Hierarchical diagnosis and treatment pathway and multidisciplinary collaborative intelligent holistic management protocol for metabolic dysfunction-associated fatty liver disease within the Hepatology Specialty Alliance framework: An integrated traditional Chinese and Western medicine approach
-
摘要: 代谢相关脂肪性肝病(MAFLD)已成为我国慢性肝病的主要病因,其与心血管疾病、2型糖尿病等多种代谢紊乱密切关联,共同构成一种复杂的全身性疾病。当前临床实践中,筛查与风险分层工具的应用缺乏标准化,跨学科协作机制亦不完善,导致MAFLD全程管理效率受限,患者预后差异显著。为应对上述挑战,本文基于肝病专科联盟体系,构建了一套科学、系统且具有可操作性的MAFLD分级诊疗与全程管理临床路径。该路径的核心内容包括:确立基于影像学与代谢异常的双维度诊断标准;明确以无创纤维化-4指数作为肝病专科联盟内初始风险分层的关键节点,联合肝脏硬度测定实现精准分流;系统制定肝病科与内分泌科、心内科、营养科等多学科间的双向转诊指征及协作流程;在强化生活方式干预基础上,整合循证药物治疗与中医辅助干预策略。此外,本文前瞻性提出以数据驱动、智能预警与全病程随访为特征的智慧化管理平台框架。本临床路径旨在为肝病专科联盟体系下各级医疗机构提供标准化MAFLD管理工具,推动从“单一肝病诊疗”向“多系统共病一体化管理”模式转变,以期最终降低肝病及心血管相关终点事件风险,改善患者长期预后。Abstract: Metabolic dysfunction-associated fatty liver disease (MAFLD) has become the leading cause of chronic liver disease in China, and it is closely intertwined with various metabolic disorders such as cardiovascular diseases and type 2 diabetes, collectively constituting a complex systemic condition. Current clinical practice still faces the challenges including non-standardized application of screening and risk stratification tools, and a lack of multidisciplinary collaboration mechanisms, which lead to inefficient holistic management of MAFLD and significant variability in prognosis. To address these challenges, this study developed a scientific, systematic, and operable clinical pathway for hierarchical diagnosis and treatment and holistic management of MAFLD based on the Hepatology Specialty Alliance framework. The core components of this pathway include the following aspects: establishing dual-dimensional diagnostic criteria based on imaging and metabolic abnormalities; defining the non-invasive fibrosis-4 index as the key node for initial risk stratification within the alliance, combined with liver stiffness measurement for precise patient triage; systematically formulating bidirectional referral indications and collaborative workflows among hepatology, endocrinology, cardiology, and nutrition departments; integrating evidence-based pharmacological therapy and traditional Chinese medicine adjuvant strategies on the basis of intensified lifestyle intervention. Furthermore, this study prospectively proposes a framework for an intelligent management platform characterized by data-driven decision-making, smart early warning, and whole-course follow-up. This clinical pathway aims to provide standardized MAFLD management tools for healthcare institutions at all levels within the Hepatology Specialty Alliance system, and it seeks to promote a shift from the model of “diagnosis and treatment of a single liver disease” to a paradigm of “integrated management of multi-system comorbidities”, in order to reduce the risk of liver diseases and cardiovascular endpoint events and improve the long-term prognosis of patients.
-
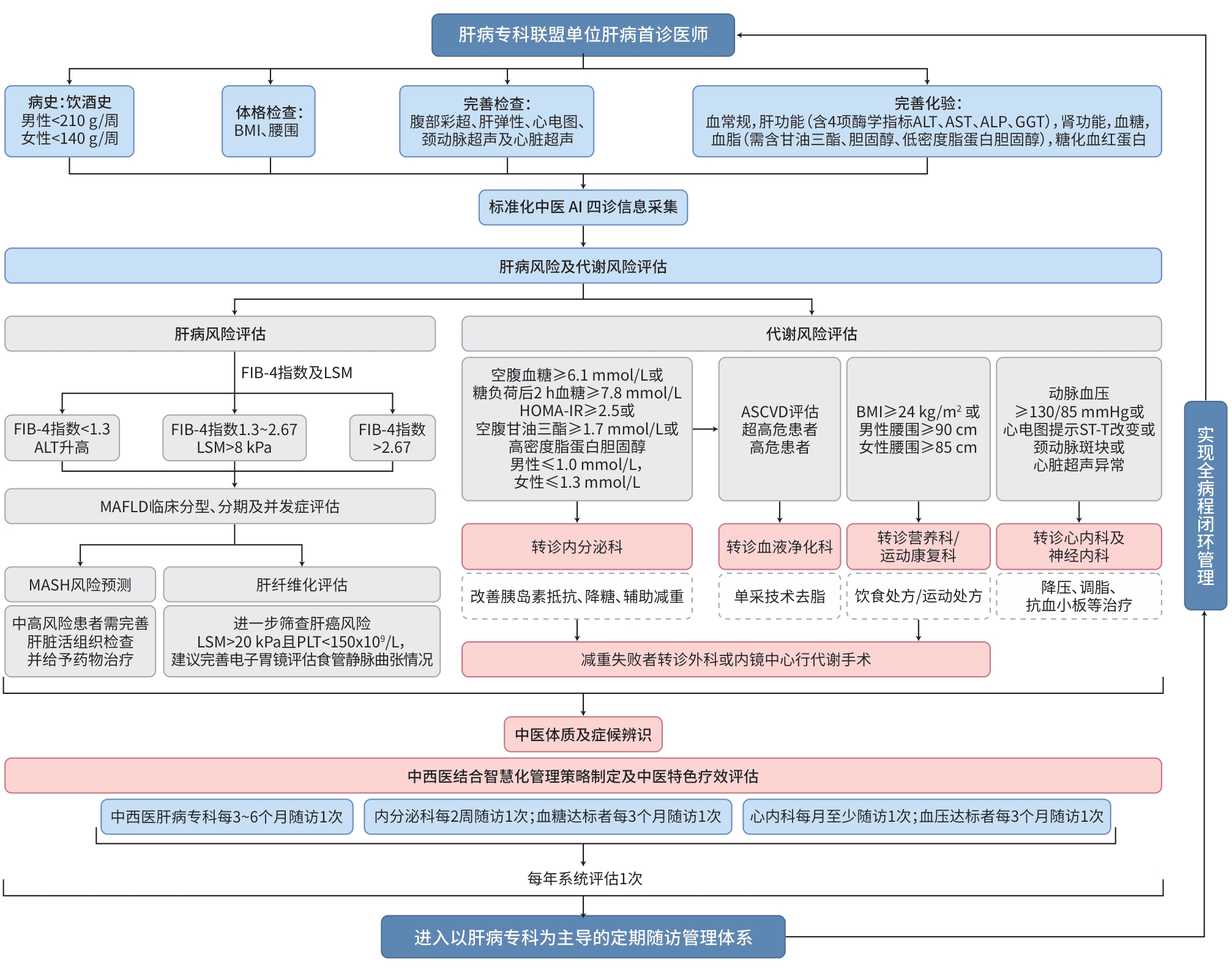
注: BMI,体重指数;ALT,丙氨酸氨基转移酶;AST,天冬氨酸氨基转移酶;ALP,碱性磷酸酶;GGT,γ-谷氨酰转移酶;AI,人工智能;FIB-4指数,纤维化-4指数;LSM,肝脏硬度测定;MAFLD,代谢相关脂肪性肝病;MASH,代谢相关脂肪性肝炎;PLT,血小板计数;HOMA-IR,胰岛素抵抗指数;ASCVD,动脉粥样硬化性心血管疾病。
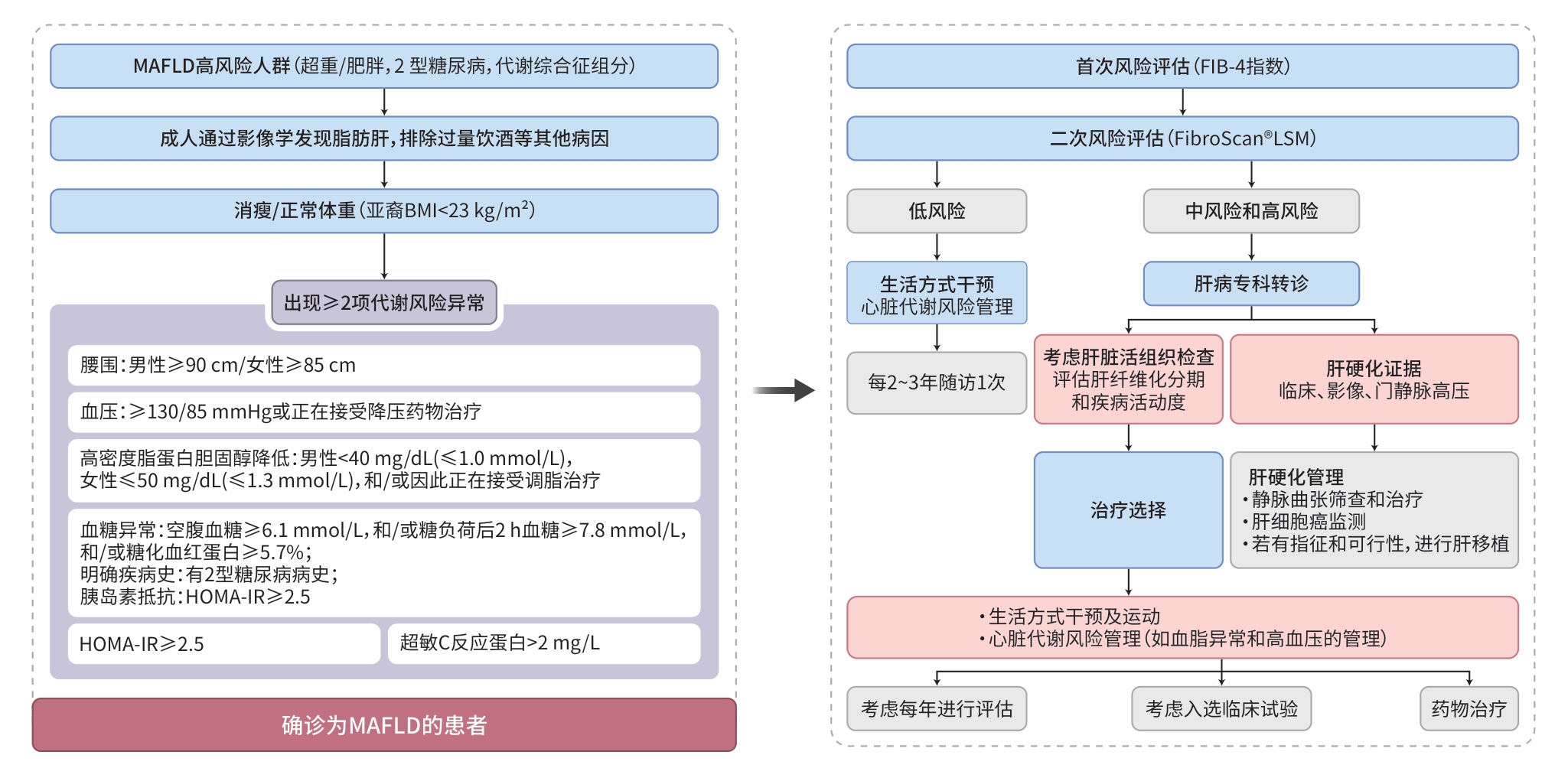
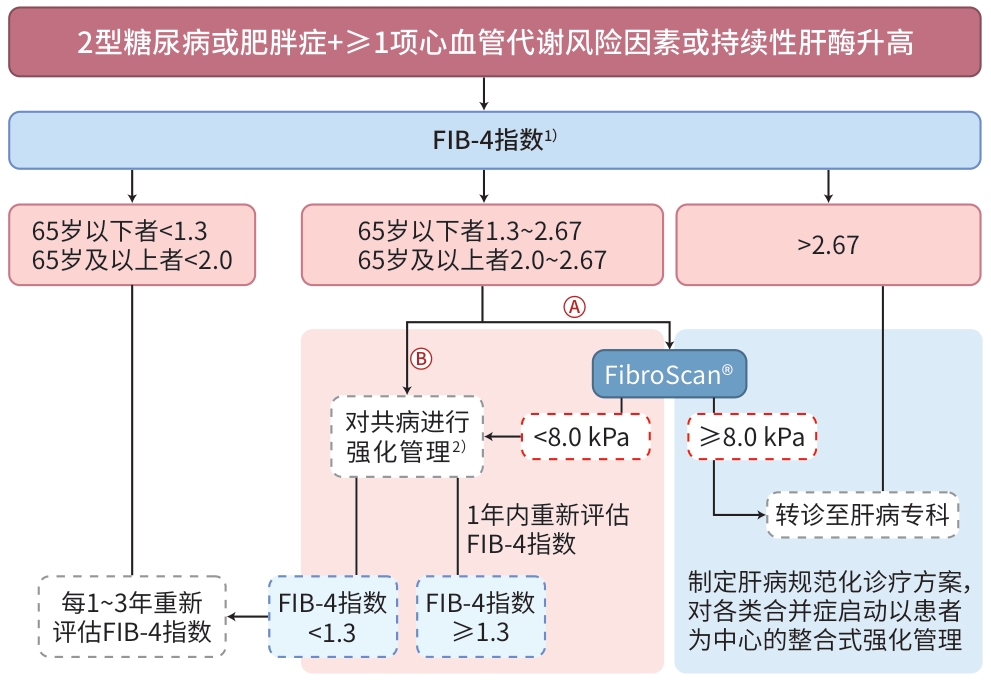
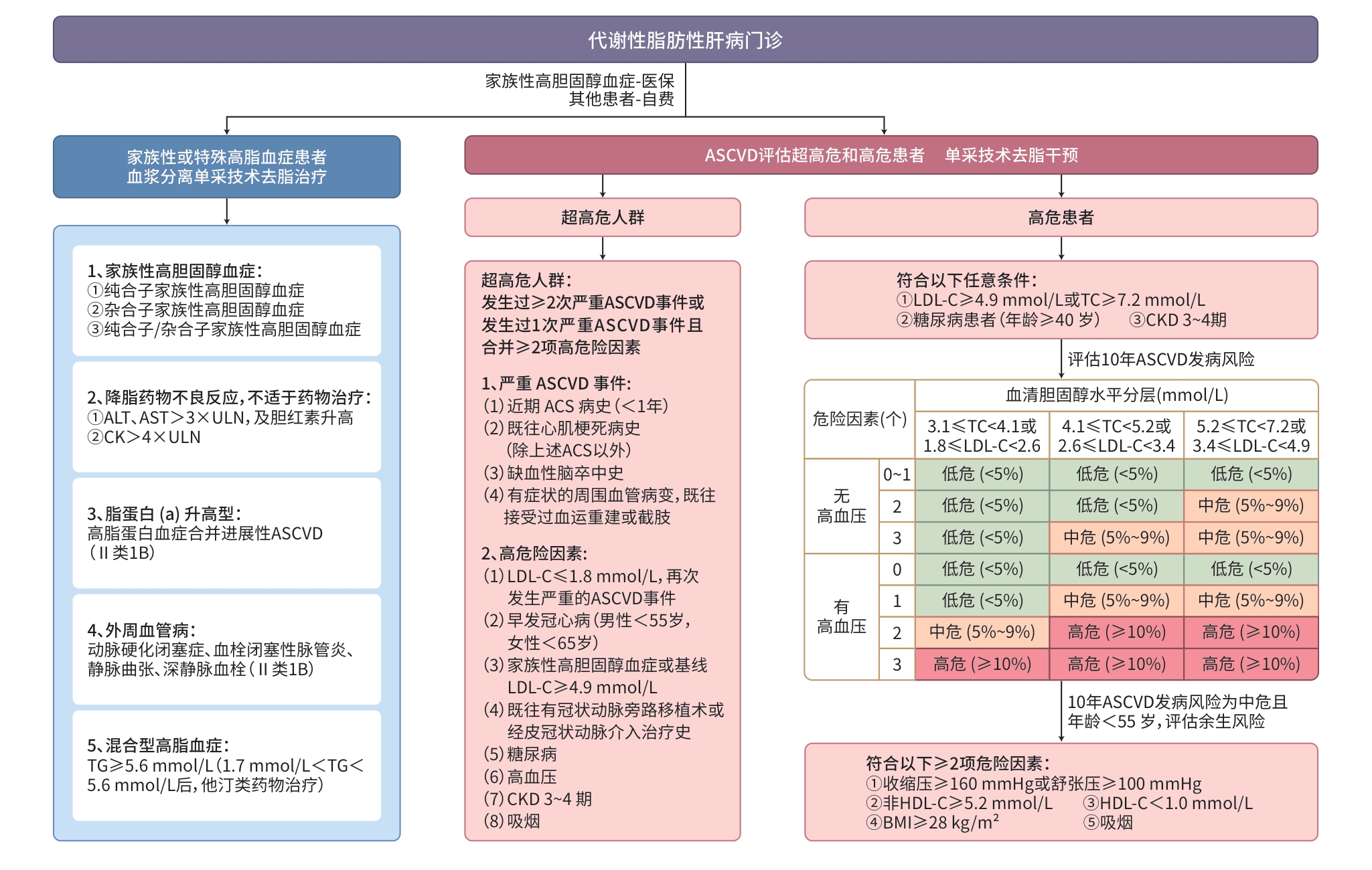
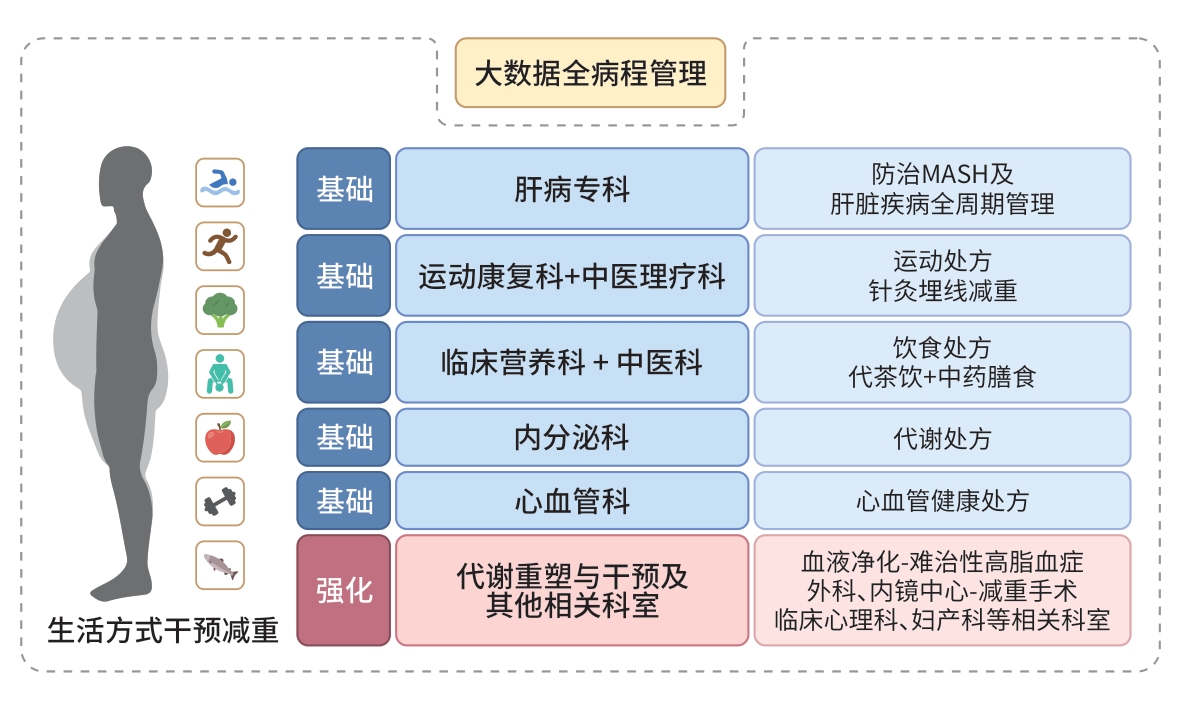
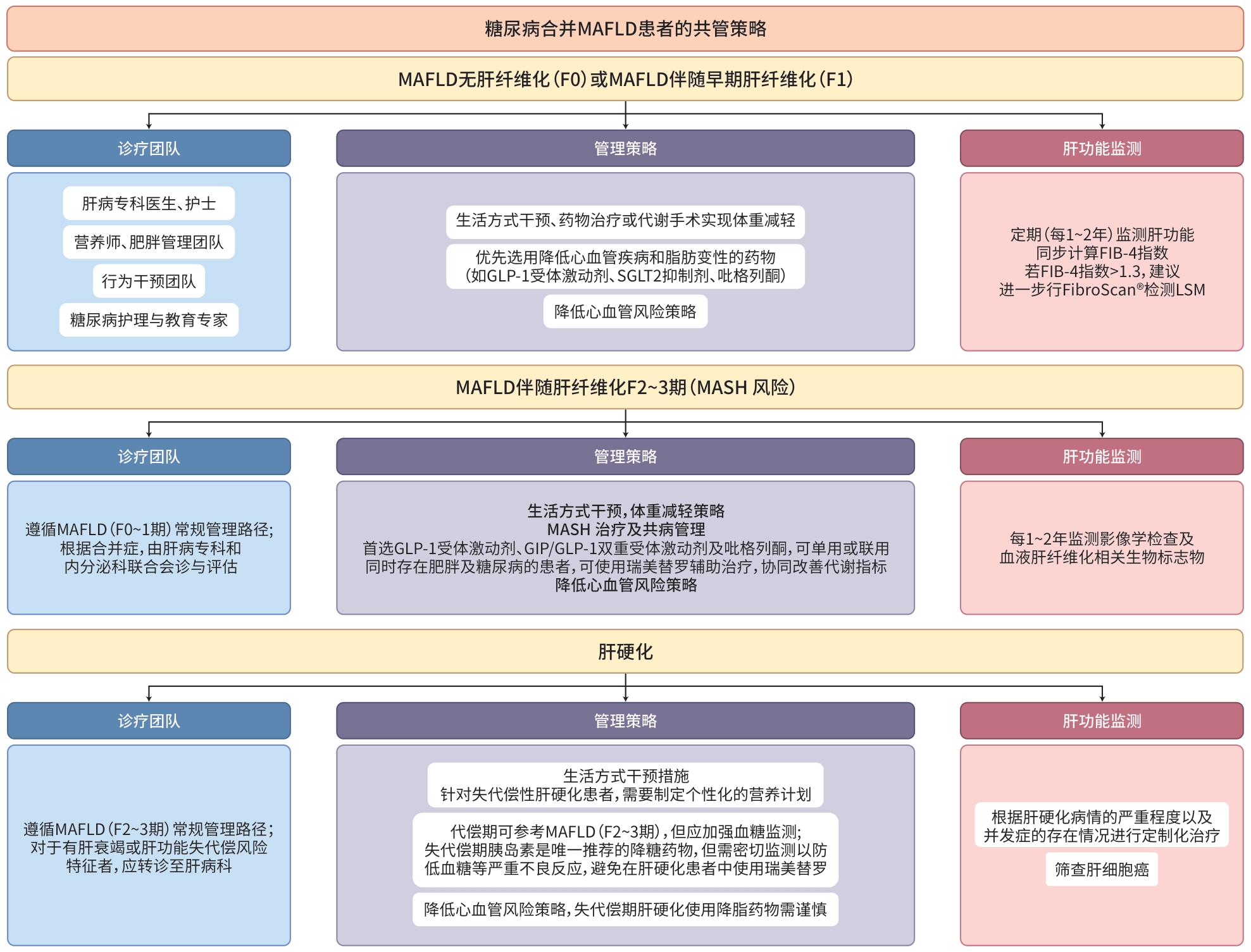
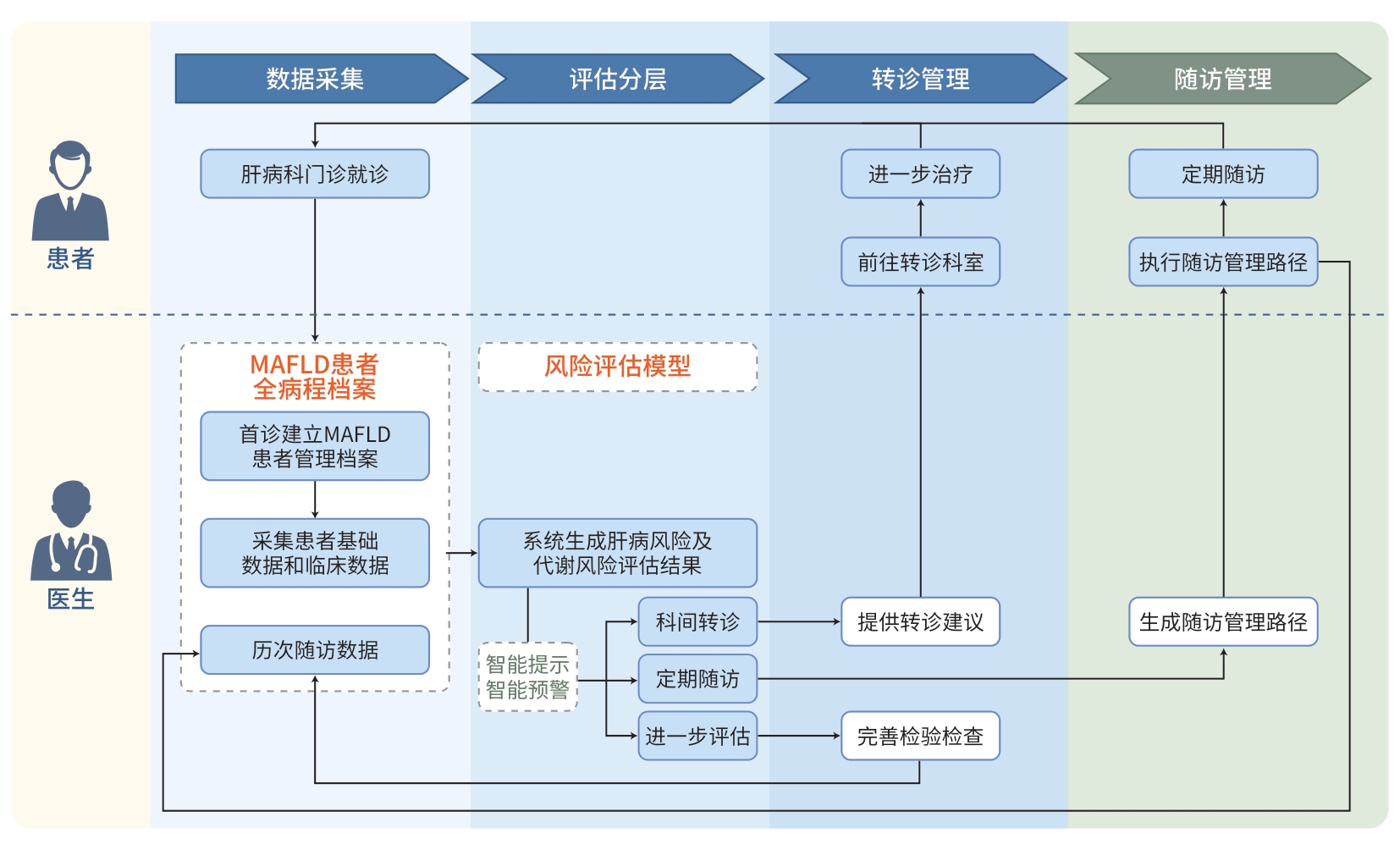
图 1 肝病专科联盟体系下MAFLD中西医结合分级诊疗与多学科协作全程管理路径
Figure 1. An integrated management pathway for MAFLD within a hepatology specialist alliance: Combining traditional Chinese and western medicine through multidisciplinary team
诊断步骤 内容 步骤一 影像学诊断脂肪肝和/或肝脏组织病理检查≥5%肝细胞大泡性脂肪变性 步骤二 (1)排除可能导致脂肪肝的其他原因及排除过量饮酒(每周乙醇摄入量男性≥210 g,女性≥140 g);若不能排除,患者
合并肥胖和/或2型糖尿病、代谢综合征则为MAFLD合并酒精性肝病(2)排除继发性脂肪性肝病(如存在基因3型丙型肝炎病毒感染、药物性脂肪肝、肝豆状核变性和营养不良等可导致
脂肪肝的疾病);若不能排除,患者合并肥胖和/或2型糖尿病、代谢综合征则为MAFLD合并继发性脂肪肝疾病步骤三 至少存在一项代谢心血管疾病危险因素: (1)BMI≥24.0 kg/m2,或者腰围≥90 cm(男性)和 85 cm(女性),或者体脂肪含量与体脂百分比超标 (2)动脉血压≥130/85 mmHg,或者在接受降血压药物治疗 (3)空腹血糖≥6.1 mmol/L,或者糖负荷后2 h血糖≥7.8 mmol/L或 HbA1c≥5.7%,或者2型糖尿病史,或者HOMA-IR≥2.5 (4)空腹血清甘油三酯≥1.70 mmol/L,或者正在接受降血脂药物治疗 (5)血清高密度脂蛋白胆固醇≤1.0 mmol/L(男性)和1.3 mmol/L(女性),或者正在接受降血脂药物治疗 注:MAFLD,代谢相关脂肪性肝病;BMI,体重指数;HbA1c,糖化血红蛋白;HOMA-IR,胰岛素抵抗指数。
表 2 肝脂肪变性的无创评估
Table 2. Non-invasive assessment of hepatic steatosis
诊断技术 技术名称 核心特点 局限性 超声 超声显像 最为常用,可诊断弥漫性和不均
质性脂肪肝敏感性低于CAP/UAP技术;仅能定性或
半定量评估,精度不足瞬时弹性成像相关技术 CAP(FibroScan®) 通过超声波衰减定量评估脂肪含
量。敏感性高于超声显像,可连
续监测脂肪变化肥胖患者腹壁厚(>25 mm)、中-大量腹水
等患者不适于该检查;
重度肥胖、非空腹状态、血清 ALT显著升
高,以及肝脏淤血、淤胆及重度肝脂肪变
性可影响检测结果UAP(FibroTouch®) 原理与CAP相近,数值参考范围
相近磁共振技术 磁共振质子密度脂肪分数 客观准确评估全肝脂肪含量,为
临床试验常用评估标准检测成本高,设备普及率低,检查耗时
较长注:CAP,受控衰减参数;UAP,超声衰减参数;ALT,丙氨酸氨基转移酶。
-
[1] YOUNOSSI ZM, ZELBER-SAGI S, LAZARUS JV, et al. Global consensus recommendations for metabolic dysfunction-associated steatotic liver disease and steatohepatitis[J]. Gastroenterology, 2025, 169( 5): 1017- 1032. DOI: 10.1053/j.gastro.2025.02.044. [2] ZHOU JH, ZHOU F, WANG WX, et al. Epidemiological features of NAFLD from 1999 to 2018 in China[J]. Hepatology, 2020, 71( 5): 1851- 1864. DOI: 10.1002/hep.31150. [3] PIPITONE RM, CICCIOLI C, INFANTINO G, et al. MAFLD: A multisystem disease[J]. Ther Adv Endocrinol Metab, 2023, 14: 20420188221145549. DOI: 10.1177/20420188221145549. [4] YOUNOSSI ZM, PAIK JM, HENRY L, et al. Pharmaco-economic assessment of screening strategies for high-risk MASLD in primary care[J]. Liver Int, 2025, 45( 4): e16119. DOI: 10.1111/liv.16119. [5] CUSI K, ISAACS S, BARB D, et al. American Association of Clinical Endocrinology clinical practice guideline for the diagnosis and management of nonalcoholic fatty liver disease in primary care and endocrinology clinical settings: Co-sponsored by the American Association for the Study of Liver Diseases(AASLD)[J]. Endocr Pract, 2022, 28( 5): 528- 562. DOI: 10.1016/j.eprac.2022.03.010. [6] Chronic Disease Management Branch of China Medical Biotechnology Association; Chinese Research Hospital Society(Integrative Chinese and Western Medicine); Chinese Society of General Practice, Chinese Medical Association, et al. Guideline for diagnosis and management of metabolic dysfunction-associated fatty liver disease in primary care(2025)[J]. Chin J Hepatol, 2025, 33( 5): 422- 433. DOI: 10.3760/cma.j.cn501113-20250305-00073.中国医药生物技术协会慢病管理分会, 中国研究型医院学会肝病(中西医结合)专业委员会, 中华医学会全科医学分会, 等. 代谢相关脂肪性肝病基层诊疗与管理指南(2025年)[J]. 中华肝脏病杂志, 2025, 33( 5): 422- 433. DOI: 10.3760/cma.j.cn501113-20250305-00073. [7] Chinese Society of Hepatology, Chinese Medical Association. Guidelines for the prevention and treatment of metabolic dysfunction-associated(non-alcoholic) fatty liver disease(Version 2024)[J]. J Prac Hepatol, 2024, 27( 4): 494- 510. DOI: 10.3760/cma.j.cn501113-20240327-00163.中华医学会肝病学分会. 代谢相关(非酒精性)脂肪性肝病防治指南(2024年版)[J]. 实用肝脏病杂志, 2024, 27( 4): 494- 510. DOI: 10.3760/cma.j.cn501113-20240327-00163. [8] ESLAM M, FAN JG, YU ML, et al. The Asian Pacific Association for the Study of the Liver clinical practice guidelines for the diagnosis and management of metabolic dysfunction-associated fatty liver disease[J]. Hepatol Int, 2025, 19( 2): 261- 301. DOI: 10.1007/s12072-024-10774-3. [9] BOURSIER J, HAGSTRÖM H, EKSTEDT M, et al. Non-invasive tests accurately stratify patients with NAFLD based on their risk of liver-related events[J]. J Hepatol, 2022, 76( 5): 1013- 1020. DOI: 10.1016/j.jhep.2021.12.031. [10] LE MH, LE DM, BAEZ TC, et al. Global incidence of adverse clinical events in non-alcoholic fatty liver disease: A systematic review and meta-analysis[J]. Clin Mol Hepatol, 2024, 30( 2): 235- 246. DOI: 10.3350/cmh.2023.0485. [11] O’BEIRNE J, SKOIEN R, LEGGETT BA, et al. Diabetes mellitus and the progression of non-alcoholic fatty liver disease to decompensated cirrhosis: A retrospective cohort study[J]. Med J Aust, 2023, 219( 8): 358- 365. DOI: 10.5694/mja2.52104. [12] LIU JY, AYADA I, ZHANG XF, et al. Estimating global prevalence of metabolic dysfunction-associated fatty liver disease in overweight or obese adults[J]. Clin Gastroenterol Hepatol, 2022, 20( 3): e573- e582. DOI: 10.1016/j.cgh.2021.02.030. [13] HUANG DQ, NOUREDDIN N, AJMERA V, et al. Type 2 diabetes, hepatic decompensation, and hepatocellular carcinoma in patients with non-alcoholic fatty liver disease: An individual participant-level data meta-analysis[J]. Lancet Gastroenterol Hepatol, 2023, 8( 9): 829- 836. DOI: 10.1016/S2468-1253(23)00157-7. [14] Chinese Diabetes Society, Chinese Medical Association. Guideline for the prevention and treatment of diabetes mellitus in China(2024 edition)[J]. Chin J Diabetes Mellitus, 2025, 17( 1): 16- 139. DOI: 10.3760/cma.j.cn115791-20241203-00705.中华医学会糖尿病学分会. 中国糖尿病防治指南(2024版)[J]. 中华糖尿病杂志, 2025, 17( 1): 16- 139. DOI: 10.3760/cma.j.cn115791-20241203-00705. [15] Joint Committee on the Revision of Chinese Guidelines for Lipid Management. Chinese guidelines for lipid management(2023)[J]. Chin J Cardiol, 2023, 51( 3): 221- 255. DOI: 10.3760/cma.j.cn112148-20230119-00038.中国血脂管理指南修订联合专家委员会. 中国血脂管理指南(2023年)[J]. 中华心血管病杂志, 2023, 51( 3): 221- 255. DOI: 10.3760/cma.j.cn112148-20230119-00038. [16] MANTOVANI A, CSERMELY A, TILG H, et al. Comparative effects of non-alcoholic fatty liver disease and metabolic dysfunction-associated fatty liver disease on risk of incident cardiovascular events: A meta-analysis of about 13 million individuals[J]. Gut, 2023, 72( 7): 1433- 1436. DOI: 10.1136/gutjnl-2022-328224. [17] Chinese Hypertension Prevention and Treatment Guidelines Revision Committee, Alliance Hypertension, Hypertension Division of China International Exchange and Promotive Association for Medical and Health Care, et al. Chinese guidelines for the prevention and treatment of hypertension(revised 2024 edition)[J]. Chin J Hypertens, 2024, 32( 7): 603- 700. DOI: 10.16439/j.issn.1673-7245.2024.07.002.中国高血压防治指南修订委员会, 高血压联盟(中国, 中国医疗保健国际交流促进会高血压分会, 等. 中国高血压防治指南(2024年修订版)[J]. 中华高血压杂志, 2024, 32( 7): 603- 700. DOI: 10.16439/j.issn.1673-7245.2024.07.002. [18] MANTOVANI A, PETRACCA G, BEATRICE G, et al. Non-alcoholic fatty liver disease and risk of incident chronic kidney disease: An updated meta-analysis[J]. Gut, 2022, 71( 1): 156- 162. DOI: 10.1136/gutjnl-2020-323082. [19] MAGHERMAN L, VAN PARYS R, PAUWELS NS, et al. Meta-analysis: The impact of light-to-moderate alcohol consumption on progressive non-alcoholic fatty liver disease[J]. Aliment Pharmacol Ther, 2023, 57( 8): 820- 836. DOI: 10.1111/apt.17388. [20] LIEBE R, ESPOSITO I, BOCK HH, et al. Diagnosis and management of secondary causes of steatohepatitis[J]. J Hepatol, 2021, 74( 6): 1455- 1471. DOI: 10.1016/j.jhep.2021.01.045. [21] The Editorial Committee of Chinese Journal of Cardiovascular Research; Heart-Renal-Metabolic Disease Prevention and Treatment Group, Future Biomedical Engineering Branch, China Future Research Association. Chinese expert consensus on comprehensive management of patients with cardiovascular-kidney-metabolic syndrome[J]. Chin J Cardiovasc Res, 2025, 23( 3): 193- 228. DOI: 10.3969/j.issn.1672-5301.2025.03.001.《中国心血管病研究》杂志编辑委员会, 中国未来研究会未来生物医学工程分会心肾代谢性疾病防治学组. 心血管-肾脏-代谢综合征患者的综合管理中国专家共识[J]. 中国心血管病研究, 2025, 23( 3): 193- 228. DOI: 10.3969/j.issn.1672-5301.2025.03.001. [22] The Specialist Committee for Primary Diabetes Care, China Association of Chinese Medicine; Diabetes Society, China Association of Chinese Medicine. Standard for co-management of diabetes under three disciplines[J]. Chin J Diabetes Mellitus, 2024, 16( 11): 1215- 1222. DOI: 10.13288/j.11-2166/r.2024.19.017.中华中医药学会基层糖尿病防治专家指导委员会, 中华中医药学会糖尿病分会. 糖尿病“三师共管”诊疗模式应用指南(2024版)[J]. 中华糖尿病杂志, 2024, 16( 11): 1215- 1222. DOI: 10.13288/j.11-2166/r.2024.19.017. [23] YAN DW, FENG K. Expert consensus on referral system and referral standard for graded diagnosis and treatment of diabetes mellitus in Shenzhen[J]. Shenzhen J Integr Tradit Chin West Med, 2022, 32( 11): 29- 34. DOI: 10.16458/j.cnki.1007-0893.2022.11.008.阎德文, 冯琨. 糖尿病分级诊疗转诊制度与转诊标准深圳专家共识[J]. 深圳中西医结合杂志, 2022, 32( 11): 29- 34. DOI: 10.16458/j.cnki.1007-0893.2022.11.008. [24] AJMERA V, CEPIN S, TESFAI K, et al. A prospective study on the prevalence of NAFLD, advanced fibrosis, cirrhosis and hepatocellular carcinoma in people with type 2 diabetes[J]. J Hepatol, 2023, 78( 3): 471- 478. DOI: 10.1016/j.jhep.2022.11.010. [25] European Association for the Study of the Liver(EASL); European Association for the Study of Diabetes(EASD); European Association for the Study of Obesity(EASO). EASL-EASD-EASO clinical practice guidelines on the management of metabolic dysfunction-associated steatotic liver disease(MASLD)[J]. J Hepatol, 2024, 81( 3): 492- 542. DOI: 10.1016/j.jhep.2024.04.031. [26] CUSI K, ABDELMALEK MF, APOVIAN CM, et al. Metabolic dysfunction-associated steatotic liver disease(MASLD) in people with diabetes: The need for screening and early intervention. A consensus report of the American Diabetes Association[J]. Diabetes Care, 2025, 48( 7): 1057- 1082. DOI: 10.2337/dci24-0094. [27] LEE HH, LEE HA, KIM EJ, et al. Metabolic dysfunction-associated steatotic liver disease and risk of cardiovascular disease[J]. Gut, 2024, 73( 3): 533- 540. DOI: 10.1136/gutjnl-2023-331003. [28] SOHN W, LEE YS, KIM SS, et al. KASL clinical practice guidelines for the management of metabolic dysfunction-associated steatotic liver disease 2025[J]. Clin Mol Hepatol, 2025, 31( Suppl): S1- S31. DOI: 10.3350/cmh.2025.0045. [29] VILAR-GOMEZ E, MARTINEZ-PEREZ Y, CALZADILLA-BERTOT L, et al. Weight loss through lifestyle modification significantly reduces features of nonalcoholic steatohepatitis[J]. Gastroenterology, 2015, 149( 2): 367- 378. DOI: 10.1053/j.gastro.2015.04.005. [30] XIAO JL, NG CH, CHAN KE, et al. Hepatic, extra-hepatic outcomes and causes of mortality in NAFLD-an umbrella overview of systematic review of meta-analysis[J]. J Clin Exp Hepatol, 2023, 13( 4): 656- 665. DOI: 10.1016/j.jceh.2022.11.006. [31] Chinese Society of Laboratory Medicine; Division of Lipids and Lipoprotein, Chinese Society of Biochemistry and Molecular Biology; Cardiovascular Health Professional Committee, China Primary Health Care Foundation, et al. Chinese expert consensus on early screening and management of homozygous familial hypercholesterolemia(2024)[J]. Chin J Lab Med, 2024, 47( 10): 1126- 1138. DOI: 10.3760/cma.j.cn114452-20240430-00218.中华医学会检验医学分会, 中国生物化学与分子生物学会脂质与脂蛋白分会, 中国初级卫生保健基金会心血管健康专业委员会, 等. 纯合子家族性高胆固醇血症早期筛查与管理中国专家共识(2024年)[J]. 中华检验医学杂志, 2024, 47( 10): 1126- 1138. DOI: 10.3760/cma.j.cn114452-20240430-00218. [32] National Society of Cardiometabolic Medicine. Chinese expert consensus on the diagnosis and management strategy of patients with statin intolerance[J]. Chin Circ J, 2024, 39( 2): 105- 115. DOI: 10.3969/j.issn.1000-3614.2024.02.001.国家心血管病专家委员会心血管代谢医学专业委员会. 他汀不耐受的临床诊断与处理中国专家共识[J]. 中国循环杂志, 2024, 39( 2): 105- 115. DOI: 10.3969/j.issn.1000-3614.2024.02.001. [33] Expert Consensus Development Group on Comprehensive Management of Lipid-Related Cardiovascular Risk; Dongfang Huaxia Cardiovascular Health Institute, Suzhou Industrial Park. Chinese expert consensus on comprehensive management of lipid-related cardiovascular risk(2025)[J]. Chin J Cardiol Online Ed, 2025, 8( 1): 1- 23. DOI: 10.3760/cma.j.cn116031.2025.1000192.全面管理血脂相关心血管风险专家共识(2025)制订专家组, 苏州工业园区东方华夏心血管健康研究院. 全面管理血脂相关心血管风险专家共识(2025)[J]. 中华心血管病杂志(网络版), 2025, 8( 1): 1- 23. DOI: 10.3760/cma.j.cn116031.2025.1000192. [34] WAN XY, CHEN YZ, CHEN XM. Interpretation of the 2019 clinical practice guidelines on plasma exchange and immunoadsorption from the American Society for Apheresis(8th edition)[J/CD]. Chin J Kidney Dis Investig Electron Ed, 2021, 10( 1): 8- 13. DOI: 10.3877/cma.j.issn.2095-3216.2021.01.002.万兴运, 陈意志, 陈香美. 2019年美国血浆置换学会血浆置换和免疫吸附临床实践指南(第8版)解读[J/CD]. 中华肾病研究电子杂志, 2021, 10( 1): 8- 13. DOI: 10.3877/cma.j.issn.2095-3216.2021.01.002. [35] Writing Group for Chinese Expert Consensus on the Diagnosis and Treatment of Mixed Hyperlipidemia in Primary Care. Chinese expert consensus on the diagnosis and treatment of mixed hyperlipidemia in primary care(2024)[J]. Chin J Gen Pract, 2024, 23( 9): 907- 917. DOI: 10.3760/cma.j.cn114798-20240523-00476.《混合型高脂血症基层诊疗中国专家共识(2024年)》编写专家组. 混合型高脂血症基层诊疗中国专家共识(2024年)[J]. 中华全科医师杂志, 2024, 23( 9): 907- 917. DOI: 10.3760/cma.j.cn114798-20240523-00476. [36] SHEA S, LIONIS C, KITE C, et al. Non-alcoholic fatty liver disease and coexisting depression, anxiety and/or stress in adults: A systematic review and meta-analysis[J]. Front Endocrinol, 2024, 15: 1357664. DOI: 10.3389/fendo.2024.1357664. [37] CAI XB, LU LG. A multidisciplinary management pathway for patients with metabolic associated fatty liver disease[J]. Chin J Hepatol, 2025, 33( 9): 822- 825. DOI: 10.3760/cma.j.cn501113-20250604-00217.蔡晓波, 陆伦根. 代谢相关脂肪性肝病患者多学科管理路径[J]. 中华肝脏病杂志, 2025, 33( 9): 822- 825. DOI: 10.3760/cma.j.cn501113-20250604-00217. [38] LASSAILLY G, CAIAZZO R, NTANDJA-WANDJI LC, et al. Bariatric surgery provides long-term resolution of nonalcoholic steatohepatitis and regression of fibrosis[J]. Gastroenterology, 2020, 159( 4): 1290- 1301. DOI: 10.1053/j.gastro.2020.06.006. [39] YOUNOSSI Z, STEPANOVA M, ONG JP, et al. Nonalcoholic steatohepatitis is the fastest growing cause of hepatocellular carcinoma in liver transplant candidates[J]. Clin Gastroenterol Hepatol, 2019, 17( 4): 748- 755. DOI: 10.1016/j.cgh.2018.05.057. [40] HALDAR D, KERN B, HODSON J, et al. Outcomes of liver transplantation for non-alcoholic steatohepatitis: A European Liver Transplant Registry study[J]. J Hepatol, 2019, 71( 2): 313- 322. DOI: 10.1016/j.jhep.2019.04.011. [41] Branch of Hepatobiliary Diseases, China Association of Chinese Medicine. Guidelines for preventive treatment intervention of non-alcoholic simple fatty liver disease[J]. Chin J Integr Tradit West Med Liver Dis, 2024, 34( 1): Post insertion 1-Post insertion 6.中华中医药学会肝胆病分会. 非酒精性单纯性脂肪性肝病治未病干预指南[J]. 中西医结合肝病杂志, 2024, 34( 1): 后插1-后插6. [42] Digestive System Diseases Professional Committee of Chinese Association of Integrative Medicine. Expert consensus on integrated traditional Chinese and western medicine diagnosis and treatment of non-alcoholic fatty liver disease(2025)[J]. Chin J Integr Tradit West Med Dig, 2025, 33( 4): 339- 350. DOI: 10.3969/j.issn.1671-038X.2025.04.01.中国中西医结合学会消化系统疾病专业委员会. 非酒精性脂肪性肝病中西医结合诊疗专家共识(2025年)[J]. 中国中西医结合消化杂志, 2025, 33( 4): 339- 350. DOI: 10.3969/j.issn.1671-038X.2025.04.01. [43] Branch of Hepatobiliary Diseases, Chinese Association of Chinese Medicine. Chinese medicine practice guide for acupoint catgut embedding in treating non-alcoholic fatty liver disease[J]. J Clin Hepatol, 2022, 38( 9): 1990- 1993. DOI: 10.3969/j.issn.1001-5256.2022.09.008.中华中医药学会肝胆病分会. 穴位埋线治疗非酒精性脂肪性肝病中医实践指南[J]. 临床肝胆病杂志, 2022, 38( 9): 1990- 1993. DOI: 10.3969/j.issn.1001-5256.2022.09.008. [44] BEYGI M, AHI S, ZOLGHADRI S, et al. Management of metabolic-associated fatty liver disease/metabolic dysfunction-associated steatotic liver disease: From medication therapy to nutritional interventions[J]. Nutrients, 2024, 16( 14): 2220. DOI: 10.3390/nu16142220. [45] HASSANI ZADEH S, MANSOORI A, HOSSEINZADEH M. Relationship between dietary patterns and non-alcoholic fatty liver disease: A systematic review and meta-analysis[J]. J Gastroenterol Hepatol, 2021, 36( 6): 1470- 1478. DOI: 10.1111/jgh.15363. [46] OH S, TSUJIMOTO T, KIM B, et al. Weight-loss-independent benefits of exercise on liver steatosis and stiffness in Japanese men with NAFLD[J]. JHEP Rep, 2021, 3( 3): 100253. DOI: 10.1016/j.jhepr.2021.100253. [47] KIM D, KONYN P, CHOLANKERIL G, et al. Physical activity is associated with nonalcoholic fatty liver disease and significant fibrosis measured by FibroScan[J]. Clin Gastroenterol Hepatol, 2022, 20( 6): e1438- e1455. DOI: 10.1016/j.cgh.2021.06.029. [48] LOUVET A, BOURCIER V, ARCHAMBEAUD I, et al. Low alcohol consumption influences outcomes in individuals with alcohol-related compensated cirrhosis in a French multicenter cohort[J]. J Hepatol, 2023, 78( 3): 501- 512. DOI: 10.1016/j.jhep.2022.11.013. [49] MA J, ZHANG J, XIA L, et al. Observation of the Clinical Effect of Auricular Acupressure in the Treatment of Insomnia: A Single Center, Single-Arm, Prospective Study[J]. Holist Nurs Pract, 2025. DOI: 10.1097/HNP.0000000000000736.[ Epub ahead of print] [50] SIU PM, YU AP, CHIN EC, et al. Effects of Tai Chi or conventional exercise on central obesity in middle-aged and older adults: A three-group randomized controlled trial[J]. Ann Intern Med, 2021, 174( 8): 1050- 1057. DOI: 10.7326/M20-7014. [51] WANG F, WANG WD, ZHANG RR, et al. Clinical observation on physiological and psychological effects of Eight-Section Brocade on type 2 diabetic patients[J]. J Tradit Chin Med, 2008, 28( 2): 101- 105. DOI: 10.1016/s0254-6272(08)60025-4. [52] YAN MX, ZHU M, QUAN F, et al. Acupoint thread-embedding at fat layer for abdominal obesity: A randomized controlled trial[J]. Chin Acupunct Moxibustion, 2024, 44( 12): 1370- 1376. DOI: 10.13703/j.0255-2930.20240517-k0005.晏明熙, 朱敏, 全菲, 等. 脂肪层穴位埋线治疗腹型肥胖: 随机对照试验[J]. 中国针灸, 2024, 44( 12): 1370- 1376. DOI: 10.13703/j.0255-2930.20240517-k0005. [53] WANG Y, YUE HY, CHEN YQ, et al. Jianpi Peiyuan acupoint thread embedding therapy for perimenopausal obesity: A randomized controlled trial[J]. Chin Acupunct Moxibustion, 2023, 43( 3): 294- 298. DOI: 10.13703/j.0255-2930.20220526-0007.王颖, 岳虹妤, 陈颖棋, 等.“健脾培元”穴位埋线法治疗围绝经期肥胖: 随机对照试验[J]. 中国针灸, 2023, 43( 3): 294- 298. DOI: 10.13703/j.0255-2930.20220526-0007. [54] NEWSOME PN, AMBERY P. Incretins(GLP-1 receptor agonists and dual/triple agonists) and the liver[J]. J Hepatol, 2023, 79( 6): 1557- 1565. DOI: 10.1016/j.jhep.2023.07.033. [55] KUCHAY MS, KRISHAN S, MISHRA SK, et al. Effect of empagliflozin on liver fat in patients with type 2 diabetes and nonalcoholic fatty liver disease: A randomized controlled trial(E-LIFT trial)[J]. Diabetes Care, 2018, 41( 8): 1801- 1808. DOI: 10.2337/dc18-0165. [56] VILAR-GOMEZ E, VUPPALANCHI R, DESAI AP, et al. Long-term metformin use may improve clinical outcomes in diabetic patients with non-alcoholic steatohepatitis and bridging fibrosis or compensated cirrhosis[J]. Aliment Pharmacol Ther, 2019, 50( 3): 317- 328. DOI: 10.1111/apt.15331. [57] HARRISON SA, BEDOSSA P, GUY CD, et al. A phase 3, randomized, controlled trial of resmetirom in NASH with liver fibrosis[J]. N Engl J Med, 2024, 390( 6): 497- 509. DOI: 10.1056/NEJMoa2309000. [58] AYADA I, VAN KLEEF LA, ZHANG H, et al. Dissecting the multifaceted impact of statin use on fatty liver disease: A multidimensional study[J]. EBioMedicine, 2023, 87: 104392. DOI: 10.1016/j.ebiom.2022.104392. [59] ZHANG XR, WONG GL, YIP TC, et al. Angiotensin-converting enzyme inhibitors prevent liver-related events in nonalcoholic fatty liver disease[J]. Hepatology, 2022, 76( 2): 469- 482. DOI: 10.1002/hep.32294. [60] HU XY, LUO Y, ZU F, et al. Effects of electroacupuncture at“Fenglong”(ST40) and“Zusanli”(ST36) on the SIRT1/FOXO1 signaling pathway in non-alcoholic fatty liver disease model rats[J]. Acupunct Res, 2025, 50( 2): 150- 158. DOI: 10.13702/j.1000-0607.20240849.胡馨月, 罗亚, 祖芳, 等. 电针“丰隆”“足三里”对非酒精性脂肪肝大鼠SIRT1/FOXO1信号通路的影响[J]. 针刺研究, 2025, 50( 2): 150- 158. DOI: 10.13702/j.1000-0607.20240849. [61] ZHANG Q, YANG YH, LUO HP. Clinical study on the efficacy of acupuncture and moxibustion combined with exercise rehabilitation training on non-alcoholic fatty liver disease[J]. Chin J Cancer Prev Treat, 2016, 23( S2): 178- 179. DOI: 10.16073/j.cnki.cjcpt.2016.s2.085.张清, 杨永和, 罗和平. 针灸结合运动康复训练对非酒精性脂肪肝疗效的临床研究[J]. 中华肿瘤防治杂志, 2016, 23( S2): 178- 179. DOI: 10.16073/j.cnki.cjcpt.2016.s2.085. [62] WEI YT, CAO ZX, LI XJ, et al. Research progress in the molecular biological mechanisms for implanting catgut in acupoint therapy[J]. China J Tradit Chin Med Pharm, 2019, 34( 8): 3633- 3636.魏玉婷, 曹朝霞, 李小娟, 等. 穴位埋线疗法的分子生物学机制研究进展[J]. 中华中医药杂志, 2019, 34( 8): 3633- 3636. [63] SHEN MD, CHEN SB, DING XD. The effectiveness of digital twins in promoting precision health across the entire population: A systematic review[J]. NPJ Digit Med, 2024, 7( 1): 145. DOI: 10.1038/s41746-024-01146-0. [64] JOSHI S, SHAMANNA P, DHARMALINGAM M, et al. Digital twin-enabled personalized nutrition improves metabolic dysfunction-associated fatty liver disease in type 2 diabetes: Results of a 1-year randomized controlled study[J]. Endocr Pract, 2023, 29( 12): 960- 970. DOI: 10.1016/j.eprac.2023.08.016. [65] SUN C, FAN JG. Application of digital therapeutics in the treatment of nonalcoholic fatty liver disease[J]. J Clin Hepatol, 2022, 38( 4): 898- 901. DOI: 10.3969/j.issn.1001-5256.2022.04.032.孙超, 范建高. 数字疗法在非酒精性脂肪性肝病治疗中的应用[J]. 临床肝胆病杂志, 2022, 38( 4): 898- 901. DOI: 10.3969/j.issn.1001-5256.2022.04.032. [66] BJÖRNSDOTTIR S, ULFSDOTTIR H, GUDMUNDSSON EF, et al. User engagement, acceptability, and clinical markers in a digital health program for nonalcoholic fatty liver disease: Prospective, single-arm feasibility study[J]. JMIR Cardio, 2024, 8: e52576. DOI: 10.2196/52576. -



 PDF下载 ( 1729 KB)
PDF下载 ( 1729 KB)

 下载:
下载: