| [1] |
Liver Disease Committee, Chinese Association of Integrative Medicine. Guidelines for diagnosis and treatment of liver fibrosis with integrated traditional Chinese and western medicine(2019 edition)[J]. J Chin Hepatol, 2019, 35( 7): 1444- 1449. DOI: 10.3969/j.issn.1001-5256.2019.07.007. |
| [2] |
YAMASHITA M, PASSEGUÉ E. TNF-α coordinates hematopoietic stem cell survival and myeloid regeneration[J]. Cell Stem Cell, 2019, 25( 3): 357- 372. e 7. DOI: 10.1016/j.stem.2019.05.019. |
| [3] |
BOZHILOV YK, HSU I, BROWN EJ, et al. In vitro human haematopoietic stem cell expansion and differentiation[J]. Cells, 2023, 12( 6): 896. DOI: 10.3390/cells12060896. |
| [4] |
PIETRAS EM, MIRANTES-BARBEITO C, FONG S, et al. Chronic interleukin-1 exposure drives haematopoietic stem cells towards precocious myeloid differentiation at the expense of self-renewal[J]. Nat Cell Biol, 2016, 18( 6): 607- 618. DOI: 10.1038/ncb3346. |
| [5] |
MOSSADEGH-KELLER N, SARRAZIN S, KANDALLA PK, et al. M-CSF instructs myeloid lineage fate in single haematopoietic stem cells[J]. Nature, 2013, 497( 7448): 239- 243. DOI: 10.1038/nature12026. |
| [6] |
ZHANG P, XU LM, GAO JS, et al. 3D collagen matrices modulate the transcriptional trajectory of bone marrow hematopoietic progenitors into macrophage lineage commitment[J]. Bioact Mater, 2022, 10: 255- 268. DOI: 10.1016/j.bioactmat.2021.08.032. |
| [7] |
WAN LF, PAN WT, YONG YT, et al. Research progress of single-cell transcriptome sequencing technology in liver fibrosis[J]. Curr Biotechnol, 2024, 14( 5): 793- 804. DOI: 10.19586/j.2095-2341.2024.0078. |
| [8] |
GUO JB. Effects of constitutive TL1A expression on myeloid cells in liver fibrogenesis and its reversal in mice[D]. Shijiazhuang: Hebei Medical University, 2016. DOI: 10.7666/d.D843844. 郭金波. 髓系细胞高表达TL1A在实验性小鼠肝纤维化发生和逆转过程中作用的研究[D]. 石家庄: 河北医科大学, 2016. DOI: 10.7666/d.D843844. |
| [9] |
CALCAGNO DM, CHU A, GAUL S, et al. NOD-like receptor protein 3 activation causes spontaneous inflammation and fibrosis that mimics human NASH[J]. Hepatology, 2022, 76( 3): 727- 741. DOI: 10.1002/hep.32320. |
| [10] |
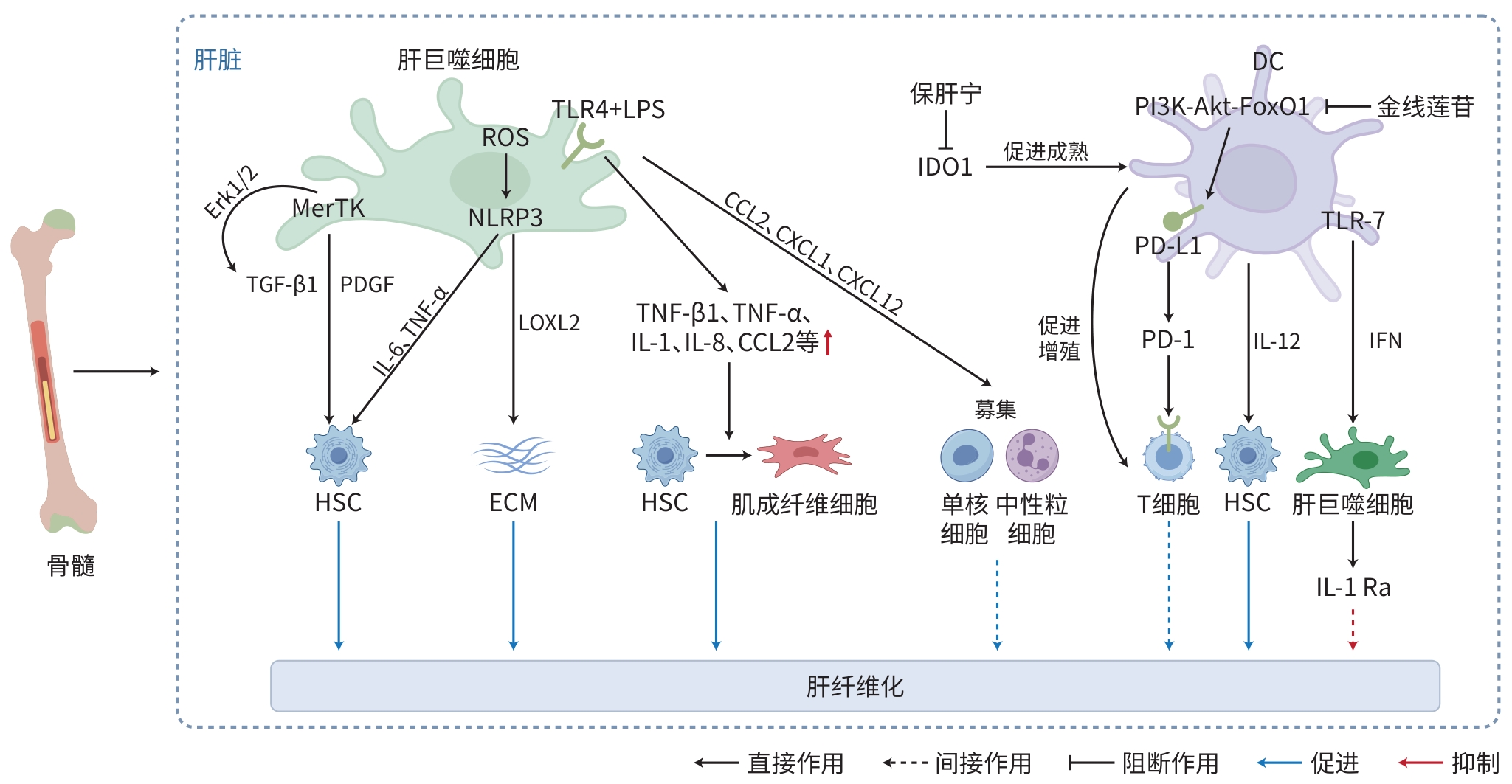
CAI BS, DONGIOVANNI P, COREY KE, et al. Macrophage MerTK promotes liver fibrosis in nonalcoholic steatohepatitis[J]. Cell Metab, 2020, 31( 2): 406- 421. e 7. DOI: 10.1016/j.cmet.2019.11.013. |
| [11] |
LI WY, CHANG N, LI LY. Heterogeneity and function of kupffer cells in liver injury[J]. Front Immunol, 2022, 13: 940867. DOI: 10.3389/fimmu.2022.940867. |
| [12] |
SLEVIN E, BAIOCCHI L, WU N, et al. Kupffer cells: Inflammation pathways and cell-cell interactions in alcohol-associated liver disease[J]. Am J Pathol, 2020, 190( 11): 2185- 2193. DOI: 10.1016/j.ajpath.2020.08.014. |
| [13] |
GUILLOT A, TACKE F. Liver macrophages: Old dogmas and new insights[J]. Hepatol Commun, 2019, 3( 6): 730- 743. DOI: 10.1002/hep4.1356. |
| [14] |
KOYAMA Y, BRENNER DA. Liver inflammation and fibrosis[J]. J Clin Invest, 2017, 127( 1): 55- 64. DOI: 10.1172/JCI88881. |
| [15] |
KALLIS YN, SCOTTON CJ, MACKINNON AC, et al. Proteinase activated receptor 1 mediated fibrosis in a mouse model of liver injury: A role for bone marrow derived macrophages[J]. PLoS One, 2014, 9( 1): e86241. DOI: 10.1371/journal.pone.0086241. |
| [16] |
LI J, LIU WQ, ZHANG J, et al. The role of mitochondrial quality control in liver diseases: Dawn of a therapeutic era[J]. Int J Biol Sci, 2025, 21( 4): 1767- 1783. DOI: 10.7150/ijbs.107777. |
| [17] |
ZHAO SX, LI WC, FU N, et al. CD14 + monocytes and CD163 + macrophages correlate with the severity of liver fibrosis in patients with chronic hepatitis C[J]. Exp Ther Med, 2020, 20( 6): 228. DOI: 10.3892/etm.2020.9358. |
| [18] |
XIANG M, LIU TT, TIAN C, et al. Kinsenoside attenuates liver fibro-inflammation by suppressing dendritic cells via the PI3K-AKT-FoxO1 pathway[J]. Pharmacol Res, 2022, 177: 106092. DOI: 10.1016/j.phrs.2022.106092. |
| [19] |
MO C, XIE SW, GAO L, et al. Baoganning formula alleviates liver fibrosis in mice by inhibiting hepatic IDO1 expression and promoting phenotypic maturation of dendritic cells[J]. J South Med Univ, 2021, 41( 7): 1002- 1011. DOI: 10.12122/j.issn.1673-4254.2021.07.06. |
| [20] |
|
| [21] |
HORN P, TACKE F. Metabolic reprogramming in liver fibrosis[J]. Cell Metab, 2024, 36( 7): 1439- 1455. DOI: 10.1016/j.cmet.2024.05.003. |
| [22] |
MOORING M, YEUNG GA, LUUKKONEN P, et al. Hepatocyte CYR61 polarizes profibrotic macrophages to orchestrate NASH fibrosis[J]. Sci Transl Med, 2023, 15( 715): eade3157. DOI: 10.1126/scitranslmed.ade3157. |
| [23] |
HOU C, WANG D, ZHAO MX, et al. MANF brakes TLR4 signaling by competitively binding S100A8 with S100A9 to regulate macrophage phenotypes in hepatic fibrosis[J]. Acta Pharm Sin B, 2023, 13( 10): 4234- 4252. DOI: 10.1016/j.apsb.2023.07.027. |
| [24] |
RAN JQ, YIN SX, ISSA R, et al. Key role of macrophages in the progression of hepatic fibrosis[J]. Hepatol Commun, 2025, 9( 1): e0602. DOI: 10.1097/hc9.0000000000000602. |
| [25] |
CHENG S, ZOU YH, ZHANG M, et al. Single-cell RNA sequencing reveals the heterogeneity and intercellular communication of hepatic stellate cells and macrophages during liver fibrosis[J]. MedComm, 2023, 4( 5): e378. DOI: 10.1002/mco2.378. |
| [26] |
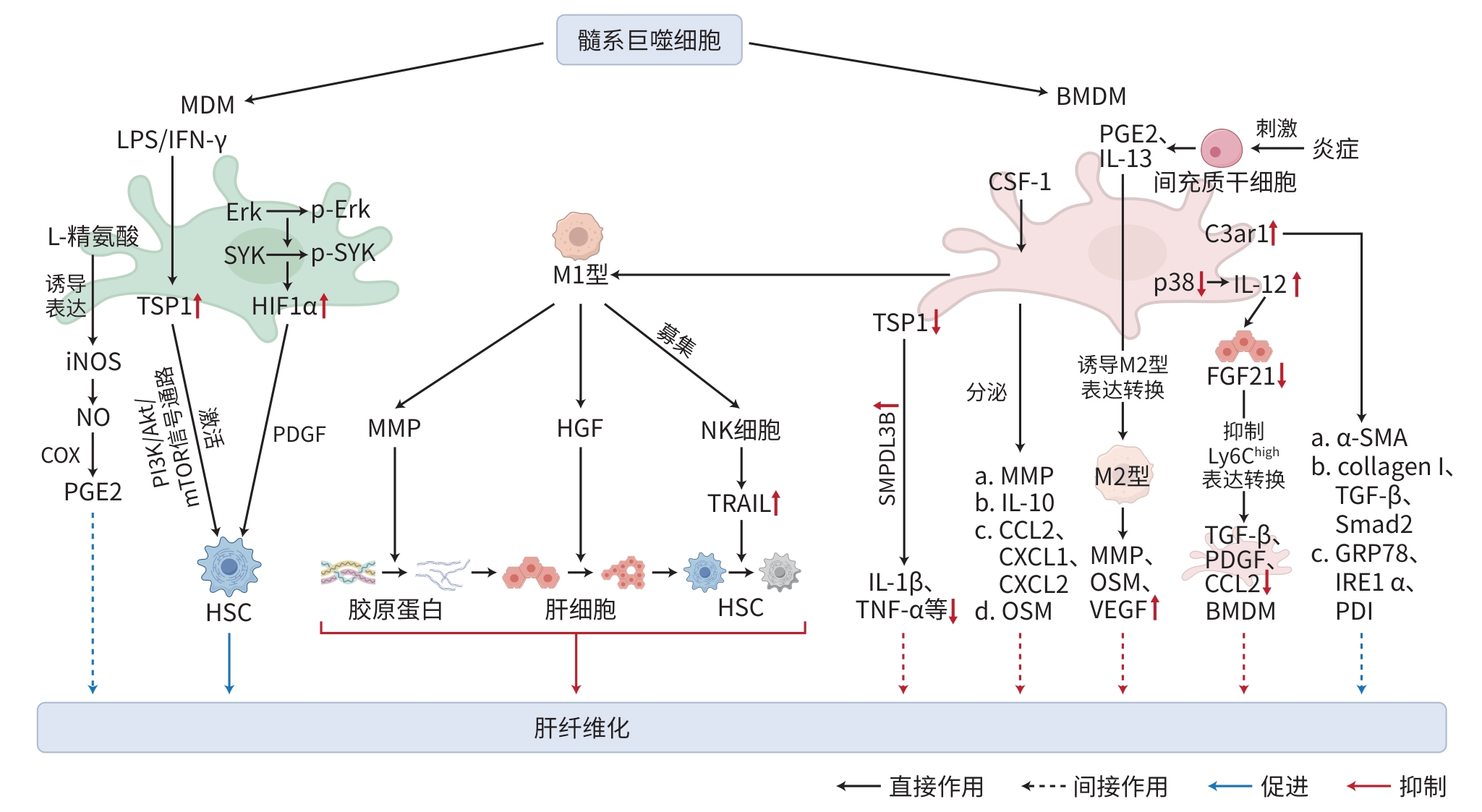
CHEN XJ, WANG ZY, HAN S, et al. Targeting SYK of monocyte-derived macrophages regulates liver fibrosis via crosstalking with Erk/Hif1α and remodeling liver inflammatory environment[J]. Cell Death Dis, 2021, 12( 12): 1123. DOI: 10.1038/s41419-021-04403-2. |
| [27] |
BRENIG R, POP OT, TRIANTAFYLLOU E, et al. Expression of AXL receptor tyrosine kinase relates to monocyte dysfunction and severity of cirrhosis[J]. Life Sci Alliance, 2020, 3( 1): e201900465. DOI: 10.26508/lsa.201900465. |
| [28] |
HAMMERICH L, TACKE F. Hepatic inflammatory responses in liver fibrosis[J]. Nat Rev Gastroenterol Hepatol, 2023, 20( 10): 633- 646. DOI: 10.1038/s41575-023-00807-x. |
| [29] |
MA PF, GAO CC, YI J, et al. Cytotherapy with M1-polarized macrophages ameliorates liver fibrosis by modulating immune microenvironment in mice[J]. J Hepatol, 2017, 67( 4): 770- 779. DOI: 10.1016/j.jhep.2017.05.022. |
| [30] |
GWAG T, REDDY MOOLI RG, LI D, et al. Macrophage-derived thrombospondin 1 promotes obesity-associated non-alcoholic fatty liver disease[J]. JHEP Rep, 2021, 3( 1): 100193. DOI: 10.1016/j.jhepr.2020.100193. |
| [31] |
WATANABE Y, TSUCHIYA A, SEINO S, et al. Mesenchymal stem cells and induced bone marrow-derived macrophages synergistically improve liver fibrosis in mice[J]. Stem Cells Transl Med, 2019, 8( 3): 271- 284. DOI: 10.1002/sctm.18-0105. |
| [32] |
CRESPO M, NIKOLIC I, MORA A, et al. Myeloid p38 activation maintains macrophage-liver crosstalk and BAT thermogenesis through IL-12-FGF21 axis[J]. Hepatology, 2023, 77( 3): 874- 887. DOI: 10.1002/hep.32581. |
| [33] |
LI ST, ZHOU B, XUE M, et al. Macrophage-specific FGF12 promotes liver fibrosis progression in mice[J]. Hepatology, 2023, 77( 3): 816- 833. DOI: 10.1002/hep.32640. |
| [34] |
HAN JQ, ZHANG X, LAU JK, et al. Bone marrow-derived macrophage contributes to fibrosing steatohepatitis through activating hepatic stellate cells[J]. J Pathol, 2019, 248( 4): 488- 500. DOI: 10.1002/path.5275. |
| [35] |
TANG JJ, YAN ZJ, FENG QY, et al. The roles of neutrophils in the pathogenesis of liver diseases[J]. Front Immunol, 2021, 12: 625472. DOI: 10.3389/fimmu.2021.625472. |
| [36] |
SAIJOU E, ENOMOTO Y, MATSUDA M, et al. Neutrophils alleviate fibrosis in the CCl(4)-induced mouse chronic liver injury model[J]. Hepatol Commun, 2018, 2( 6): 703- 717. DOI: 10.1002/hep4.1178. |
| [37] |
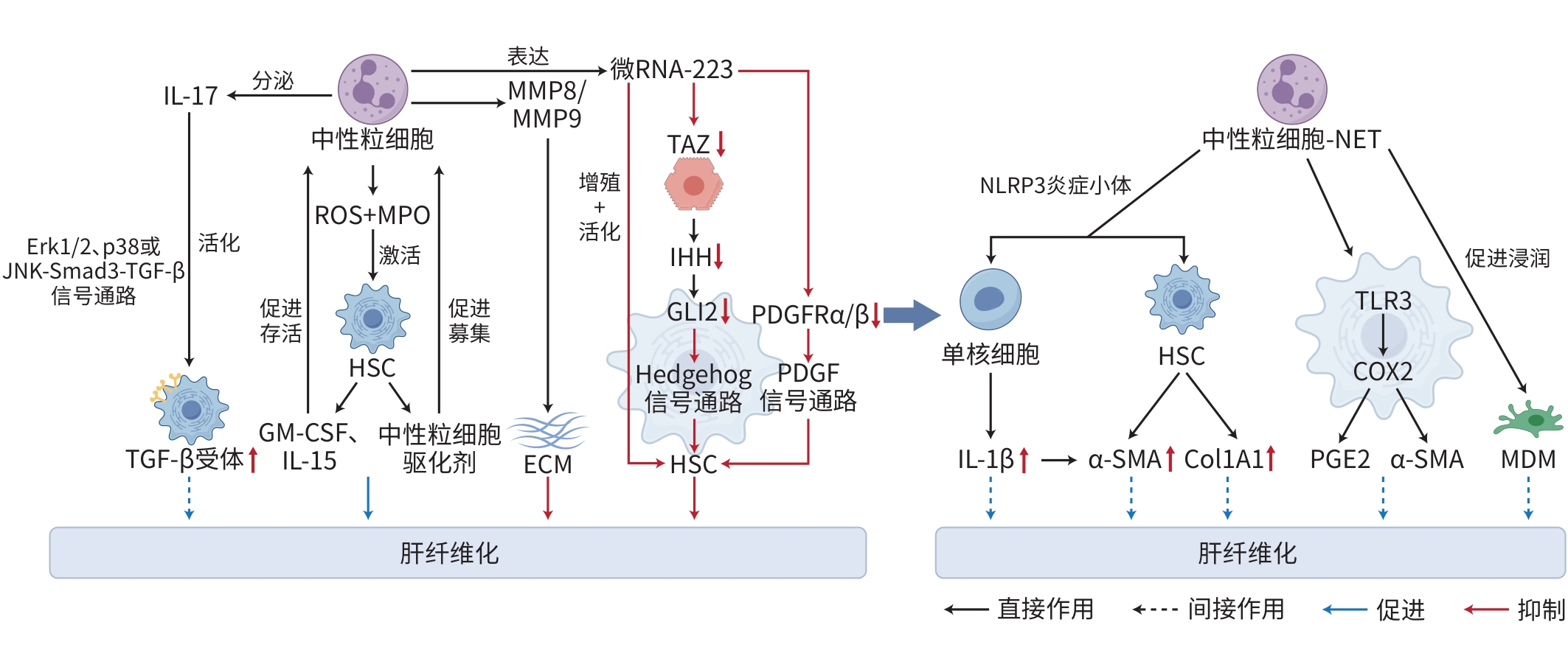
WANG XL, SEO W, PARK SH, et al. microRNA-223 restricts liver fibrosis by inhibiting the TAZ-IHH-GLI2 and PDGF signaling pathways via the crosstalk of multiple liver cell types[J]. Int J Biol Sci, 2021, 17( 4): 1153- 1167. DOI: 10.7150/ijbs.58365. |
| [38] |
|
| [39] |
BABUTA M, MOREL C, DE CARVALHO RIBEIRO M, et al. Neutrophil extracellular traps activate hepatic stellate cells and monocytes via NLRP3 sensing in alcohol-induced acceleration of MASH fibrosis[J]. Gut, 2024, 73( 11): 1854- 1869. DOI: 10.1136/gutjnl-2023-331447. |
| [40] |
XIA YJ, WANG Y, XIONG Q, et al. Neutrophil extracellular traps promote MASH fibrosis by metabolic reprogramming of HSC[J]. Hepatology, 2025, 81( 3): 947- 961. DOI: 10.1097/HEP.0000000000000762. |
| [41] |
van der WINDT DJ, SUD V, ZHANG HJ, et al. Neutrophil extracellular traps promote inflammation and development of hepatocellular carcinoma in nonalcoholic steatohepatitis[J]. Hepatology, 2018, 68( 4): 1347- 1360. DOI: 10.1002/hep.29914. |
| [42] |
ZHOU ZJ, LAI PH, ZHANG SL, et al. The relationship between hepatic myeloid-derived suppressor cells and clinicopathological parameters in patients with chronic liver disease[J]. Biomed Res Int, 2021, 2021: 6612477. DOI: 10.1155/2021/6612477. |
| [43] |
LI TY, YANG Y, ZHOU G, et al. Immune suppression in chronic hepatitis B infection associated liver disease: A review[J]. World J Gastroenterol, 2019, 25( 27): 3527- 3537. DOI: 10.3748/wjg.v25.i27.3527. |
| [44] |
SENDO S, SAEGUSA J, MORINOBU A. Myeloid-derived suppressor cells in non-neoplastic inflamed organs[J]. Inflamm Regen, 2018, 38: 19. DOI: 10.1186/s41232-018-0076-7. |
| [45] |
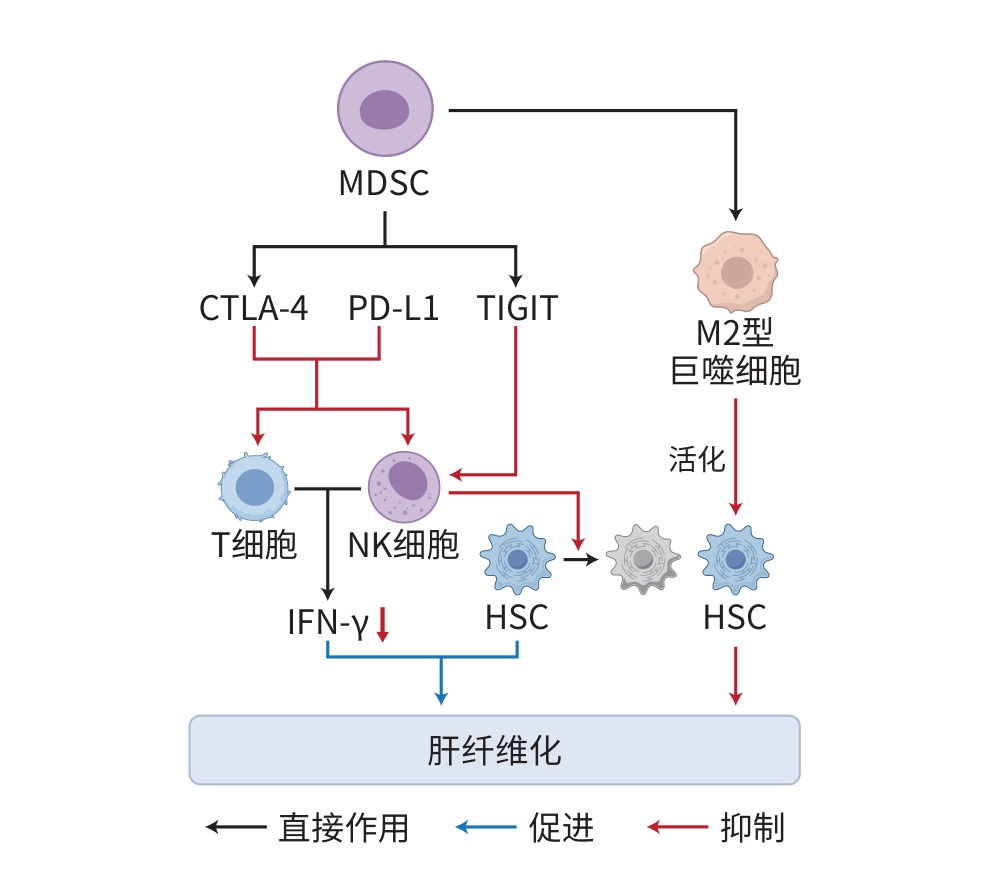
JI B. Study on the mechanism of myeloid suppressor cells in the occurrence of liver fibrosis in mice[D]. Changchun: Jilin University, 2013.
纪柏. 髓样抑制细胞在小鼠肝纤维化发生中的影响机制研究[D]. 长春: 吉林大学, 2013.
|
| [46] |
GUO FY, WANG DW. Research advances on pathogenesis of liver fibrosis and related therapeutic drugs[J]. Prog Pharm Sci, 2024, 48( 11): 838- 848. DOI: 10.20053/j.issn1001-5094.2024.11.004. |
| [47] |
SHEN B, LU LG. Mechanism and therapeutic strategy of macrophage myeloid-epithelial-reproductive tyrosine kinase promoting NASH fibrosis[J]. Chin Hepatol, 2020, 25( 10): 1021- 1023. DOI: 10.14000/j.cnki.issn.1008-1704.2020.10.002. |
| [48] |
XU J, JIN WL, LI X. A new perspective in the treatment of liver fibrosis: Targeting macrophage metabolism[J]. J Clin Hepatol, 2023, 39( 4): 922- 928. DOI: 10.3969/j.issn.1001-5256.2023.04.027. |







 DownLoad:
DownLoad: