妊娠合并罗托综合征1例报告
DOI: 10.12449/JCH260321
-
摘要: 罗托综合征是一种常染色体隐性胆红素代谢障碍性疾病,因其极为罕见且临床表现缺乏特异性,难以诊断和鉴别。近年来,基因检测技术的发展为不典型患者的早期诊断提供了可能。经检索,目前仅有19例详尽临床及遗传数据的病例被报道。本文报道了1例妊娠期间以直接胆红素水平升高为主、溶质载体有机阴离子转运蛋白家族成员1B1/1B3双基因纯合突变诊断为罗托综合征并成功分娩的孕妇,并对相关文献进行回顾性分析,旨在从遗传机制角度探讨罗托综合征的早期精准诊断与用药策略。Abstract: Rotor syndrome is an autosomal recessive disorder of bilirubin metabolism, and it is difficult to diagnose and differentiate due to its extreme rarity and a lack of specific clinical manifestations. In recent years, the development of genetic testing technology has enabled the early diagnosis of atypical patients. Literature search shows that only 19 cases with detailed clinical and genetic data have been reported. This article reports a case of a pregnant woman with an increase in direct bilirubin during pregnancy who was diagnosed with Rotor syndrome based on a bi-allelic mutation in the SLCO1B1 and SLCO1B3 genes and delivered successfully at last, and a retrospective analysis was performed for related articles, in order to facilitate the early accurate diagnosis of patients with Rotor syndrome and guide medications from the perspective of genetic mechanisms.
-
Key words:
- Rotor Syndrome /
- Pregnancy /
- Diagnosis
-
表 1 患者历次胆红素数据
Table 1. Patient’s historical bilirubin data
次数 妊娠 日期 TBil(μmol/L) DBil(μmol/L) IBil(μmol/L) DBil/TBil(%) 1 无 2021/09/10 95.01 41.10 53.91 43.26 2 无 2021/12/02 101.90 46.40 55.50 45.53 3 无 2022/07/11 74.70 31.90 42.80 42.70 4 无 2023/07/15 90.40 40.30 50.10 44.58 5 孕30周+5天 2024/10/23 120.13 61.64 58.49 51.31 6 孕38周+5天 2024/12/18 127.88 69.23 58.65 54.14 7 产后0周+4天 2024/12/25 119.25 67.36 51.89 56.93 8 产后6周+4天 2025/02/06 125.67 65.53 60.14 52.14 注:TBil,总胆红素;DBil,直接胆红素;IBil,间接胆红素。
表 2 新生儿TcB测定结果
Table 2. Results of neonatal transcutaneous bilirubin measurements
时间(h) TcB(mg/dL) 时间(h) TcB(mg/dL) 24×0+0 1.2 24×3+0 12.0 24×0+6 5.4 24×3+6 11.9 24×0+12 6.5 24×3+12 12.1 24×0+18 6.1 24×3+18 12.0 24×1+0 8.5 24×4+0 11.8 24×1+6 9.0 24×4+6 11.6 24×1+12 10.6 24×4+12 11.9 24×1+18 9.8 24×4+18 12.4 24×2+0 9.1 24×5+0 11.3 24×2+6 10.3 25×5+6 11.5 24×2+12 11.0 25×5+12 11.2 24×2+18 10.8 24×5+18 — 注:TcB,经皮胆红素。
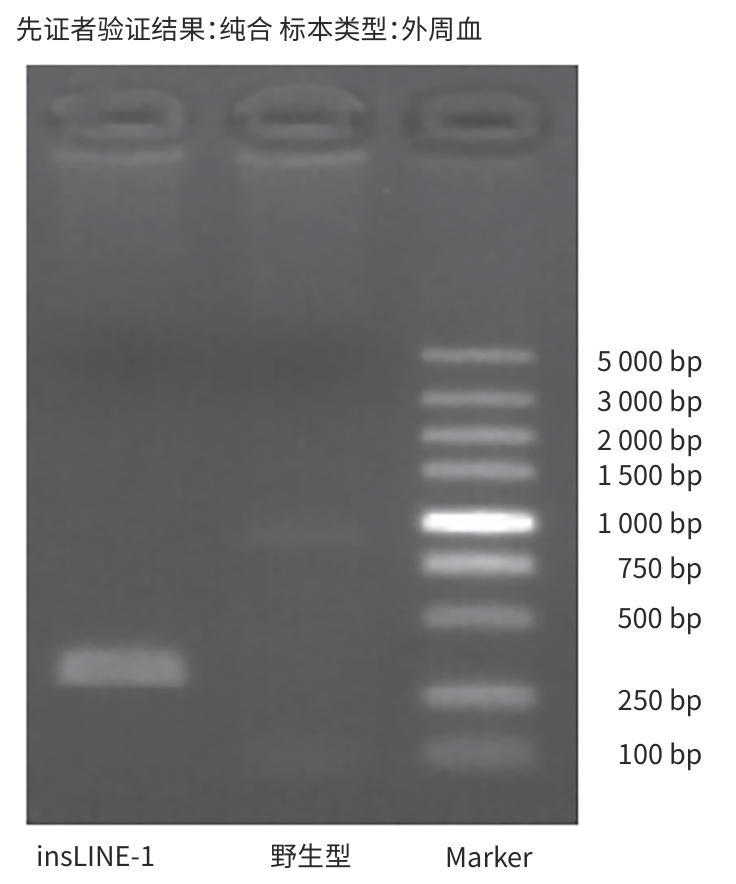
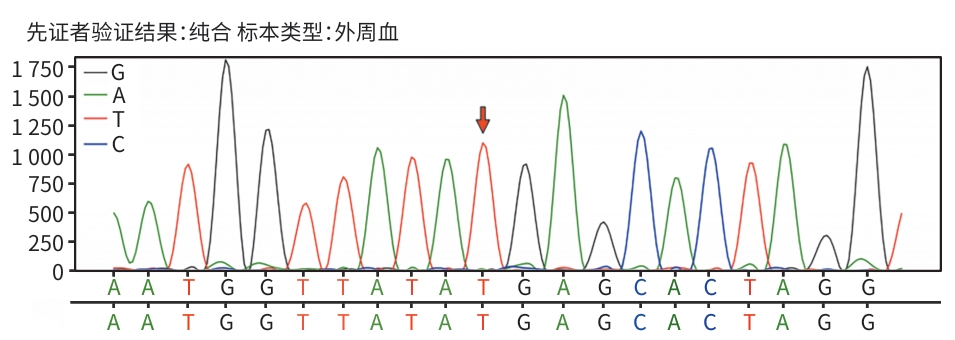
表 3 与受检者临床信息相关的致病变异或可疑变异
Table 3. Pathogenic or suspected variants associated with clinical information about the subject
基因(组) 染色体位置hg19 变异命名 人群频率 合子状态 ACMG分类 关联疾病 SLCO1B3 chr12:21014093-
21014094NM_019844
intron5
insLINE-1— 纯合 致病 罗托型高胆红素血症(237450,
DR)SLCO1B1 chr12:21375289
C>TNM_006446.5
exon13
c.1738C>T
p.R580*0.004 241 67 纯合 致病 罗托型高胆红素血症(237450,
DR)UGT1A1 chr2:234669144
G>ANM_000463.3
exon1
c.211G>A
p.G71R0.153 8 杂合 疾病相关
多态位点家族性暂时新生儿高胆红素血
症(237900,AD,AR)、克里格勒-
纳贾尔综合征Ⅰ型(218800,
AR)、克里格勒-纳贾尔综合征Ⅱ
型(606785,AR)、吉尔伯特综合
征(143500,AR)NPC2 chr14:74947448
T>CNM_006432.5 exon4
c.398A>G p.D133G— 杂合 意义不
明确尼曼-匹克病C2型(607625,AR) 注:ACMG,美国医学遗传学与基因组学学会;SLCO1B3,溶质载体有机阴离子转运蛋白家族成员1B3基因;SLCO1B1,溶质载体有机阴离子转运蛋白家族成员1B1基因;UGT1A1,尿苷二磷酸葡萄糖醛酸转移酶1A1基因;NPC2,尼曼-匹克病C型细胞内胆固醇转运蛋白2基因;DR,双基因隐性遗传;AD,常染色体显性遗传;AR,常染色体隐性遗传。
-
[1] BAI J, ZHENG SJ, DUAN ZP. Clinical features and diagnosis of four common types of congenital hyperbilirubinemia[J]. J Clin Hepatol, 2019, 35( 8): 1680- 1683. DOI: 10.3969/j.issn.1001-5256.2019.08.005.白洁, 郑素军, 段钟平. 4种常见先天性高胆红素血症的临床特征及诊断思路[J]. 临床肝胆病杂志, 2019, 35( 8): 1680- 1683. DOI: 10.3969/j.issn.1001-5256.2019.08.005. [2] LI W. Research progress in diagnosis of hereditary hyperbilirubinemia by gene sequencing[J]. J Med Inf, 2021, 34( 16): 64- 67. DOI: 10.3969/j.issn.1006-1959.2021.16.018.李伟. 基因测序诊断遗传性高胆红素血症的研究进展[J]. 医学信息, 2021, 34( 16): 64- 67. DOI: 10.3969/j.issn.1006-1959.2021.16.018. [3] MEMON N, WEINBERGER BI, HEGYI T, et al. Inherited disorders of bilirubin clearance[J]. Pediatr Res, 2016, 79( 3): 378- 386. DOI: 10.1038/pr.2015.247. [4] MORAIS MB, MACHADO MV. Benign inheritable disorders of bilirubin metabolism manifested by conjugated hyperbilirubinemia-A narrative review[J]. United European Gastroenterol J, 2022, 10( 7): 745- 753. DOI: 10.1002/ueg2.12279. [5] LU J, LI W, LIU Y. Research advances in congenital non-hemolytic jaundice[J]. J Clin Hepatol, 2021, 37( 1): 216- 220. DOI: 10.3969/j.issn.1001-5256.2021.01.048.鲁杰, 李武, 刘叶. 先天性非溶血性黄疸的研究进展[J]. 临床肝胆病杂志, 2021, 37( 1): 216- 220. DOI: 10.3969/j.issn.1001-5256.2021.01.048. [6] van de STEEG E, STRÁNECKÝ V, HARTMANNOVÁ H, et al. Complete OATP1B1 and OATP1B3 deficiency causes human Rotor syndrome by interrupting conjugated bilirubin reuptake into the liver[J]. J Clin Invest, 2012, 122( 2): 519- 528. DOI: 10.1172/JCI59526. [7] CHENG YY, CHANG KC, CHEN PL, et al. SLCO1B1 and SLCO1B3 genetic mutations in Taiwanese patients with Rotor syndrome[J]. J Formos Med Assoc, 2023, 122( 7): 648- 652. DOI: 10.1016/j.jfma.2023.03.003. [8] LIN LZ, WU QY, ZHANG JH, et al. A pedigree analysis of Rotor hyperbilirubinemia combined with hepatitis B virus infection in a SLCO1B1 and SLCO1B3 gene mutations patient[J]. Heliyon, 2024, 10( 13): e33864. DOI: 10.1016/j.heliyon.2024.e33864. [9] WANG J. Analysis of 9 families with congenital nonhemolytic jaundice abstract[D]. Tianjin: Tianjin Medical University, 2021. DOI: 10.27366/d.cnki.gtyku.2021.001428.王婧. 先天性非溶血性黄疸9例家系分析[D]. 天津: 天津医科大学, 2021. DOI: 10.27366/d.cnki.gtyku.2021.001428. [10] YE JW, TAN LM, YANG FX, et al. Analysis of clinical feature and SLCO1B1 and SLC01B3 gene mutations in children with Rotor syndrome[J]. Guangzhou Med J, 2021, 52( 6): 1- 5. DOI: 10.3969/j.issn.1000-8535.2021.06.001.叶家卫, 谭丽梅, 杨峰霞, 等. 儿童Rotor综合征临床特点及SLCO1B1和SLCO1B3基因突变分析[J]. 广州医药, 2021, 52( 6): 1- 5. DOI: 10.3969/j.issn.1000-8535.2021.06.001. [11] WANG DY, LI XB, LAI PJ, et al. Analysis of genetic variants in a case with Rotor syndrome[J]. Chin J Med Genet, 2021, 38( 4): 359- 362. DOI: 10.3760/cma.j.cn511374-20200131-00051.王大燕, 李小兵, 赖盼建, 等. 一例Rotor综合征患儿的基因变异分析[J]. 中华医学遗传学杂志, 2021, 38( 4): 359- 362. DOI: 10.3760/cma.j.cn511374-20200131-00051. [12] TAN YF, OUYANG WX, JIANG T, et al. Clinical characteristics and genetic analysis of four children with Rotor syndrome[J]. Chin J Med Genet, 2024, 41( 6): 715- 719. DOI: 10.3760/cma.j.cn511374-20220520-00342.谭艳芳, 欧阳文献, 姜涛, 等. Rotor综合征患儿4例的临床特征及遗传学分析[J]. 中华医学遗传学杂志, 2024, 41( 6): 715- 719. DOI: 10.3760/cma.j.cn511374-20220520-00342. [13] ZHANG ZH, ZHENG BX, LI M, et al. SLCO1B1 and SLCO1B3 gene mutations in a Chinese boy with Rotor syndrome: A case report[J]. Chin Hepatol, 2016, 21( 7): 542- 544, 605. DOI: 10.14000/j.cnki.issn.1008-1704.2016.07.006.张志华, 郑必霞, 李玫, 等. 一例Rotor综合征SLCO1B1和SLCO1B3基因突变分析[J]. 肝脏, 2016, 21( 7): 542- 544, 605. DOI: 10.14000/j.cnki.issn.1008-1704.2016.07.006. [14] MORAIS M, COUVERT P, JÉRU I, et al. Rotor syndrome presenting as dubin-Johnson syndrome[J]. Case Rep Gastroenterol, 2022, 16( 2): 452- 455. DOI: 10.1159/000525517. [15] ZENG XY, ZHANG T, SUN KW, et al. Rotor syndrome combined with HBsAg carriers: One case report[J]. Chin J Gastroenterol Hepatol, 2016, 25( 4): 446- 447. DOI: 10.3969/j.issn.1006-5709.2016.04.024.曾祥源, 张涛, 孙克伟, 等. Rotor综合征合并HBsAg携带者1例报道[J]. 胃肠病学和肝病学杂志, 2016, 25( 4): 446- 447. DOI: 10.3969/j.issn.1006-5709.2016.04.024. [16] DIMOPOULOU D, LYRA V, DIMOPOULOU A, et al. Is hepatobiliary scintigraphy sufficient to diagnose rotor syndrome in a 3-year-old boy?[J]. J Nucl Med Technol, 2021, 49( 2): 193- 194. DOI: 10.2967/jnmt.120.257618. [17] LI J, DENG CJ, HE SL, et al. Clinical characteristics and polymorphism of UGT1A1 gene in 53 cases of congenital hyperbilirubinemia in Yunnan[J]. J Kunming Med Univ, 2024, 45( 5): 136- 143. DOI: 10.12259/j.issn.2095-610X.S20240521.李娟, 邓成俊, 何舒丽, 等. 云南地区53例先天性高胆红素血症临床特征及UGT1A1基因多态性分析[J]. 昆明医科大学学报, 2024, 45( 5): 136- 143. DOI: 10.12259/j.issn.2095-610X.S20240521. [18] ZHANG M. Diagnostic value of UGT1A1 in Gilbert syndrome[D]. Wuhan: Huazhong University of Science and Technology, 2019. DOI: 10.27157/d.cnki.ghzku.2019.002956.张梦. UGT1A1基因检测在Gilbert综合征中的诊断价值分析[D]. 武汉: 华中科技大学, 2019. DOI: 10.27157/d.cnki.ghzku.2019.002956. [19] GEBERHIWOT T, MORO A, DARDIS A, et al. Consensus clinical management guidelines for Niemann-Pick disease type C[J]. Orphanet J Rare Dis, 2018, 13( 1): 50. DOI: 10.1186/s13023-018-0785-7. [20] ERLINGER S, ARIAS IM, DHUMEAUX D. Inherited disorders of bilirubin transport and conjugation: New insights into molecular mechanisms and consequences[J]. Gastroenterology, 2014, 146( 7): 1625- 1638. DOI: 10.1053/j.gastro.2014.03.047. [21] YEE SW, HALDAR T, KVALE M, et al. SLCO1B1 functional variants and statin-induced myopathy in people with recent genealogical ancestors from Africa: A population-based real-world study[J]. medRxiv, 2023. DOI: 10.1101/2023.12.02.23299324.[Preprint] [22] KAGAWA T, ADACHI Y, HASHIMOTO N, et al. Loss of organic anion transporting polypeptide 1B3 function causes marked delay in indocyanine green clearance without any clinical symptoms[J]. Hepatology, 2017, 65( 3): 1065- 1068. DOI: 10.1002/hep.28950. [23] KIM YG, SUNG H, SHIN HS, et al. Intronic LINE-1 insertion in SLCO1B3 as a highly prevalent cause of rotor syndrome in East Asian population[J]. J Hum Genet, 2022, 67( 2): 71- 77. DOI: 10.1038/s10038-021-00967-1. [24] CHAUBAL AN, PATEL R, CHOKSI D, et al. Management of pregnancy in Crigler Najjar syndrome type 2[J]. World J Hepatol, 2016, 8( 11): 530- 532. DOI: 10.4254/wjh.v8.i11.530. [25] BOUCHGHOUL H, BOUYER J, SENAT MV, et al. Hypoglycemia and glycemic control with glyburide in women with gestational diabetes and genetic variants of cytochrome P450 2C9 and/or OATP1B3[J]. Clin Pharmacol Ther, 2021, 110( 1): 141- 148. DOI: 10.1002/cpt.2142. [26] SUN H, FRASSETTO L, BENET LZ. Effects of renal failure on drug transport and metabolism[J]. Pharmacol Ther, 2006, 109( 1-2): 1- 11. DOI: 10.1016/j.pharmthera.2005.05.010. [27] NAUD J, MICHAUD J, LEBLOND FA, et al. Effects of chronic renal failure on liver drug transporters[J]. Drug Metab Dispos, 2008, 36( 1): 124- 128. DOI: 10.1124/dmd.107.018192. [28] KUNZE A, EDIAGE EN, DILLEN L, et al. Clinical investigation of coproporphyrins as sensitive biomarkers to predict mild to strong OATP1B-mediated drug-drug interactions[J]. Clin Pharmacokinet, 2018, 57( 12): 1559- 1570. DOI: 10.1007/s40262-018-0648-3. [29] UJIHIRA Y, TAN SPF, SCOTCHER D, et al. Genotype, ethnicity, and drug-drug interaction modeling as means of verifying transporter biomarker PBPK model: The coproporphyrin-I story[J]. CPT Pharmacometrics Syst Pharmacol, 2025, 14( 5): 941- 953. DOI: 10.1002/psp4.70008. [30] PAUL WILSON JH, SINAASAPPEL M, LOTGERING FK, et al. Recommendations for pregnancies in patients with crigler-najjar syndrome[J]. JIMD Rep, 2013, 7: 59- 62. DOI: 10.1007/8904_2012_142. -



 PDF下载 ( 1460 KB)
PDF下载 ( 1460 KB)

 下载:
下载: