| [1] |
KAWAIDA H, KONO H, HOSOMURA N, et al. Surgical techniques and postoperative management to prevent postoperative pancreatic fistula after pancreatic surgery[J]. World J Gastroenterol, 2019, 25( 28): 3722- 3737. DOI: 10.3748/wjg.v25.i28.3722. |
| [2] |
SØREIDE K, LABORI KJ. Risk factors and preventive strategies for postoperative pancreatic fistula after pancreatic surgery: a comprehensive review[EB/OL].[ 2024-05-07]. https://www.tandfonline.com/doi/full/10.3109/00365521.2016.1169317. DOI: 10.3109/00365521.2016.1169317 |
| [3] |
BASSI C, MARCHEGIANI G, DERVENIS C, et al. The 2016 update of the international study group(ISGPS) definition and grading of postoperative pancreatic fistula: 11 years after[J]. Surgery, 2017, 161( 3): 584- 591. DOI: 10.1016/j.surg.2016.11.014. |
| [4] |
WU HR, ZHANG H, DUAN XH, et al. Complications after laparoscopic pancreaticoduodenectomy and establishment of predicting model for postoperative pancreatic fistula[J]. Chin J Gen Surg, 2020, 35( 11): 838- 842. DOI: 10.3760/cma.j.cn113855-20200211-00071. |
| [5] |
LEE W, PARK HJ, LEE HJ, et al. Deep learning-based prediction of post-pancreaticoduodenectomy pancreatic fistula[J]. Sci Rep, 2024, 14( 1): 5089. DOI: 10.1038/s41598-024-51777-2. |
| [6] |
FUJII T, YAMADA S, MUROTANI K, et al. Oral food intake versus fasting on postoperative pancreatic fistula after distal pancreatectomy: A multi-institutional randomized controlled trial[J]. Medicine, 2015, 94( 52): e2398. DOI: 10.1097/MD.0000000000002398. |
| [7] |
MOONS KGM, de GROOT JAH, BOUWMEESTER W, et al. Critical appraisal and data extraction for systematic reviews of prediction modelling studies: The CHARMS checklist[J]. PLoS Med, 2014, 11( 10): e1001744. DOI: 10.1371/journal.pmed.1001744. |
| [8] |
WOLFF RF, MOONS KGM, RILEY RD, et al. PROBAST: A tool to assess the risk of bias and applicability of prediction model studies[J]. Ann Intern Med, 2019, 170( 1): 51- 58. DOI: 10.7326/M18-1376. |
| [9] |
HANLEY JA, MCNEIL BJ. The meaning and use of the area under a receiver operating characteristic(ROC) curve[J]. Radiology, 1982, 143( 1): 29- 36. DOI: 10.1148/radiology.143.1.7063747. |
| [10] |
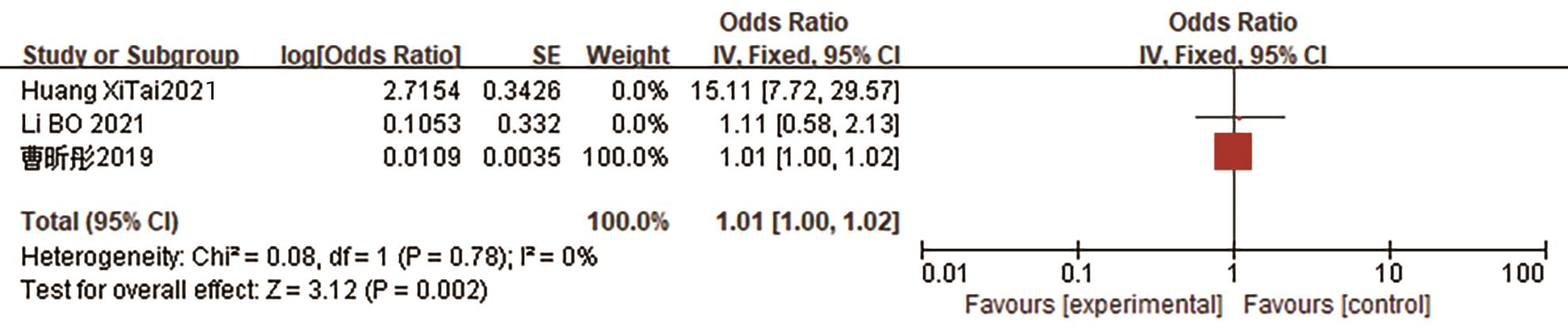
CAO XT, SHEN DC, HUANG GW, et al. A single center prospective study of screening predictive factors and building predictive model for postoperative pancreatic fistula after pancreaticoduodenectomy[J]. Chin J Gen Surg, 2019, 28( 9): 1115- 1122. DOI: 10.7659/j.issn.1005-6947.2019.09.013. |
| [11] |
CHEN FH. Prediction model of pancreatic fistula after laparoscopic pancreaticoduodenectomy with nomogram[D]. Fujian: Fujian Medical University, 2020.
陈富华. 腹腔镜胰十二指肠切除术后胰瘘列线图预测模型[D]. 福建: 福建医科大学, 2020.
|
| [12] |
CHEN LJ, LI WB, TANG ZG, et al. The value of risk model based on CT radiomics in predicting postoperative pancreatic fistula following pancreaticoduodenectomy[J]. J Hepatopancreatobiliary Surg, 2022, 34( 11): 667- 673. DOI: 10.11952/j.issn.1007-1954.2022.11.007. |
| [13] |
GUAN QC. Risk factors and risk prediction of pancreatic fistula after laparoscopic pancreatoduodenectomy[D]. Changchun: Jilin University, 2020.
管清春. 腹腔镜胰十二指肠切除术后胰瘘的危险因素分析及风险预测[D]. 长春: 吉林大学, 2020.
|
| [14] |
JIN JK. Study on risk factors and risk prediction of clinically relevant pancreatic fistula after laparoscopic pancreatoduodenectomy[D]. Wuhan: Huazhong University of Science and Technology, 2019.
金继宽. 腹腔镜胰十二指肠切除术后临床相关性胰瘘危险因素及风险预测研究[D]. 武汉: 华中科技大学, 2019.
|
| [15] |
LI K. Screening of predictors of clinically relevant pancreatic fistula after pancreaticoduodenectomy and construction of predictive model[D]. Nanchang: Nanchang University, 2020.
李轲. 胰十二指肠切除术后临床相关胰瘘预测因素的筛选与预测模型的构建[D]. 南昌: 南昌大学, 2020.
|
| [16] |
LIU SD. Risk factors analysis and risk prediction of pancreatic fistula after pancreatoduodenectomy[D]. Taiyuan: Shanxi Medical University, 2020.
刘少东. 胰十二指肠切除术后胰瘘危险因素分析及风险预测[D]. 太原: 山西医科大学, 2020.
|
| [17] |
LIU XY, ZHENG C, CHEN X, et al. Development and validation of pancreatic fistula risk prediction model after laparoscopic pancreaticoduodenectomy[J]. Chin J Lab Diagn, 2023, 27( 2): 204- 209. DOI: 10.3969/j.issn.1007-4287.2023.02.021. |
| [18] |
WU N, REN ZQ, ZHANG PB, et al. Risk factors and risk prediction of pancreatic fistula after pancreatoduodenectomy[J]. Anhui Med Pharm J, 2019, 23( 7): 1380- 1383. DOI: 10.3969/j.issn.1009-6469.2019.07.027. |
| [19] |
XIA WZ. Establishment and clinical verification of risk assessment model of pancreatic fistula after pancreatoduodenectomy[D]. Guangzhou: Southern Medical University, 2019.
夏武政. 胰十二指肠切除术后胰瘘风险评估模型的建立和临床验证[D]. 广州: 南方医科大学, 2019.
|
| [20] |
YU J, REN CY, CUI W, et al. Establishment of a risk prediction model for pancreatic fistula after pancreaticoduodenectomy: A study based on the 2016 edition of the definition and classification system of pancreatic fistula[J]. J Clin Hepatol, 2024, 40( 4): 773- 781. DOI: 10.12449/JCH240421. 余俊, 任超逸, 崔巍, 等. 胰十二指肠切除术后胰瘘风险预测模型的建立: 基于2016新版胰瘘定义及分级系统[J]. 临床肝胆病杂志, 2024, 40( 4): 773- 781. DOI: 10.12449/JCH240421. |
| [21] |
ZHANG C, ZHANG PB, ZHANG XZ, et al. Value of single factor combined with multi-factor risk screening model in risk prediction of pancreatic fistula after pancreaticoduodenectomy[J]. Shandong Med J, 2016, 56( 41): 56- 58. DOI: 10.3969/j.issn.1002-266X.2016.41.018. |
| [22] |
ZHANG JW, HE CC, WANG CH. Construction and validation of a risk prediction model for pancreatic fistula after pancreaticoduodenectomy[J]. Chin J Endocr Surg, 2023, 17( 3): 268- 272. DOI: 10.3760/cma.j.cn.115807-20220104-00001. |
| [23] |
AKGUL O, MERATH K, MEHTA R, et al. Postoperative pancreatic fistula following pancreaticoduodenectomy-stratification of patient risk[J]. J Gastrointest Surg, 2019, 23( 9): 1817- 1824. DOI: 10.1007/s11605-018-4045-x. |
| [24] |
CHOI M, LEE JH, ROH YH, et al. Multidimensional nomogram to predict postoperative pancreatic fistula after minimally invasive pancreaticoduodenectomy[J]. Ann Surg Oncol, 2023, 30( 8): 5083- 5090. DOI: 10.1245/s10434-023-13360-3. |
| [25] |
NAKEEB A EL, SALAH T, SULTAN A, et al. Pancreatic anastomotic leakage after pancreaticoduodenectomy. Risk factors, clinical predictors, and management(single center experience)[J]. World J Surg, 2013, 37( 6): 1405- 1418. DOI: 10.1007/s00268-013-1998-5. |
| [26] |
GU ZT, DU YX, WANG P, et al. Development and validation of a novel nomogram to predict postoperative pancreatic fistula after pancreatoduodenectomy using lasso-logistic regression: An international multi-institutional observational study[J]. Int J Surg, 2023, 109( 12): 4027- 4040. DOI: 10.1097/JS9.0000000000000695. |
| [27] |
GUO CX, SHEN YN, ZHANG Q, et al. Prediction of postoperative pancreatic fistula using a nomogram based on the updated definition[J]. Ann Surg Treat Res, 2020, 98( 2): 72- 81. DOI: 10.4174/astr.2020.98.2.72. |
| [28] |
HUANG XT, HUANG CS, LIU C, et al. Development and validation of a new nomogram for predicting clinically relevant postoperative pancreatic fistula after pancreatoduodenectomy[J]. World J Surg, 2021, 45( 1): 261- 269. DOI: 10.1007/s00268-020-05773-y. |
| [29] |
LI B, PU N, CHEN QD, et al. Comprehensive diagnostic nomogram for predicting clinically relevant postoperative pancreatic fistula after pancreatoduodenectomy[J]. Front Oncol, 2021, 11: 717087. DOI: 10.3389/fonc.2021.717087. |
| [30] |
LI Y, ZHOU F, ZHU DM, et al. Novel risk scoring system for prediction of pancreatic fistula after pancreaticoduodenectomy[J]. World J Gastroenterol, 2019, 25( 21): 2650- 2664. DOI: 10.3748/wjg.v25.i21.2650. |
| [31] |
MAQUEDA GONZÁLEZ R, DI MARTINO M, GALÁN GONZÁLEZ I, et al. Development of a prediction model of pancreatic fistula after duodenopancreatectomy and soft pancreas by assessing the preoperative image[J]. Langenbecks Arch Surg, 2022, 407( 6): 2363- 2372. DOI: 10.1007/s00423-022-02564-y. |
| [32] |
SHI Y, GAO F, QI YF, et al. Computed tomography-adjusted fistula risk score for predicting clinically relevant postoperative pancreatic fistula after pancreatoduodenectomy: Training and external validation of model upgrade[J]. EBioMedicine, 2020, 62: 103096. DOI: 10.1016/j.ebiom.2020.103096. |
| [33] |
GUO XJ, ZHU F, YANG MW, et al. A score model based on pancreatic steatosis and fibrosis and pancreatic duct diameter to predict postoperative pancreatic fistula after pancreatoduodenectomy[J]. BMC Surg, 2019, 19( 1): 75. DOI: 10.1186/s12893-019-0534-4. |
| [34] |
YAMAMOTO Y, SAKAMOTO Y, NARA S, et al. A preoperative predictive scoring system for postoperative pancreatic fistula after pancreaticoduodenectomy[J]. World J Surg, 2011, 35( 12): 2747- 2755. DOI: 10.1007/s00268-011-1253-x. |
| [35] |
YOU Y, HAN IW, CHOI DW, et al. Nomogram for predicting postoperative pancreatic fistula[J]. HPB(Oxford), 2019, 21( 11): 1436- 1445. DOI: 10.1016/j.hpb.2019.03.351. |
| [36] |
YU J, REN CY, WANG J, et al. Establishment of risk prediction model of postoperative pancreatic fistula after pancreatoduodenectomy: 2016 edition of definition and grading system of pancreatic fistula: A single center experience with 223 cases[J]. World J Surg Oncol, 2021, 19( 1): 257. DOI: 10.1186/s12957-021-02372-6. |
| [37] |
ZHANG JY, HUANG J, ZHAO SY, et al. Risk factors and a new prediction model for pancreatic fistula after pancreaticoduodenectomy[J]. Risk Manag Healthc Policy, 2021, 14: 1897- 1906. DOI: 10.2147/RMHP.S305332. |
| [38] |
ZHU YW, WU D, YANG H, et al. Analysis of factors influencing pancreatic fistula after minimally invasive pancreaticoduodenectomy and establishment of a new prediction model for clinically relevant pancreatic fistula[J]. Surg Endosc, 2024, 38( 5): 2622- 2631. DOI: 10.1007/s00464-024-10770-6. |
| [39] |
XU XB, JIA CP, JIA Y, et al. Construction and application value of prediction model of pancreatic fistula after pancreaticoduodenectomy[J]. Chin J Dig Surg, 2020, 19( 4): 408- 413. DOI: 10.3760/cma.j.cn115610-20200409-00240. |
| [40] |
ZHANG ZH. Research on risk factors and clinical prediction model of pancreatic fistula after pancreaticoduodenectomy based on machine learning[D]. Beijing: Peking Union Medical College, 2023.
张子欢. 基于机器学习的胰十二指肠切除术发生胰瘘的危险因素及临床预测模型研究[D]. 北京: 北京协和医学院, 2023.
|
| [41] |
ZHANG DY, LEI P, ZHANG YB, et al. Construction and validation of a risk prediction model for clinically relevant pancreatic fistula after pancreaticoduodenectomy[J]. China J Gen Surg, 2024, 33( 3): 366- 375. DOI: 10.7659/j.issn.1005-6947.2024.03.007. |
| [42] |
ZHOU LC. Establishment and verification of prediction model of pancreatic fistula after pancreatoduodenectomy[D]. Luzhou: Southwest Medical University, 2023.
周黎晨. 胰十二指肠切除术后胰瘘预测模型建立与验证[D]. 泸州: 西南医科大学, 2023.
|
| [43] |
CHEN YR, TIAN XD, XIE XH, et al. Risk factors of postoperative pancreatic fistula after pancreaticoduodenectomy and its predictive score[J]. Chin J Surg, 2016, 54( 1): 39- 43. DOI: 10.3760/cma.j.issn.0529-5815.2016.01.010. |
| [44] |
GROUP PS, COMMITTEE W, PANDE R, et al. External validation of postoperative pancreatic fistula prediction scores in pancreatoduodenectomy: A systematic review and meta-analysis[J]. HPB(Oxford), 2022, 24( 3): 287- 298. DOI: 10.1016/j.hpb.2021.10.006. |
| [45] |
van der PLOEG T, AUSTIN PC, STEYERBERG EW. Modern modelling techniques are data hungry: A simulation study for predicting dichotomous endpoints[J]. BMC Med Res Methodol, 2014, 14: 137. DOI: 10.1186/1471-2288-14-137. |
| [46] |
CHEN XP, ZHANG Y, ZHUANG YY, et al. PROBAST: A tool for assessing risk of bias in the study of diagnostic or prognostic multi-factorial predictive models[J]. Chin J Evid Based Med, 2020, 20( 6): 737- 744. DOI: 10.7507/1672-2531.201910087. |
| [47] |
RANALLI MG, SALVATI N, PETRELLA L, et al. M-quantile regression shrinkage and selection via the Lasso and Elastic Net to assess the effect of meteorology and traffic on air quality[J]. Biom J, 2023, 65( 8): e2100355. DOI: 10.1002/bimj.202100355. |
| [48] |
ZHANG Q, YUAN KH, WANG LJ. Asymptotic bias of normal-distribution-based maximum likelihood estimates of moderation effects with data missing at random[J]. Br J Math Stat Psychol, 2019, 72( 2): 334- 354. DOI: 10.1111/bmsp.12151. |
| [49] |
ZHOU CY, YAO LB. Biochemistry and molecular biology[M]. 9th ed. Beijing: People’s Medical Publishing House, 2018: 350- 351.
周春燕, 药立波. 生物化学与分子生物学[M]. 9版. 北京: 人民卫生出版社, 2018: 350- 351.
|
| [50] |
SLEEP D. Albumin and its application in drug delivery[J]. Expert Opin Drug Deliv, 2015, 12( 5): 793- 812. DOI: 10.1517/17425247.2015.993313. |
| [51] |
YANG JX, YE SY, DAI D. Risk factors and preventive measures for postoperative pancreatic fistula after pancreaticoduodenectomy[J]. World Chin J Dig, 2020, 28( 18): 914- 919. DOI: 10.11569/wcjd.v28.i18.914. |
| [52] |
WANG XL, TU YY, WANG W, et al. Risk factors for pancreatic fistula after pancreaticoduodenectomy[J]. J Clin Hepatol, 2017, 33( 1): 116- 120. DOI: 10.3969/j.issn.1001-5256.2017.01.025. |
| [53] |
Chinese Society of Endoscopy, Chinese Medical Association; Endoscopic Physician Branch of Chinese Medical Doctor Association; Beijing Society of Digestive Endoscopy, Beijing Medical Association. Chinese expert consensus on the endoscopic diagnosis and treatment of pancreatic fistula(2020, Beijing)[J]. J Clin Hepatol, 2021, 37( 4): 803- 808. DOI: 10.3969/j.issn.1001-5256.2021.04.016. |
| [54] |
HE CC, WANG CH, TANG YF. Research status of abdominal drainage after pancreaticoduodenectomy[J]. Chin J Med Offic, 2022, 50( 1): 99- 101, 105. DOI: 10.16680/j.1671-3826.2022.01.31. |
| [55] |
HALLE-SMITH JM, VINUELA E, BROWN RM, et al. A comparative study of risk factors for pancreatic fistula after pancreatoduodenectomy or distal pancreatectomy[J]. HPB(Oxford), 2017, 19( 8): 727- 734. DOI: 10.1016/j.hpb.2017.04.013. |
| [56] |
RILEY RD, ENSOR J, SNELL KIE, et al. Calculating the sample size required for developing a clinical prediction model[J]. BMJ, 2020, 368: m441. DOI: 10.1136/bmj.m441. |







 DownLoad:
DownLoad: