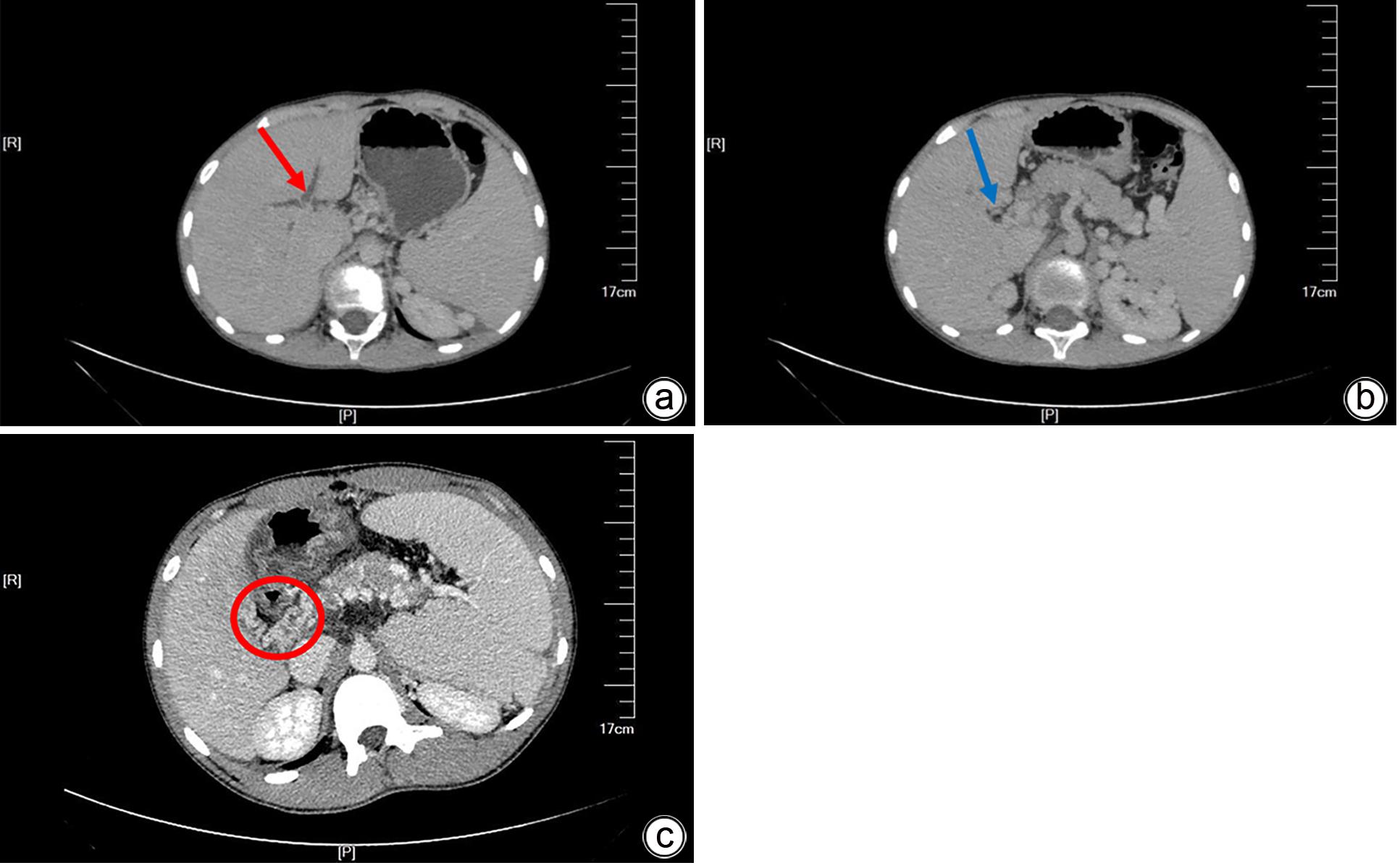
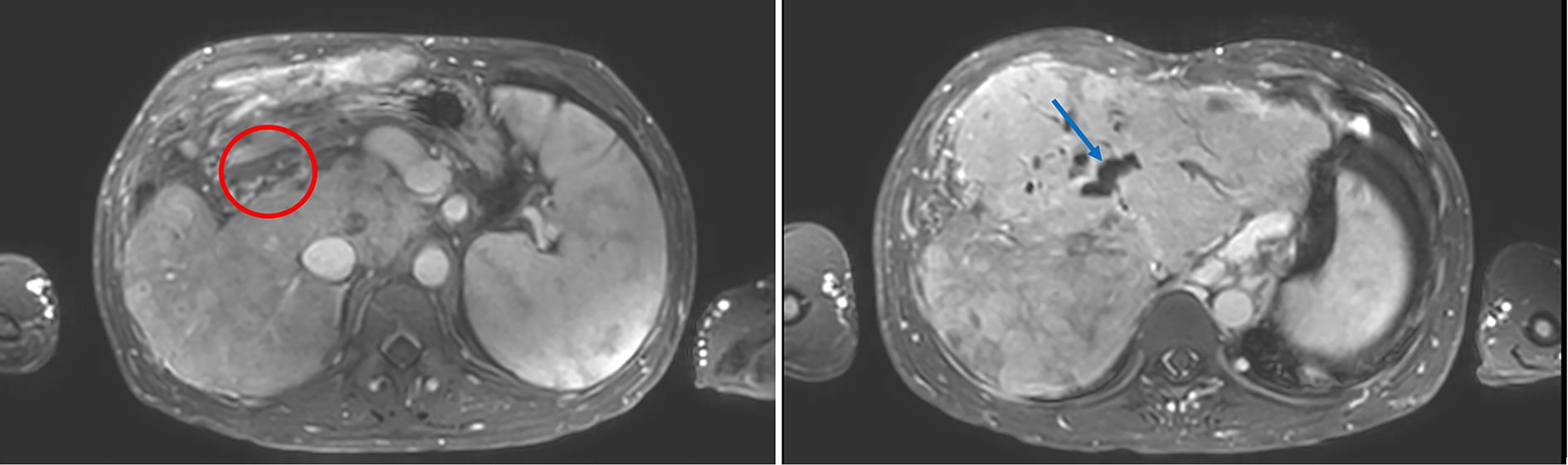
门静脉性胆道病的临床特征分析
DOI: 10.3969/j.issn.1001-5256.2023.11.020
伦理学声明:本研究方案于2017年12月28日经由吉林大学第一医院伦理委员会审批,批号:2017-322。
利益冲突声明:本文不存在任何利益冲突。
作者贡献声明:耿雯倩负责课题设计,资料分析,撰写论文;王崇、李航参与收集和分析数据;牛俊奇、许芳负责拟定写作思路,修改论文,指导撰写文章并最后定稿。
-
摘要:
目的 通过分析门静脉性胆道病(PB)患者的临床特征,旨在提高对PB的认识。 方法 收集吉林大学第一医院近年来诊断为PB的22例患者的临床资料,并对患者的临床表现、肝功能、腹部彩色多普勒超声、腹部CT和肝胆核磁共振成像进行分析,描述胆道异常的影像学表现,侧支循环类型和血栓形成部位等特点。 结果 本研究22例患者中,就诊的首发症状分别为:11例消化道出血,5例腹胀,3例腹痛,1例发热,1例腹部不适,1例牙龈出血。AST升高3例,ALT升高4例,GGT升高4例,ALP升高7例,CHE降低8例,Alb降低9例,Glo升高2例,TBil升高5例。20例患者有门静脉海绵样变性;2例存在门静脉系统血栓而无门静脉海绵样变性。22例患者均有胆管异常,其中2例仅为肝外胆管异常,12例仅为肝内胆管扩张,8例肝内外胆管均扩张。20例患者出现了不同部位的静脉曲张,其中19例主要表现为食管胃底静脉曲张,1例为胆囊周围静脉曲张,未见单纯肠系膜上静脉或脾静脉曲张。 结论 PB无典型的临床症状及肝功能指标变化,但影像学均可见不同部位胆管扩张、狭窄或畸形,需扩大样本量对其诊断及治疗方式进行进一步探索。 -
关键词:
- 胆道疾病 /
- 超声检查, 多普勒, 彩色 /
- 磁共振成像 /
- 治疗学
Abstract:Objective This article aims to investigate the clinical features of portal biliopathy (PB) patients, in order to improve the understanding of PB. Methods Clinical data were collected from 22 patients who were diagnosed with PB in recent years in The First Hospital of Jilin University, and an analysis was performed for their clinical manifestations, liver function, abdominal color Doppler ultrasound, abdominal CT, and hepatobiliary magnetic resonance imaging. The imaging manifestations of biliary tract abnormalities were described, as well as the type of collateral circulation and the location of thrombosis. Results As for the initial symptom in these 22 patients, three were 11 patients with gastrointestinal bleeding, 5 with abdominal distension, 3 with abdominal pain, 1 with fever, 1 with abdominal discomfort, and 1 with gingival bleeding. There were 3 patients with an increase in aspartate aminotransferase, 4 with an increase in alanine aminotransferase, 4 with an increase in gamma-glutamyl transpeptidase, 7 with an increase in alkaline phosphatase, 8 with a reduction in cholinesterase, 9 with a reduction in albumin, 2 with an increase in globulin, and 5 with an increase in total bilirubin. Among the 22 patients, 20 had cavernous transformation of the portal vein, and 2 had portal vein thrombosis without cavernous transformation. All 22 patients had bile duct abnormalities, among whom 2 had extrahepatic bile duct abnormalities alone, 12 had intrahepatic bile duct dilatation alone, and 8 had dilatation of both intrahepatic and extrahepatic bile ducts. Varices at different sites were observed in 20 patients, among whom 19 had esophageal and gastric varices and 1 had peri-gallbladder varices, and no varices was observed in the superior mesenteric vein or the splenic vein. Conclusion There are no typical clinical symptoms and changes in liver function parameters in patients with PB, but radiological examination may show dilatation, stenosis, or malformation of the bile ducts at different parts. Therefore, it is necessary to expand the sample size to further explore the diagnosis and treatment of PB. -
-
[1] DHIMAN RK, BEHERA A, CHAWLA YK, et al. Portal hypertensive biliopathy[J]. Gut, 2007, 56( 7): 1001- 1008. DOI: 10.1136/gut.2006.103606. [2] XU F, WEN XY, ZHANG L, et al. Portal ductopathy[J]. Chin J Hepatol, 2014, 22( 11): 871- 873. DOI: 10.3760/cma.j.issn.1007-3418.2014.011.016.许芳, 温晓玉, 张磊, 等. 门静脉性胆道病[J]. 中华肝脏病杂志, 2014, 22( 11): 871- 873. DOI: 10.3760/cma.j.issn.1007-3418.2014.011.016. [3] CHANDRA R, KAPOOR D, THARAKAN A, et al. Portal biliopathy[J]. J Gastroenterol Hepatol, 2001, 16( 10): 1086- 1092. DOI: 10.1046/j.1440-1746.2001.02562.x. [4] HE ZP, FAN LJ. Diagnosis and treatment of portal biliopathy[J]. Hepatobiliary Pancreat Dis Int, 2002, 1( 4): 581- 586. [5] JIANG P, WANG SP, LIU YH. A case of portal biliopathy[J]. J Clin Hepatol, 2022, 38( 2): 430- 432. DOI: 10.3969/j.issn.1001-5256.2022.02.034.姜朋, 王树鹏, 刘亚辉. 门静脉性胆道病1例报告[J]. 临床肝胆病杂志, 2022, 38( 2): 430- 432. DOI: 10.3969/j.issn.1001-5256.2022.02.034. [6] SHIN SM, KIM S, LEE JW, et al. Biliary abnormalities associated with portal biliopathy: Evaluation on MR cholangiography[J]. AJR Am J Roentgenol, 2007, 188( 4): W341- W347. DOI: 10.2214/AJR.05.1649. [7] PANG SJ, YE QW, SHI Y, et al. Progress in clinical diagnosis and treatment of portal hypertensive biliary disease[J]. J Hepatopancreatobiliary Surg, 2015, 27( 5): 431- 433. DOI: 10.11952/j.issn.1007-1954.2015.05.027.庞书杰, 叶庆旺, 施洋, 等. 门脉高压性胆病临床诊疗进展[J]. 肝胆胰外科杂志, 2015, 27( 5): 431- 433. DOI: 10.11952/j.issn.1007-1954.2015.05.027. [8] CHATTOPADHYAY S, NUNDY S. Portal biliopathy[J]. World J Gastroenterol, 2012, 18( 43): 6177- 6182. DOI: 10.3748/wjg.v18.i43.6177. [9] ITARE VB, IMANIRAD D, ALMAGHRABY A. Portal cholangiopathy: An uncommon cause of right upper quadrant pain[J]. Cureus, 2020, 12( 9): e10281. DOI: 10.7759/cureus.10281. [10] DHIMAN R, CHAWLA Y, DUSEJA A, et al. Portal hypertensive biliopathy(PHB) in patients with extrahepatic portal venous obstruction(EHPVO)[J]. J Gastroenterol Hepatol, 2006, 21: A222. [11] TACCHELLA G, GJERMENI O, CRINÓ SF, et al. Portal hypertensive biliopathy and bile duct varices presenting as jaundice[J]. Endoscopy, 2021, 53( 12): E442- E443. DOI: 10.1055/a-1337-1994. [12] NUNOI H, HIROOKA M, OCHI H, et al. Portal biliopathy diagnosed using color Doppler and contrast-enhanced ultrasound[J]. Intern Med, 2013, 52( 10): 1055- 1059. DOI: 10.2169/internalmedicine.52.8848. [13] KHUROO MS, RATHER AA, KHUROO NS, et al. Portal biliopathy[J]. World J Gastroenterol, 2016, 22( 35): 7973- 7982. DOI: 10.3748/wjg.v22.i35.7973. [14] DING HG, OUYANG Y. Clinical manifestations of portal hypertension[J]. Beijing Med J, 2011, 33( 12): 1014- 1017. DOI: 10.15932/j.0253-9713.2011.12.021.丁惠国, 欧阳颖. 门脉高压症临床表现[J]. 北京医学, 2011, 33( 12): 1014- 1017. DOI: 10.15932/j.0253-9713.2011.12.021. [15] OZKAVUKCU E, ERDEN A, ERDEN I. Imaging features of portal biliopathy: Frequency of involvement patterns with emphasis on MRCP[J]. Eur J Radiol, 2009, 71( 1): 129- 134. DOI: 10.1016/j.ejrad.2008.03.007. [16] BESA C, CRUZ JP, HUETE A, et al. Portal biliopathy: A multitechnique imaging approach[J]. Abdom Imaging, 2012, 37( 1): 83- 90. DOI: 10.1007/s00261-011-9765-2. [17] WALSER EM, RUNYAN BR, HECKMAN MG, et al. Extrahepatic portal biliopathy: Proposed etiology on the basis of anatomic and clinical features[J]. Radiology, 2011, 258( 1): 146- 153. DOI: 10.1148/radiol.10090923. [18] KHAN MR, TARIQ J, RAZA R, et al. Portal hypertensive biliopathy: Review of pathophysiology and management[J]. Trop Gastroenterol, 2012, 33( 3): 173- 178. DOI: 10.7869/tg.2012.44. [19] D’SOUZA SL, DAVENPORT MS, ELTA GH. Biliary stricture secondary to portal biliopathy[J]. Gastrointest Endosc, 2013, 78( 6): 942- 944. DOI: 10.1016/j.gie.2013.07.052. [20] SEZGIN O, OĞUZ D, ALTINTAŞ E, et al. Endoscopic management of biliary obstruction caused by cavernous transformation of the portal vein[J]. Gastrointest Endosc, 2003, 58( 4): 602- 608. DOI: 10.1067/s0016-5107(03)01975-8. [21] CHATTOPADHYAY S, GOVINDASAMY M, SINGLA P, et al. Portal biliopathy in patients with non-cirrhotic portal hypertension: Does the type of surgery affect outcome?[J]. HPB, 2012, 14( 7): 441- 447. DOI: 10.1111/j.1477-2574.2012.00473.x. -



 PDF下载 ( 781 KB)
PDF下载 ( 781 KB)

 下载:
下载: