柴胡疏肝散加减方对胆囊胆固醇结石肝郁证小鼠模型的治疗作用及其机制
DOI: 10.12449/JCH260219
Therapeutic effect and mechanism of modified Chaihu Shugan Powder on a mouse model of gallbladder cholesterol stone with liver depression syndrome
-
摘要:
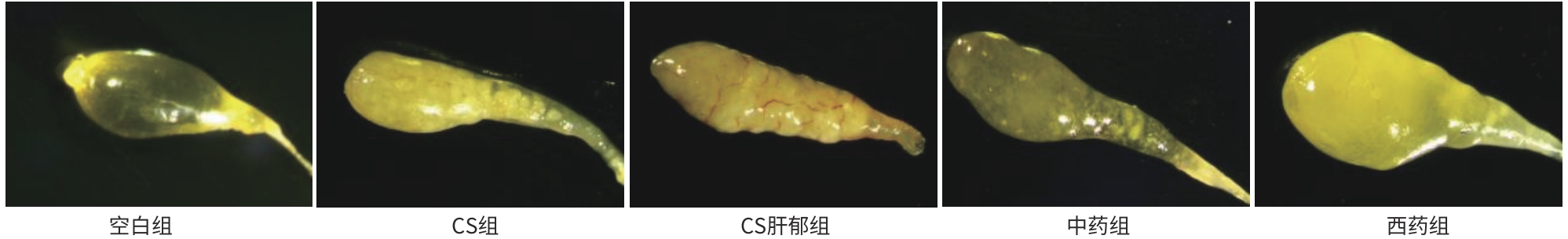
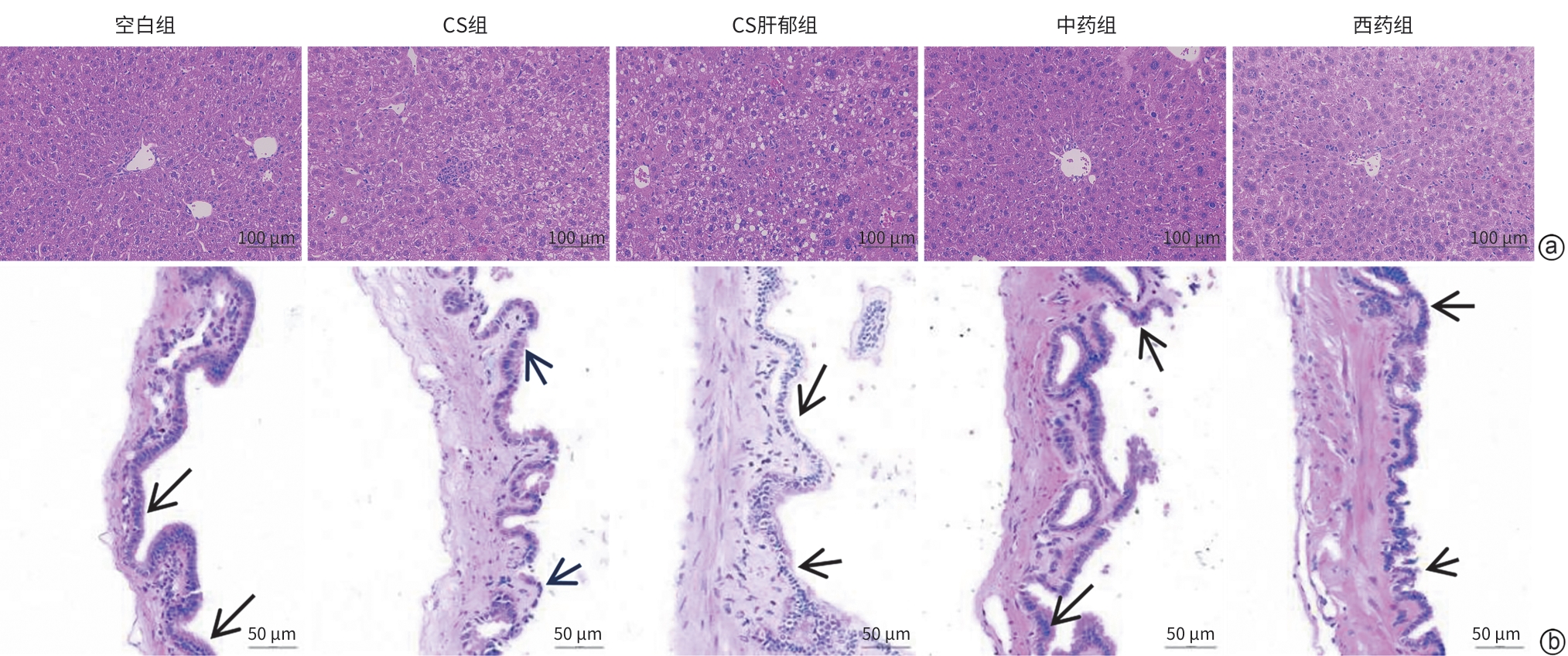
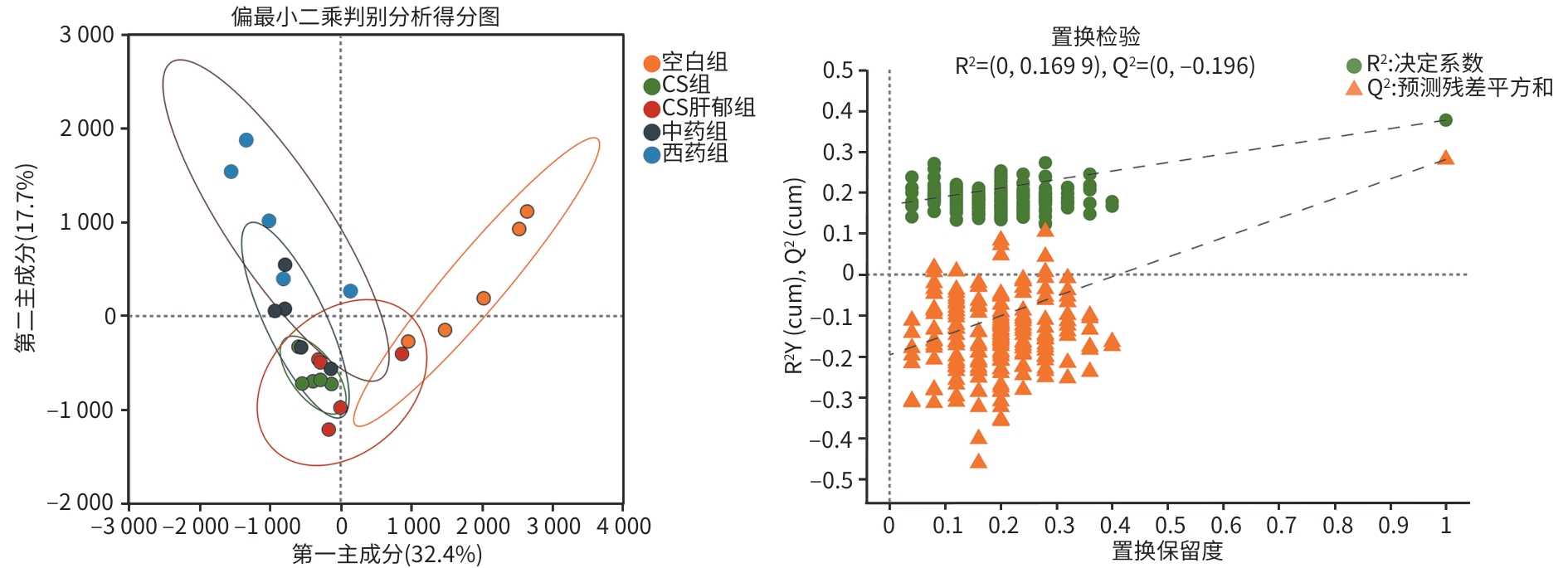
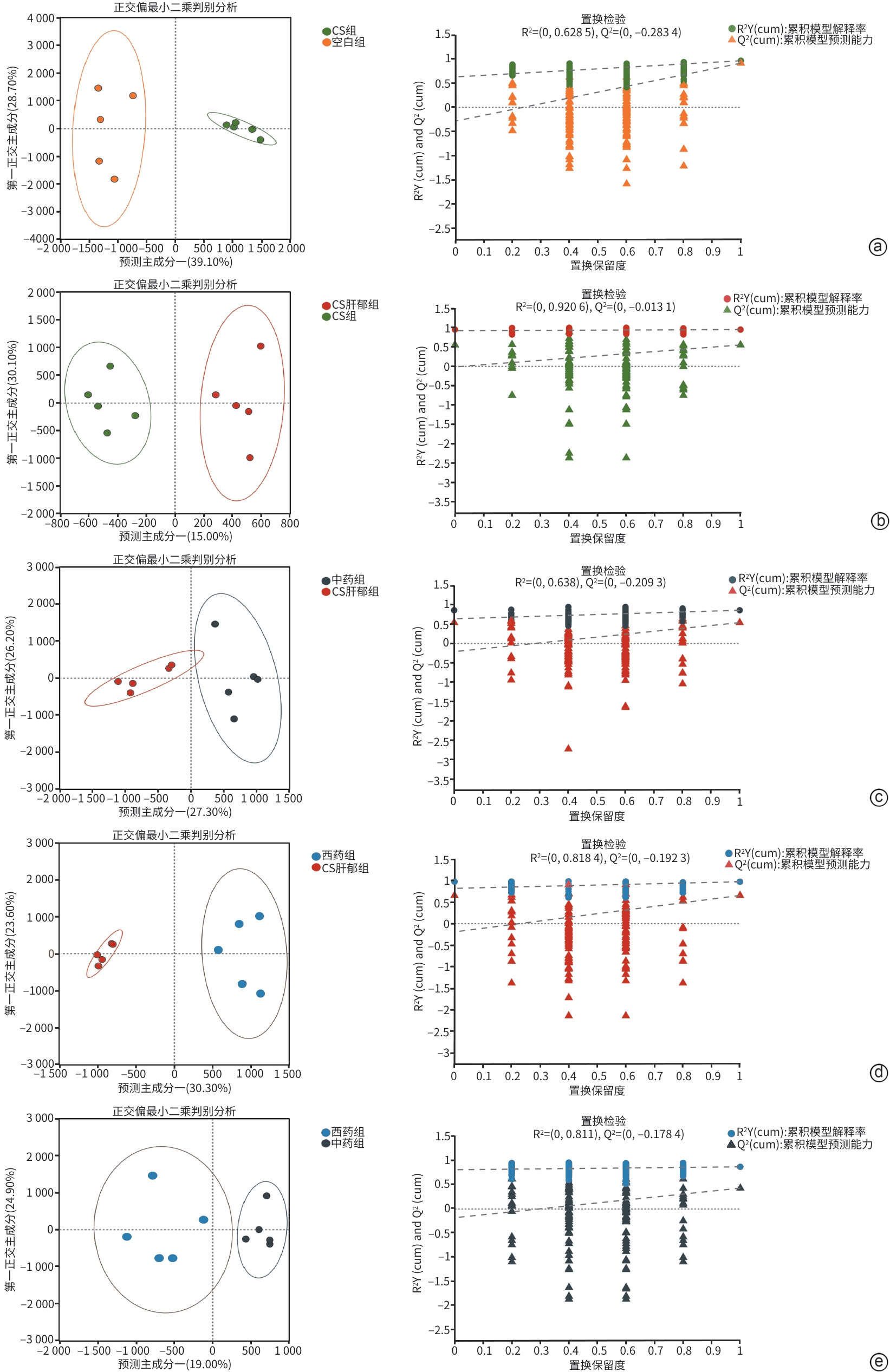
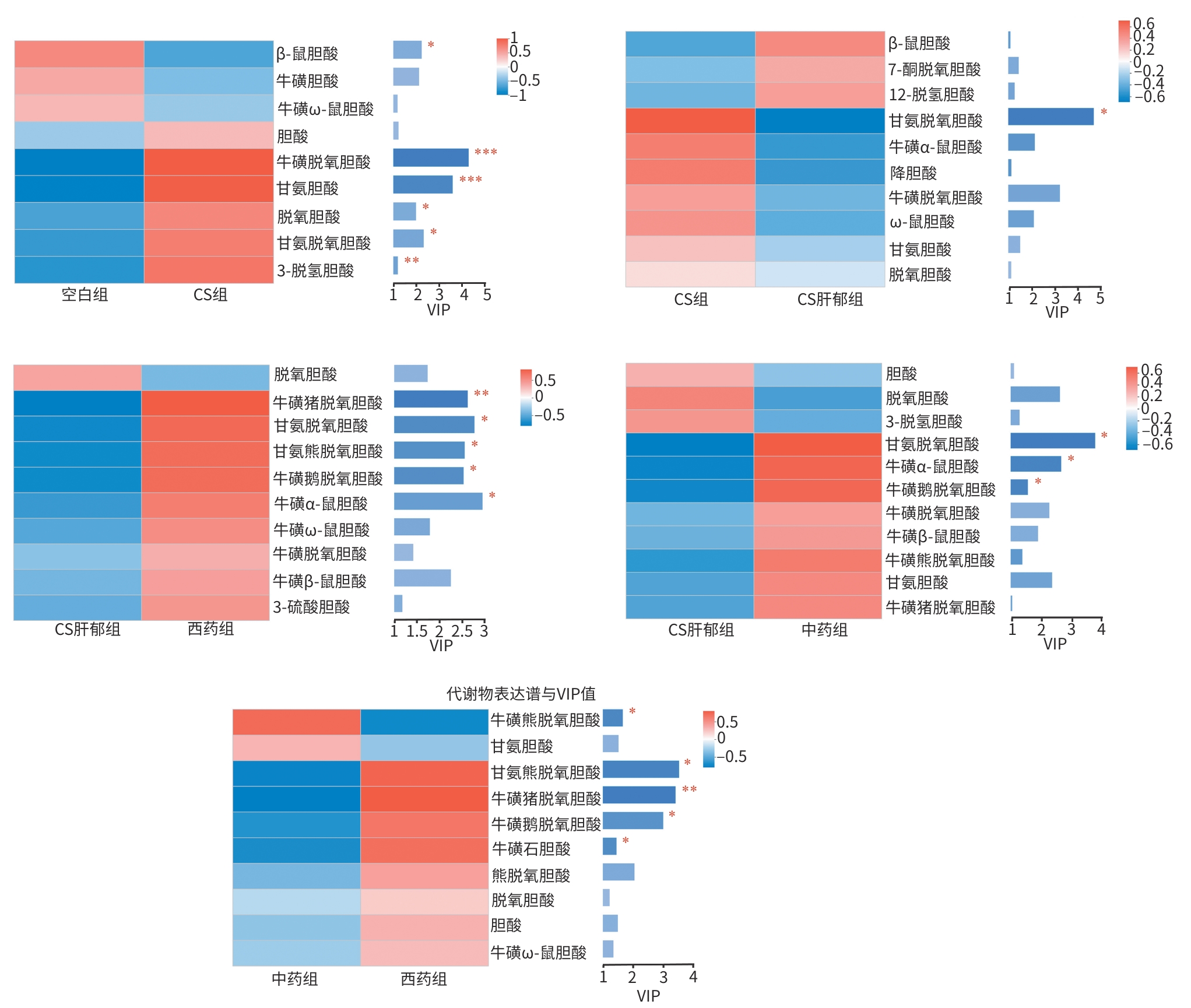
目的 探讨柴胡疏肝散加减方对胆囊胆固醇结石(CS)肝郁证胆囊异常舒张的作用机制,进而为临床用药提供依据。 方法 采用“高脂致石饲料+慢性不可预知轻度应激(CUMS)”建立CS肝郁证小鼠模型。将45只C57BL/6雄性小鼠随机分为空白组(6只,普通饲料)和CS造模组(39只,高脂致石饲料)。CS成模后,将CS造模组再次随机分为CS组、CS肝郁组、中药组(柴胡疏肝散加减方)和西药组(熊去氧胆酸),每组各9只;继续高脂致石饲料喂养,除CS组外,其余3组进行21天的CUMS造模,干预结束后取材。检测血清胆囊收缩素(CCK)、肝功能、血脂相关指标;肝、胆囊组织行苏木精-伊红染色;RT-qPCR与Western Blot分别检测肠道G蛋白偶联胆汁酸受体1(TGR5)、胰高血糖素样肽-1/2(GLP-1/2)和胆囊TGR5、胰高血糖素样肽-2受体(GLP-2R)的mRNA及蛋白表达;代谢组学检测肠内容物胆汁酸组成。计量资料两组间比较采用成组t检验;多组间比较采用单因素方差分析,进一步两两比较采用LSD-t法或Games-Howell法。 结果 与空白组相比,CS组出现明显胆囊结石、胆汁浑浊,肝脂肪变性及胆囊壁结构异常,行为学结果表明焦虑与抑郁样行为增加;胆汁总胆固醇、血清丙氨酸氨基转移酶、天冬氨酸氨基转移酶及低密度脂蛋白水平显著升高,胆汁总胆汁酸(TBA)、血清CCK及高密度脂蛋白(HDL)水平显著降低(P值均<0.05);肠GLP-1/2、TGR5 mRNA表达均显著升高,胆GLP-2R、TGR5的蛋白表达显著升高,mRNA表达显著降低(P值均<0.05);肠内容物多种胆汁酸成分显著改变(P值均<0.05)。与CS组相比,CS肝郁组病理及行为学表现进一步加重,胆汁酸成分改变,肠TGR5、GLP-1/2及胆TGR5、GLP-2R的蛋白和mRNA表达均升高(P值均<0.01)。与CS肝郁组相比,两用药组均能改善胆囊形态,减轻结石及肝损伤,恢复肝功能及血脂水平;并且均可显著降低肠TGR5、GLP-1/2及胆TGR5、GLP-2R的蛋白和mRNA表达(P值均<0.05);甘氨脱氧胆酸、牛磺α-鼠胆酸与牛磺鹅脱氧胆酸在中药组显著上调(P值均<0.05),西药组则见牛磺猪脱氧胆酸、牛磺α-鼠胆酸、牛磺鹅脱氧胆酸、甘氨脱氧胆酸和甘氨熊脱氧胆酸显著上调(P值均<0.05)。与西药组相比,中药组行为学改善更明显,胆汁TBA和血清HDL更高(P值均<0.01),肠TGR5、GLP-1/2及胆TGR5、GLP-2R的蛋白表达降低,肠TGR5的mRNA表达降低(P值均<0.01),牛磺熊脱氧胆酸上调,而甘氨熊脱氧胆酸、牛磺猪脱氧胆酸、牛磺鹅脱氧胆酸和牛磺石胆酸显著下调(P值均<0.05)。 结论 柴胡疏肝散加减方可通过调控胆汁酸-TGR5轴改善CS肝郁证肝功能及胆囊异常舒张,发挥疏肝解郁、行气利胆的治疗作用。 -
关键词:
- 胆囊结石病 /
- 肝郁 /
- 柴胡疏肝散 /
- 小鼠,近交C57BL
Abstract:Objective To investigate the mechanism of action of modified Chaihu Shugan Powder in the treatment of abnormal gallbladder relaxation in gallbladder cholesterol stone (CS) with liver depression syndrome, and to provide a basis for clinical medication. Methods Mice were given a high-fat lithogenic diet combined with chronic unpredictable mild stress (CUMS) to establish a model of CS. A total of 45 male C57BL/6 mice were randomly divided into blank group (6 mice fed a normal diet) and CS group (39 mice fed a high-fat lithogenic diet). After CS modeling, the CS group was further randomly divided into four subgroups of CS group, CS liver depression group, traditional Chinese medicine group (treated with modified Chaihu Shugan Powder), and Western medicine group (treated with ursodeoxycholic acid), with 9 mice in each group. All subgroups were fed with the high-fat lithogenic diet, and all mice except those in the CS group were given 21 days of CUMS for modeling. Samples were collected after intervention. The serum levels of cholecystokinin (CCK), liver function parameters, and blood lipid profiles were measured; HE staining was performed for liver and gallbladder tissue; qPCR and Western blot were used to measure the mRNA and protein expression levels of G protein-coupled bile acid receptor 1 (TGR5) and glucagon-likepeptide-1/2 (GLP-1/2) in the intestine and TGR5 and glucagon-like peptide-2 receptor (GLP-2R) in gallbladder; metabolomics methods were used to determine bile acid composition in intestinal contents. The independent-samples t-test was used for comparison of continuous data between two groups; a one-way analysis of variance was used for comparison between multiple groups, and the least significant difference t-test or the Games-Howell method was used for further comparison between two groups. Results Compared with the blank group, the CS group showed significant gallstone formation, bile turbidity, hepatic steatosis, abnormal gallbladder wall structure, and significant increases in anxiety- and depression-like behaviors based on behavioral tests; significant increases in the level of total cholesterol in bile and the serum levels of alanine aminotransferase, aspartate aminotransferase, and low-density lipoprotein and significant reductions in the level of total bile acid (TBA) in bile and the serum levels of CCK and high-density lipoprotein (HDL) (all P<0.05); significant increases in the mRNA expression levels of GLP-1/2 and TGR5 in the intestine and the protein expression levels of GLP-2R and TGR5 in the gallbladder and significant reductions in the mRNA expression levels of GLP-2R and TGR5 in the gallbladder (all P<0.05); significant changes in multiple bile acid components in intestinal contents (all P<0.05). Compared with the CS group, the CS liver depression group had further aggravation of pathological and behavioral manifestations, changes in bile acid composition, significant increases in the protein and mRNA expression levels of TGR5 and GLP-1/2 in the intestine, and significant increases in the protein and mRNA expression levels of TGR5 and GLP-2R in the gallbladder (all P<0.01). Compared with the CS liver depression group, both treatment groups had an improvement in gallbladder morphology, alleviation of stones and liver injury, and recovery of liver function and blood lipid levels, as well as significant reductions in the protein and mRNA expression levels of TGR5 and GLP-1/2 in the intestine and TGR5 and GLP-2R in the gallbladder (all P<0.05); the traditional Chinese medicine group showed significant increases in glycodeoxycholic acid (GDCA), tauro-α-muricholic acid (T-α-MCA), and taurochenodeoxycholic acid (TCDCA) (all P<0.05), while the Western medicine group showed significant increases in taurohyodeoxycholic acid, T-α-MCA, TCDCA, GDCA, and glycoursodeoxycholic acid (all P<0.05). Compared with the Western medicine group, the traditional Chinese medicine group had significantly greater behavioral improvements, significantly higher levels of TBA in bile and serum HDL (both P<0.01), significant reductions in the protein expression levels of TGR5 and GLP-1/2 in the intestine and TGR5 and GLP-2R in the gallbladder, and a significant reduction in the mRNA expression level of TGR5 in the intestine (all P<0.01), as well as a significant increase in tauroursodeoxycholic acid and significant reductions in glycoursodeoxycholic acid, taurohyodeoxycholic acid, TCDCA, and taurolithocholic acid (all P<0.05). Conclusion Modified Chaihu Shugan Powder can improve liver function and abnormal gallbladder relaxation in CS with liver depression syndrome by regulating the bile acid-TGR5 axis, thereby exerting the therapeutic effect of soothing the liver, resolving depression, moving Qi, and promoting bile flow. -
Key words:
- Cholecystolithiasis /
- Stagnation of Liver Qi /
- Chai Hu Shu Gan San /
- Mice, Inbred C57BL
-
表 1 引物序列
Table 1. Primer sequences
引物 序列(5'-3') 长度(bp) GAPDH 151 F 5'-TGTGTCCGTCGTGGATCTGA-3' R 5'-TTGCTGTTGAAGTCGCAGGAG-3' GLP-1/2 118 F 5'-CCAGAAGAAGTCGCCATTGCC-3' R 5'-TCAGCCAGTTGATGAAGTCCCT-3' GLP-2R 190 F 5'-TCTTCTTGTTCCTTCGAAAACTGC-3' R 5'-GAGCGGCAGGAGGCAGAAAT-3' TGR5 135 F 5'-TTATGGCCTCCTGTTGCCTG-3' R 5'-GCCAGGGTTGAGGGTACATC-3' 注:GAPDH,甘油醛-3-磷酸脱氢酶,本实验所选内参基因;GLP-1/2,胰高血糖素样肽-1/2;GLP-2R,胰高血糖素样肽-2受体;TGR5,G蛋白偶联胆汁酸受体1。
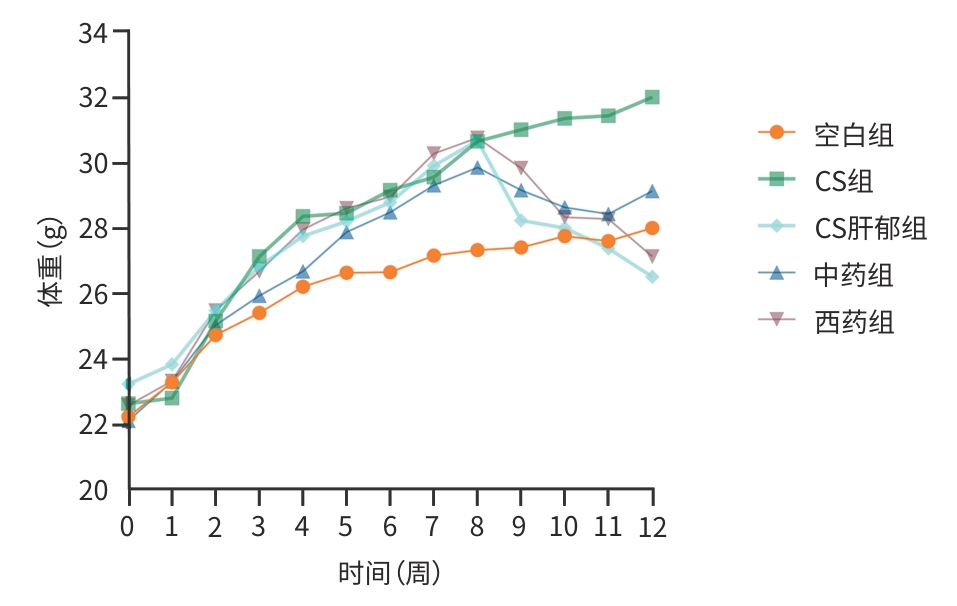
表 2 各组小鼠肝郁造模前后体重、肝重及肝脏系数变化
Table 2. Body weight, liver weight and liver coefficient of mice in each group before and after liver depression modeling
组别 动物数(只) 造模前体重(g) 造模后 体重(g) 肝重(g) 肝脏系数(%) 空白组 6 27.35±0.75 28.01±0.35 1.27±0.06 44.55±2.12 CS组 9 30.68±0.681) 32.14±0.681) 1.89±0.061) 61.12±1.501) CS肝郁组 9 30.72±0.401) 26.13±0.652) 2.10±0.052) 78.52±2.932) 中药组 9 29.87±0.121) 29.11±0.973) 1.77±0.103) 62.80±2.513) 西药组 9 30.77±0.621) 27.11±1.103)4) 1.85±0.083)4) 67.94±3.533)4) F值 47.21 89.39 120.70 156.53 P值 <0.001 <0.001 <0.001 <0.001 注:与空白组相比,1)P<0.01;与CS组相比,2)P<0.01;与CS肝郁组相比,3)P<0.01;与中药组相比,4)P<0.05。CS,胆固醇结石。肝脏系数=肝重/体重×100%。
表 3 各组小鼠旷场实验
Table 3. Open field test of mice in each group
组别 动物数(只) 移动总距离(mm) 中心停留时间(s) 造模前 造模后 造模前 造模后 空白组 4 17 015.81±400.57 18 122.23±1 450.42 43.27±4.21 45.01±7.25 CS组 4 15 913.23±2 018.68 15 734.50±1 381.681) 40.25±2.88 31.61±7.401) CS肝郁组 4 15 154.36±1 453.04 8 930.80±807.282) 40.90±11.27 18.08±5.682) 中药组 4 16 156.59±939.05 13 356.06±547.003) 36.01±7.34 29.16±3.573) 西药组 4 15 610.81±1 458.77 9 399.90±992.704) 35.03±8.07 23.99±4.63 F值 1.029 53.202 0.883 11.684 P值 0.424 <0.001 0.497 <0.001 注:与空白组相比,1)P<0.01;与CS组相比,2)P<0.01;与CS肝郁组相比,3)P<0.05;与中药组相比,4)P<0.01。CS,胆固醇结石。
表 4 各组小鼠强迫游泳实验不动时间
Table 4. Immobility time of forced swimming test in mice of each group
组别 动物数(只) 造模前(s) 造模后(s) 空白组 4 45.71±7.65 63.46±5.83 CS组 4 40.39±9.47 78.02±23.01 CS肝郁组 4 38.09±6.44 105.15±6.091) 中药组 4 43.46±9.02 75.76±8.512) 西药组 4 46.35±9.70 89.42±18.31 F值 0.678 4.902 P值 0.617 0.010 注:与CS组相比,1)P<0.05;与CS肝郁组相比,2)P<0.05。
表 5 各组小鼠悬尾实验不动时间
Table 5. Immobility time of tail suspension test in each group of mice
组别 动物数(只) 造模前(s) 造模后(s) 空白组 4 86.75±25.57 90.59±19.33 CS组 4 100.86±4.51 100.68±27.50 CS肝郁组 4 94.96±25.90 157.17±22.981) 中药组 4 86.33±17.67 100.02±5.872) 西药组 4 92.97±8.87 105.65±28.522) F值 0.424 5.594 P值 0.789 0.006 注:与CS组相比,1)P<0.01;与CS肝郁组相比,2)P<0.01。
表 6 各组小鼠糖水实验糖水消耗率
Table 6. Sugar water consumption rate of mice in each group
组别 动物数(只) 造模前(%) 造模后(%) 空白组 4 57.43±2.43 59.46±4.79 CS组 4 53.15±9.73 54.60±1.11 CS肝郁组 4 55.79±2.54 39.09±4.321) 中药组 4 57.20±7.68 56.75±3.382) 西药组 4 56.64±4.33 44.64±10.113) F值 0.327 9.574 P值 0.856 <0.001 注:与CS组相比,1)P<0.01;与CS肝郁组相比,2)P<0.01;与中药组相比,3)P<0.01。CS,胆固醇结石。
表 7 各组小鼠胆汁TC、TBA及血清CCK含量
Table 7. Content of TC and TBA in bile and CCK in serum of mice in each group
组别 动物数
(只)TC(mmol/L) TBA(μmol/L) CCK(pg/mL) 空白组 4 2.10±0.25 17.05±0.79 313.00±6.14 CS组 4 3.12±0.351) 12.47±0.531) 251.07±6.981) CS肝郁组 4 4.34±0.352) 10.50±1.002) 174.13±23.542) 中药组 4 3.33±0.143) 14.76±0.883) 229.72±6.13 西药组 4 3.57±0.143) 12.76±0.733)4) 198.46±33.02 F值 46.752 48.327 32.220 P值 <0.001 <0.001 <0.001 注:与空白组相比,1)P<0.01;与CS组相比,2)P<0.05;与CS肝郁组相比,3)P<0.01;与中药组相比,4)P<0.01。TC,总胆固醇;TBA,总胆汁酸;CCK,胆囊收缩素;CS,胆固醇结石。
表 8 各组小鼠血清ALT、AST、HDL和LDL含量
Table 8. Serum ALT, AST, HDL and LDL levels in each group of mice
组别 动物数(只) ALT(U/L) AST(U/L) HDL(mmol/L) LDL(mmol/L) 空白组 5 64.23±9.20 109.13±9.55 1.86±0.23 0.35±0.04 CS组 5 194.28±33.581) 211.23±38.591) 1.47±0.211) 1.44±0.141) CS肝郁组 5 249.22±51.48 270.80±25.78 1.02±0.262) 1.91±0.352) 中药组 5 120.21±27.933) 204.82±15.403) 1.70±0.173) 1.20±0.133) 西药组 5 172.49±14.44 183.02±17.283) 1.16±0.354) 1.35±0.243) F值 25.825 30.606 9.931 37.601 P值 <0.001 <0.001 <0.001 <0.001 注:与空白组相比,1)P<0.05;与CS组相比,2)P<0.05;与CS肝郁组相比,3)P<0.05;与中药组相比,4)P<0.01。ALT,丙氨酸氨基转移酶;AST,天冬氨酸氨基转移酶;HDL,高密度脂蛋白;LDL,低密度脂蛋白;CS,胆固醇结石。
表 9 各组小鼠肠GLP-1/2、TGR5与胆囊GLP-2R、TGR5的mRNA相对表达量
Table 9. Relative mRNA expression of intestinal GLP1/2, TGR5 and gallbladder GLP2R, TGR5 in each group of mice
组别 动物数(只) 肠GLP-1/2 肠TGR5 胆GLP-2R 胆TGR5 空白组 3 1.00±0.03 0.97±0.05 0.99±0.07 1.01±0.04 CS组 3 2.66±0.061) 1.21±0.041) 0.77±0.031) 0.84±0.101) CS肝郁组 3 5.39±0.292) 2.29±0.132) 1.32±0.182) 1.28±0.112) 中药组 3 3.16±0.173) 1.22±0.163) 0.94±0.083) 0.87±0.073) 西药组 3 3.57±0.603) 1.59±0.033)4) 0.93±0.083) 0.89±0.063) F值 105.225 111.967 16.664 19.635 P值 <0.001 <0.001 <0.001 <0.001 注:与空白组相比,1)P<0.05;与CS组相比,2)P<0.01;与CS肝郁组相比,3)P<0.05;与中药组相比,4)P<0.01。GLP-1/2,胰高血糖素样肽-1/2;TGR5,G蛋白偶联胆汁酸受体1;GLP-2R,胰高血糖素样肽-2受体;CS,胆固醇结石。
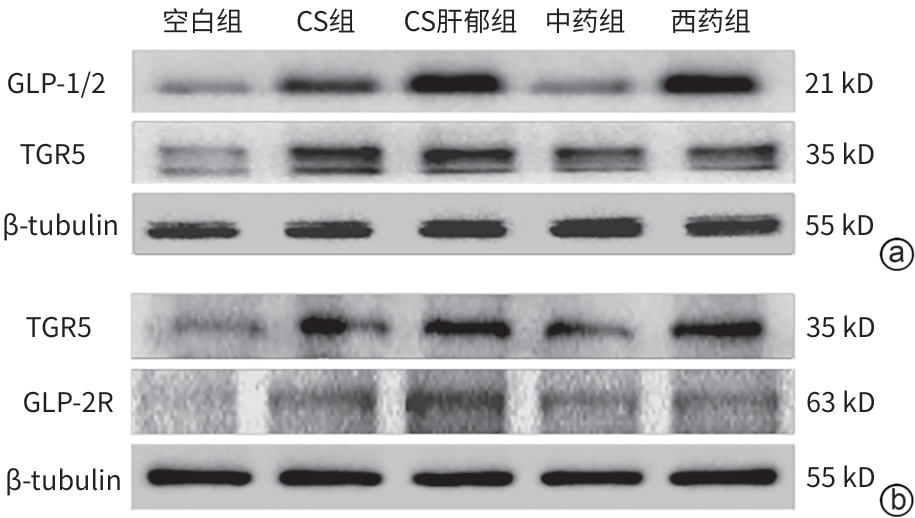
表 10 各组小鼠肠GLP-1/2、TGR5与胆囊GLP-2R、TGR5的蛋白相对表达量
Table 10. The relative protein expression of intestinal GLP-1/2, TGR5 and gallbladder GLP2-R, TGR5 in each group of mice
组别 动物数(只) 肠GLP-1/2 肠TGR5 胆GLP-2R 胆TGR5 空白组 3 0.25±0.01 0.47±0.07 0.63±0.05 0.37±0.03 CS组 3 0.50±0.041) 0.66±0.051) 1.03±0.111) 0.65±0.031) CS肝郁组 3 0.74±0.022) 0.94±0.022) 1.49±0.052) 1.07±0.042) 中药组 3 0.43±0.023) 0.67±0.053) 1.04±0.033) 0.62±0.043) 西药组 3 0.54±0.043)4) 0.80±0.033)4) 1.28±0.093)4) 0.76±0.073)4) F值 120.580 41.464 63.365 106.892 P值 <0.001 <0.001 <0.001 <0.001 注:与空白组相比,1)P<0.01;与CS组相比,2)P<0.01;与CS肝郁组相比,3)P<0.01;与中药组相比,4)P<0.01。GLP-1/2,胰高血糖素样肽-1/2;TGR5,G蛋白偶联胆汁酸受体1;GLP-2R,胰高血糖素样肽-2受体;CS,胆固醇结石。
-
[1] LU JH, LI YL, GUO RF, et al. Clinical features of patients with recurrent primary common bile duct stones after cholecystectomy[J]. J Clin Hepatol, 2025, 41( 1): 118- 126. DOI: 10.12449/JCH250118.芦建慧, 李勇利, 郭瑞芳, 等. 胆囊切除术后原发性胆总管结石复发患者的临床特征分析[J]. 临床肝胆病杂志, 2025, 41( 1): 118- 126. DOI: 10.12449/JCH250118. [2] HJALTADÓTTIR K, HARALDSDÓTTIR KH, MÖLLER PH. Gallstones-review[J]. Læknablaðið, 2020, 106( 10): 464- 472. DOI: 10.17992/lbl.2020.10.602. [3] LI JQ, ZHANG GX. Research advances in the risk factors for recurrence of common bile duct stone after choledocholithotomy[J]. J Clin Hepatol, 2023, 39( 1): 231- 237. DOI: 10.3969/j.issn.1001-5256.2023.01.036.李积强, 张桂信. 胆总管取石术后结石复发危险因素的研究进展[J]. 临床肝胆病杂志, 2023, 39( 1): 231- 237. DOI: 10.3969/j.issn.1001-5256.2023.01.036. [4] TENG JH, CHEN WT, PAN M, et al. Formation mechanism and surgical treatment status of cholelithiasis[J]. Acta Univ Med Anhui, 2024, 59( 8): 1489- 1494. DOI: 10.19405/j.cnki.issn1000-1492.2024.08.030.滕金豪, 陈伟棠, 潘孟, 等. 胆石症的形成机制及外科治疗现状[J]. 安徽医科大学学报, 2024, 59( 8): 1489- 1494. DOI: 10.19405/j.cnki.issn1000-1492.2024.08.030. [5] SONG B, WEN GQ, WANG L. Intestinal microorganisms and bile acid metabolism[J]. J Microbiol, 2021, 41( 3): 107- 112. DOI: 10.3969/j.issn.1005-7021.2021.03.016.宋波, 文国琴, 王蔺. 胆汁酸代谢与肠道微生物[J]. 微生物学杂志, 2021, 41( 3): 107- 112. DOI: 10.3969/j.issn.1005-7021.2021.03.016. [6] LI M, MA CY. Exploration of the biological basis of“liver controlling conveyance and dispersion” in TCM based on bile acid signal[J]. J Shanxi Univ Chin Med, 2023, 24( 1): 110- 113. DOI: 10.19763/j.cnki.2096-7403.2023.01.22.李鸣, 马重阳. 基于胆汁酸信号探讨中医“肝主疏泄”的生物学基础[J]. 山西中医药大学学报, 2023, 24( 1): 110- 113. DOI: 10.19763/j.cnki.2096-7403.2023.01.22. [7] BERR F, KULLAK-UBLICK GA, PAUMGARTNER G, et al. 7 alpha-dehydroxylating bacteria enhance deoxycholic acid input and cholesterol saturation of bile in patients with gallstones[J]. Gastroenterology, 1996, 111( 6): 1611- 1620. DOI: 10.1016/s0016-5085(96)70024-0. [8] AKAO T, AKAO T, HATTORI M, et al. 3 beta-Hydroxysteroid dehydrogenase of Ruminococcus sp. from human intestinal bacteria[J]. J Biochem, 1986, 99( 5): 1425- 1431. DOI: 10.1093/oxfordjournals.jbchem.a135612. [9] MA XH, SUN YB, CEN YY, et al. Advances in effect of bile acid metabolism on cholesterol gallstone disease[J/CD]. Electron J Metab Nutr Cancer, 2023, 10( 3): 430- 436. DOI: 10.16689/j.cnki.cn11-9349/r.2023.03.020.马先豪, 孙岩波, 岑云云, 等. 胆汁酸代谢对胆固醇结石形成影响的研究进展[J/CD]. 肿瘤代谢与营养电子杂志, 2023, 10( 3): 430- 436. DOI: 10.16689/j.cnki.cn11-9349/r.2023.03.020. [10] YUSTA B, MATTHEWS D, FLOCK GB, et al. Glucagon-like peptide-2 promotes gallbladder refilling via a TGR5-independent, GLP-2R-dependent pathway[J]. Mol Metab, 2017, 6( 6): 503- 511. DOI: 10.1016/j.molmet.2017.03.006. [11] GETHER IM, NEXØE-LARSEN C, KNOP FK. New avenues in the regulation of gallbladder motility-implications for the use of glucagon-like peptide-derived drugs[J]. J Clin Endocrinol Metab, 2019, 104( 7): 2463- 2472. DOI: 10.1210/jc.2018-01008. [12] REHFELD JF, KNOP FK, ASMAR A, et al. Cholecystokinin secretion is suppressed by glucagon-like peptide-1: Clue to the mechanism of the adverse gallbladder events of GLP-1-derived drugs[J]. Scand J Gastroenterol, 2018, 53( 12): 1429- 1432. DOI: 10.1080/00365521.2018.1530297. [13] FU X, WANG XM, ZHANG Y, et al. Shugan Xiaoshi decoction in treatment of cholelithiasis with liver depressionand qi stagnation syndrome[J]. Acta Chin Med, 2024, 39( 11): 2465- 2470. DOI: 10.16368/j.issn.1674-8999.2024.11.406.付鑫, 王雪梅, 张雨, 等. 疏肝消石汤治疗胆石症肝郁气滞证[J]. 中医学报, 2024, 39( 11): 2465- 2470. DOI: 10.16368/j.issn.1674-8999.2024.11.406. [14] ZHANG Z, ZHAO JJ, WANG YZ, et al. Research progress in pharmacological effects and mechanism of Chaihu Shugan Powder[J]. Chin J Inf Tradit Chin Med, 2017, 24( 9): 128- 131. DOI: 10.3969/j.issn.1005-5304.2017.09.035.张喆, 赵静洁, 王永志, 等. 柴胡疏肝散药理作用及机制研究进展[J]. 中国中医药信息杂志, 2017, 24( 9): 128- 131. DOI: 10.3969/j.issn.1005-5304.2017.09.035. [15] MIN L, LIN XJ, ZHOU ZH, et al. Effects of Chaihu Shugan Powder on gallbladder contractile function in mice with gallbladder cholesterol stones[J]. Fujian J Tradit Chin Med, 2023, 54( 3): 23- 26. DOI: 10.13260/j.cnki.jfjtcm.2023.03007.闵莉, 林雪娟, 周智慧, 等. 柴胡疏肝散对胆囊胆固醇结石小鼠胆囊收缩功能的影响[J]. 福建中医药, 2023, 54( 3): 23- 26. DOI: 10.13260/j.cnki.jfjtcm.2023.03007. [16] ZHOU YN. Mechanism of soothing the liver, eliminating dampness and heat on gallbladder dynamics in CS mice[D]. Fuzhou: Fujian University of Traditional Chinese Medicine, 2018.周亚男. 疏肝清利湿热对CS小鼠胆囊动力学影响的机制研究[D]. 福州: 福建中医药大学, 2018. [17] ZHANG Z, CAO DF. Effect of Chaishao Liujunzi decoction combined with anethol trithione tablets on abdominal pain, gallbladder systolic function and inflammatory response of patients with chronic cholecystitis[J]. Drug Eval, 2024, 21( 8): 1011- 1014. DOI: 10.19939/j.cnki.1672-2809.2024.08.25.张珍, 曹丹凤. 柴芍六君子汤联合茴三硫片治疗慢性胆囊炎对患者腹痛程度、胆囊收缩功能及炎症反应的影响[J]. 药品评价, 2024, 21( 8): 1011- 1014. DOI: 10.19939/j.cnki.1672-2809.2024.08.25. [18] CAO HF, ZHANG Y, WEI ST, et al. Effect of modified Chaihu Shugansan on gallbladder function and inflammatory cytokines levels in treatment of chronic cholecystitis cholelithiasis[J]. Chin J Exp Tradit Med Formulae, 2021, 27( 15): 63- 67. DOI: 10.13422/j.cnki.syfjx.20210331.曹海芳, 张瑜, 魏胜泰, 等. 柴胡疏肝散加减治疗慢性胆囊炎胆石症及胆囊功能和炎症因子的影响[J]. 中国实验方剂学杂志, 2021, 27( 15): 63- 67. DOI: 10.13422/j.cnki.syfjx.20210331. [19] Branch of Gastrointestinal Diseases, China Association of Chinese Medicine. Expert consensus on traditional Chinese medicine diagnosis and treatment of(acute and chronic) cholecystitis and cholelithiasis(2023)[J]. Chin J Integr Trad West Med Dig, 2024, 32( 10): 839- 848. DOI: 10.3969/j.issn.1671-038X.2024.10.01.中华中医药学会脾胃病分会.(急、慢性)胆囊炎、胆石症中医诊疗专家共识(2023)[J]. 中国中西医结合消化杂志, 2024, 32( 10): 839- 848. DOI: 10.3969/j.issn.1671-038X.2024.10.01. [20] ZHOU ZH. Study on the mechanism of cholesterol gallstones in regulating gallbladder motility from DAG-PKC pathway based on“Fu organs for general purpose”[D]. Fuzhou: Fujian University of Traditional Chinese Medicine, 2021. DOI: 10.27021/d.cnki.gfjzc.2021.000079.周智慧. 基于“腑以通为用”从DAG-PKC通路调控胆囊动力的胆固醇结石机制研究[D]. 福州: 福建中医药大学, 2021. DOI: 10.27021/d.cnki.gfjzc.2021.000079. [21] WANG SY. Molecular biological mechanism of damp-heat syndrome of gallbladder cholesterol stones based on the regulation of FXR/FGF15/FGFR4 pathway by intestinal flora[D]. Fuzhou: Fujian University of Traditional Chinese Medicine, 2022. DOI: 10.27021/d.cnki.gfjzc.2022.000003.王素英. 基于肠道菌群调控FXR/FGF15/FGFR4通路探讨胆囊胆固醇结石湿热证的分子生物学机制[D]. 福州: 福建中医药大学, 2022. DOI: 10.27021/d.cnki.gfjzc.2022.000003. [22] NOLLET M. Models of depression: Unpredictable chronic mild stress in mice[J]. Curr Protoc, 2021, 1( 8): e208. DOI: 10.1002/cpz1.208. [23] LU YJ, ZHANG S, ZHAO Q, et al. A review of behavioral evaluation of depression in rodents[J]. Lab Anim Sci, 2023, 40( 6): 87- 93. DOI: 10.3969/j.issn.1006-6179.2023.06.016.卢宇佳, 张珊, 赵谦, 等. 啮齿类动物抑郁相关行为学评价[J]. 实验动物科学, 2023, 40( 6): 87- 93. DOI: 10.3969/j.issn.1006-6179.2023.06.016. [24] WANG YN, ZHANG XY, LIU YP, et al. Traditional Chinese medicine regulates the gut microbiota-bile acids-FXR axis to intervene in the development of colorectal cancer[J]. Acta Pharm Sin, 2024, 59( 11): 3027- 3041. DOI: 10.16438/j.0513-4870.2024-0568.王亚妮, 张潇予, 刘玉萍, 等. 肠道菌群-胆汁酸-FXR轴干预结直肠癌的研究进展及中药干预的现状分析[J]. 药学学报, 2024, 59( 11): 3027- 3041. DOI: 10.16438/j.0513-4870.2024-0568. [25] LIU C, WANG ZY, ZHANG N, et al. Exploring the mechanism of Houpo Sanwu Decoction in regulating bile components in rabbits after cholecystectomy based on the FXR/TGR5 bile acid receptor signaling pathway[J/OL]. Acta Chin Med, 1- 10[ 2024-08-05]. https://link.cnki.net/urlid/41.1411.R.20240805.1321.097. https://link.cnki.net/urlid/41.1411.R.20240805.1321.097刘昌, 王兆阳, 张楠, 等. 基于胆汁酸受体FXR/TGR5信号通路探讨厚朴三物汤调节胆囊切除术后兔胆汁组分的作用机制[J/OL]. 中医学报, 1- 10[ 2024-08-05]. https://link.cnki.net/urlid/41.1411.R.20240805.1321.097. https://link.cnki.net/urlid/41.1411.R.20240805.1321.097 [26] WARD JBJ, LAJCZAK NK, KELLY OB, et al. Ursodeoxycholic acid and lithocholic acid exert anti-inflammatory actions in the colon[J]. Am J Physiol Gastrointest Liver Physiol, 2017, 312( 6): G550- G558. DOI: 10.1152/ajpgi.00256.2016. [27] WANG YH, YU XY, SHEN L. Regulation of NF-κB pathway by bile acid receptor TGR5 in DSS induced mouse colitis[J]. Chin J Gastroenterol Hepatol, 2024, 33( 11): 1459- 1463. DOI: 10.3969/j.issn.1006-5709.2024.11.008.王宇豪, 余晓云, 沈磊. 胆汁酸受体TGR5对DSS诱导的小鼠结肠炎NF-κB通路的调节作用[J]. 胃肠病学和肝病学杂志, 2024, 33( 11): 1459- 1463. DOI: 10.3969/j.issn.1006-5709.2024.11.008. [28] POOLE DP, GODFREY C, CATTARUZZA F, et al. Expression and function of the bile acid receptor GpBAR1(TGR5) in the murine enteric nervous system[J]. Neurogastroenterol Motil, 2010, 22( 7): 814- 825. DOI: 10.1111/j.1365-2982.2010.01487.x. [29] HANSEN NL, BRØNDEN A, NEXØE-LARSEN CC, et al. Glucagon-like peptide 2 inhibits postprandial gallbladder emptying in man: A randomized, double-blinded, crossover study[J]. Clin Transl Gastroenterol, 2020, 11( 12): e00257. DOI: 10.14309/ctg.0000000000000257. [30] HUNT JE, BILLESCHOU A, WINDELØV JA, et al. Pharmacological activation of TGR5 promotes intestinal growth via a GLP-2-dependent pathway in mice[J]. Am J Physiol Gastrointest Liver Physiol, 2020, 318( 5): G980- G987. DOI: 10.1152/ajpgi.00062.2020. [31] BIDAULT-JOURDAINNE V, MERLEN G, GLÉNISSON M, et al. TGR5 controls bile acid composition and gallbladder function to protect the liver from bile acid overload[J]. JHEP Rep, 2021, 3( 2): 100214. DOI: 10.1016/j.jhepr.2020.100214. [32] CHENG JL. Retrospective study of TCM syndrome differentiation of cholelithiasis and its distribution in metabolic syndrome[D]. Hangzhou: Zhejiang Chinese Medical University, 2024. DOI: 10.27465/d.cnki.gzzyc.2024.000041.程建林. 胆石症中医证候分型与代谢综合征分布规律的回顾性研究[D]. 杭州: 浙江中医药大学, 2024. DOI: 10.27465/d.cnki.gzzyc.2024.000041. [33] LI LL. Cholithiasis on TCM syndromes study and its retrospective analysis of curative effect of TCM[D]. Nanning: Guangxi University of Chinese Medicine, 2021. DOI: 10.27879/d.cnki.ggxzy.2021.000105.李璐璐. 胆石症中医证候研究及中医药治疗疗效回顾性分析[D]. 南宁: 广西中医药大学, 2021. DOI: 10.27879/d.cnki.ggxzy.2021.000105. [34] LU YJ, ZHANG S, SHI W, et al. Effects of Chaihu-Shugan San on behavior and hippocampal neurogenesis in depressive model mice[J]. Chin J Behav Med Brain Sci, 2022, 31( 3): 198- 204. DOI: 10.3760/cma.j.cn371468-20210918-00538.卢宇佳, 张珊, 史伟, 等. 柴胡疏肝散对抑郁模型小鼠行为及海马神经再生的影响[J]. 中华行为医学与脑科学杂志, 2022, 31( 3): 198- 204. DOI: 10.3760/cma.j.cn371468-20210918-00538. [35] YU YQ, WANG LL, WANG JJ, et al. Antidepressant effects of Chaihu Shugan Powder alcohol extracts in mice depression model[J]. Acta Neuropharmacol, 2014, 4( 5): 8- 14. DOI: 10.3969/j.issn.2095-1396.2014.05.002.于亚青, 王林林, 王静静, 等. 柴胡疏肝散醇提物对抑郁模型小鼠的抗抑郁作用[J]. 神经药理学报, 2014, 4( 5): 8- 14. DOI: 10.3969/j.issn.2095-1396.2014.05.002. [36] LI AQ, HE QY. Discussion on the TCM syndrome differentiation system of‘categorized formula-formula syndrome-main TCM syndrome’[J]. China J Tradit Chin Med Pharm, 2021, 36( 4): 2148- 2151.李安琪, 何庆勇.“类方-方证-主证”辨证体系的探讨[J]. 中华中医药杂志, 2021, 36( 4): 2148- 2151. [37] SHEN ZY, ZHAO LY, WU D, et al. Exploration of the mechanism of liver injury caused by ethanol extract of Inonotus Obliquus based on liver metabolomics[J]. J Changchun Univ Chin Med, 2024, 40( 10): 1095- 1101. DOI: 10.13463/j.cnki.cczyy.2024.10.008.沈子扬, 赵良友, 吴丹, 等. 基于肝脏代谢组学探讨桦褐孔菌醇提物肝损伤机制[J]. 长春中医药大学学报, 2024, 40( 10): 1095- 1101. DOI: 10.13463/j.cnki.cczyy.2024.10.008. [38] WANG X, WANG XS, ZHOU BD, et al. Clinical observation on Chaihu Shugansan combined with Xuanfu Daizhetang in treating barrett’s esophagus with liver-stomach disharmony[J]. Chin J Exp Tradit Med Formulae, 2024, 30( 24): 10- 17. DOI: 10.13422/j.cnki.syfjx.20241122.王晓, 王晓素, 周秉舵, 等. 柴胡疏肝散合旋覆代赭汤治疗肝胃不和型Barrett食管的临床观察[J]. 中国实验方剂学杂志, 2024, 30( 24): 10- 17. DOI: 10.13422/j.cnki.syfjx.20241122. [39] WENG LR, WANG QH, CAI JH, et al. Progress in pharmacological action and clinical application of cholic acid[J]. Chin J Mod Appl Pharm, 2025, 42( 12): 2179- 2184. DOI: 10.13748/j.cnki.issn1007-7693.20232348.翁浪仁, 王秋红, 蔡家瀚, 等. 胆酸的药理作用及其临床应用研究进展[J]. 中国现代应用药学, 2025, 42( 12): 2179- 2184. DOI: 10.13748/j.cnki.issn1007-7693.20232348. [40] ZHAO JC, SHU Y, CHENG NS, et al. Changes of cholesterol metabolism in cholesterol gallstone formation in the rabbit[J]. Chin J Gen Surg, 2000, 9( 2): 124- 128. DOI: 10.3969/j.issn.1005-6947.2000.02.010.赵纪春, 舒晔, 程南生, 等. 胆囊结石中胆固醇代谢变化的实验研究[J]. 中国普通外科杂志, 2000, 9( 2): 124- 128. DOI: 10.3969/j.issn.1005-6947.2000.02.010. -



 PDF下载 ( 18747 KB)
PDF下载 ( 18747 KB)

 下载:
下载: