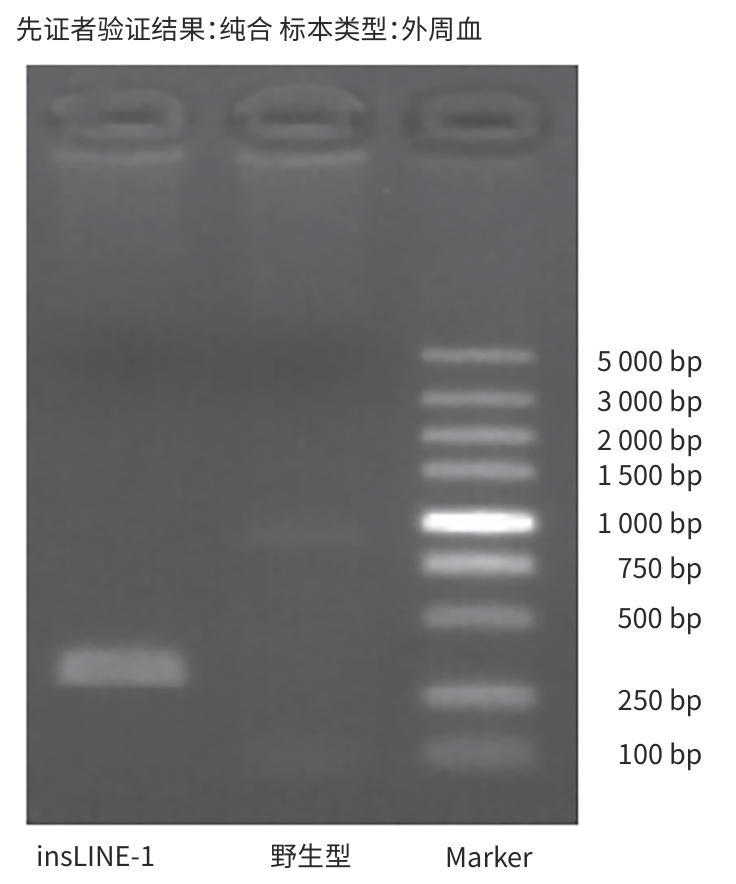
| [1] |
BAI J, ZHENG SJ, DUAN ZP. Clinical features and diagnosis of four common types of congenital hyperbilirubinemia[J]. J Clin Hepatol, 2019, 35( 8): 1680- 1683. DOI: 10.3969/j.issn.1001-5256.2019.08.005. |
| [2] |
|
| [3] |
MEMON N, WEINBERGER BI, HEGYI T, et al. Inherited disorders of bilirubin clearance[J]. Pediatr Res, 2016, 79( 3): 378- 386. DOI: 10.1038/pr.2015.247. |
| [4] |
MORAIS MB, MACHADO MV. Benign inheritable disorders of bilirubin metabolism manifested by conjugated hyperbilirubinemia-A narrative review[J]. United European Gastroenterol J, 2022, 10( 7): 745- 753. DOI: 10.1002/ueg2.12279. |
| [5] |
|
| [6] |
van de STEEG E, STRÁNECKÝ V, HARTMANNOVÁ H, et al. Complete OATP1B1 and OATP1B3 deficiency causes human Rotor syndrome by interrupting conjugated bilirubin reuptake into the liver[J]. J Clin Invest, 2012, 122( 2): 519- 528. DOI: 10.1172/JCI59526. |
| [7] |
CHENG YY, CHANG KC, CHEN PL, et al. SLCO1B1 and SLCO1B3 genetic mutations in Taiwanese patients with Rotor syndrome[J]. J Formos Med Assoc, 2023, 122( 7): 648- 652. DOI: 10.1016/j.jfma.2023.03.003. |
| [8] |
LIN LZ, WU QY, ZHANG JH, et al. A pedigree analysis of Rotor hyperbilirubinemia combined with hepatitis B virus infection in a SLCO1B1 and SLCO1B3 gene mutations patient[J]. Heliyon, 2024, 10( 13): e33864. DOI: 10.1016/j.heliyon.2024.e33864. |
| [9] |
|
| [10] |
YE JW, TAN LM, YANG FX, et al. Analysis of clinical feature and SLCO1B1 and SLC01B3 gene mutations in children with Rotor syndrome[J]. Guangzhou Med J, 2021, 52( 6): 1- 5. DOI: 10.3969/j.issn.1000-8535.2021.06.001. |
| [11] |
|
| [12] |
TAN YF, OUYANG WX, JIANG T, et al. Clinical characteristics and genetic analysis of four children with Rotor syndrome[J]. Chin J Med Genet, 2024, 41( 6): 715- 719. DOI: 10.3760/cma.j.cn511374-20220520-00342. |
| [13] |
ZHANG ZH, ZHENG BX, LI M, et al. SLCO1B1 and SLCO1B3 gene mutations in a Chinese boy with Rotor syndrome: A case report[J]. Chin Hepatol, 2016, 21( 7): 542- 544, 605. DOI: 10.14000/j.cnki.issn.1008-1704.2016.07.006. |
| [14] |
MORAIS M, COUVERT P, JÉRU I, et al. Rotor syndrome presenting as dubin-Johnson syndrome[J]. Case Rep Gastroenterol, 2022, 16( 2): 452- 455. DOI: 10.1159/000525517. |
| [15] |
ZENG XY, ZHANG T, SUN KW, et al. Rotor syndrome combined with HBsAg carriers: One case report[J]. Chin J Gastroenterol Hepatol, 2016, 25( 4): 446- 447. DOI: 10.3969/j.issn.1006-5709.2016.04.024. |
| [16] |
DIMOPOULOU D, LYRA V, DIMOPOULOU A, et al. Is hepatobiliary scintigraphy sufficient to diagnose rotor syndrome in a 3-year-old boy?[J]. J Nucl Med Technol, 2021, 49( 2): 193- 194. DOI: 10.2967/jnmt.120.257618. |
| [17] |
LI J, DENG CJ, HE SL, et al. Clinical characteristics and polymorphism of UGT1A1 gene in 53 cases of congenital hyperbilirubinemia in Yunnan[J]. J Kunming Med Univ, 2024, 45( 5): 136- 143. DOI: 10.12259/j.issn.2095-610X.S20240521. |
| [18] |
|
| [19] |
GEBERHIWOT T, MORO A, DARDIS A, et al. Consensus clinical management guidelines for Niemann-Pick disease type C[J]. Orphanet J Rare Dis, 2018, 13( 1): 50. DOI: 10.1186/s13023-018-0785-7. |
| [20] |
ERLINGER S, ARIAS IM, DHUMEAUX D. Inherited disorders of bilirubin transport and conjugation: New insights into molecular mechanisms and consequences[J]. Gastroenterology, 2014, 146( 7): 1625- 1638. DOI: 10.1053/j.gastro.2014.03.047. |
| [21] |
YEE SW, HALDAR T, KVALE M, et al. SLCO1B1 functional variants and statin-induced myopathy in people with recent genealogical ancestors from Africa: A population-based real-world study[J]. medRxiv, 2023. DOI: 10.1101/2023.12.02.23299324.[Preprint] |
| [22] |
KAGAWA T, ADACHI Y, HASHIMOTO N, et al. Loss of organic anion transporting polypeptide 1B3 function causes marked delay in indocyanine green clearance without any clinical symptoms[J]. Hepatology, 2017, 65( 3): 1065- 1068. DOI: 10.1002/hep.28950. |
| [23] |
KIM YG, SUNG H, SHIN HS, et al. Intronic LINE-1 insertion in SLCO1B3 as a highly prevalent cause of rotor syndrome in East Asian population[J]. J Hum Genet, 2022, 67( 2): 71- 77. DOI: 10.1038/s10038-021-00967-1. |
| [24] |
CHAUBAL AN, PATEL R, CHOKSI D, et al. Management of pregnancy in Crigler Najjar syndrome type 2[J]. World J Hepatol, 2016, 8( 11): 530- 532. DOI: 10.4254/wjh.v8.i11.530. |
| [25] |
BOUCHGHOUL H, BOUYER J, SENAT MV, et al. Hypoglycemia and glycemic control with glyburide in women with gestational diabetes and genetic variants of cytochrome P450 2C9 and/or OATP1B3[J]. Clin Pharmacol Ther, 2021, 110( 1): 141- 148. DOI: 10.1002/cpt.2142. |
| [26] |
SUN H, FRASSETTO L, BENET LZ. Effects of renal failure on drug transport and metabolism[J]. Pharmacol Ther, 2006, 109( 1-2): 1- 11. DOI: 10.1016/j.pharmthera.2005.05.010. |
| [27] |
NAUD J, MICHAUD J, LEBLOND FA, et al. Effects of chronic renal failure on liver drug transporters[J]. Drug Metab Dispos, 2008, 36( 1): 124- 128. DOI: 10.1124/dmd.107.018192. |
| [28] |
KUNZE A, EDIAGE EN, DILLEN L, et al. Clinical investigation of coproporphyrins as sensitive biomarkers to predict mild to strong OATP1B-mediated drug-drug interactions[J]. Clin Pharmacokinet, 2018, 57( 12): 1559- 1570. DOI: 10.1007/s40262-018-0648-3. |
| [29] |
UJIHIRA Y, TAN SPF, SCOTCHER D, et al. Genotype, ethnicity, and drug-drug interaction modeling as means of verifying transporter biomarker PBPK model: The coproporphyrin-I story[J]. CPT Pharmacometrics Syst Pharmacol, 2025, 14( 5): 941- 953. DOI: 10.1002/psp4.70008. |
| [30] |
PAUL WILSON JH, SINAASAPPEL M, LOTGERING FK, et al. Recommendations for pregnancies in patients with crigler-najjar syndrome[J]. JIMD Rep, 2013, 7: 59- 62. DOI: 10.1007/8904_2012_142. |



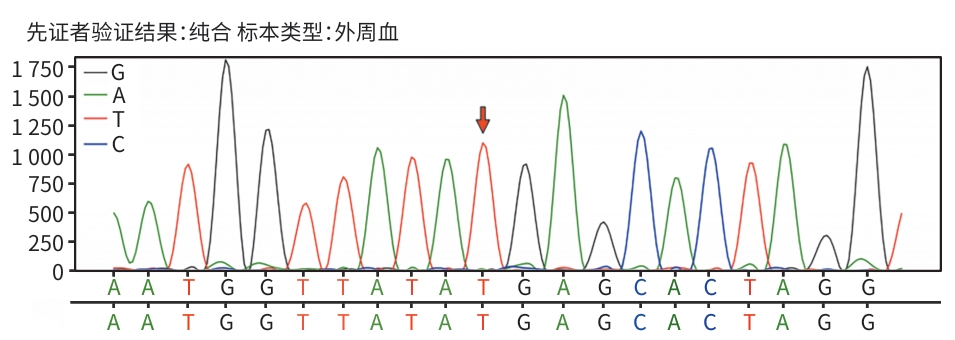




 DownLoad:
DownLoad: