程序性细胞死亡受体-1抑制剂治疗中晚期非病毒性相关肝癌的效果及安全性分析
DOI: 10.3969/j.issn.1001-5256.2022.12.015
Effectiveness and safety of programmed cell death-1 inhibitor in the treatment of advanced non-HBV non-HCV-related hepatocellular carcinoma
-
摘要:
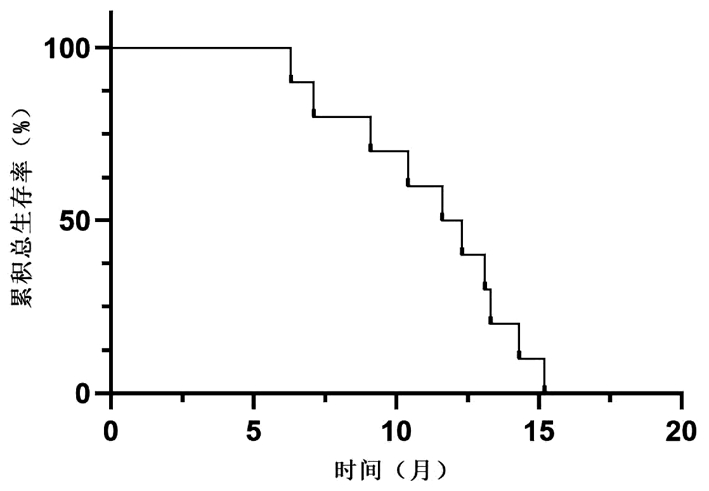
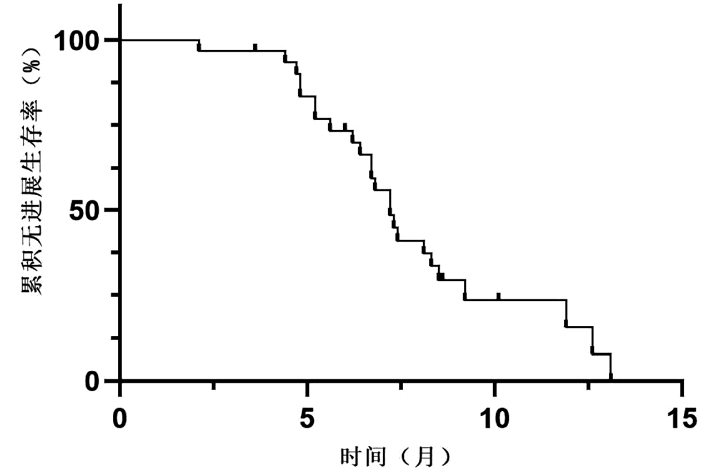
目的 研究国产程序性细胞死亡受体-1(PD-1)抑制剂在中晚期非病毒性相关肝癌(NBNC-HCC)中的临床疗效及不良反应。 方法 选取2019年6月—2022年2月徐州医科大学附属医院收治的使用国产PD-1抑制剂治疗的31例中晚期NBNC-HCC患者。分析患者疾病进展时间、客观缓解率、疾病控制率和不良反应发生情况。采用Kaplan-Meier法绘制生存曲线。 结果 在31例中晚期NBNC-HCC患者中,1例患者疗效评价为完全缓解,4例评价为部分缓解,6例评价为疾病稳定,20例评价为疾病进展,客观缓解率为16.1%,疾病控制率为35.5%,中位疾病进展时间为7.2(6.4~8.0)个月。不良反应发生率为61.30%,常见的不良反应为皮疹(29.03%)和高血压(22.58%),所有患者均无4级不良反应和不良反应相关死亡事件发生。 结论 本研究提示中晚期NBNC-HCC患者对PD-1抑制剂治疗的反应可能较弱,但不良反应可控,未来仍需多中心前瞻性试验进一步验证。 -
关键词:
- 肝肿瘤 /
- 程序性细胞死亡受体1 /
- 实体肿瘤疗效评价标准 /
- 药物相关性副作用和不良反应
Abstract:Objective To investigate the clinical effectiveness and adverse events of domestic programmed cell death -1 (PD-1) inhibitor in the treatment of advanced non-HBV non-HCV-related hepatocellular carcinoma (NBNC-HCC). Methods A totals of 31 patients with advanced NBNC-HCC who received domestic PD-1 inhibitor in the Affiliated Hospital of Xuzhou Medical University from June 2019 to February 2022 were retrospectively enrolled and their clinicopathological data were retrieved from their medical records and analyzed, i.e., the time to disease progression (TTP), disease control rate (DCR), objective response rate (ORR), and adverse events were recorded and statistically analyzed. The Kaplan-Meier method was used for survival analysis. Results Among these 31 patients, only one achieved the complete response and four achieved the partial response, and six had the stable disease, but 20 showed a disease progression, resulting in an ORR of 16.1% and a (DCR of 35.5%. The median TTP was 7.2 months [95% confidence interval: 6.4-8.0) months]. The incidence of adverse events was 61.30% and the common adverse events were skin rash (29.03%) and hypertension (22.58%). However, there was no grade 4 adverse reactions or related death in these patients. Conclusion Advanced NBNC-HCC patients had a relative weak response to the PD-1 inhibitor although the adverse events were controllable. Future multi-center prospective clinical trials are needed to validate the data. -
表 1 入组患者的临床资料
Table 1. Clinical information of enrolled patients
项目 数值 年龄(岁) 57.13±11.55 性别[例(%)] 男 20(64.5) 女 11(35.5) 病因[例(%)] NAFLD 24(77.4) 酒精性肝病 6(19.4) 自身免疫性肝病 1(3.2) 肿瘤大小[例(%)] <5 cm 13(41.9) ≥5 cm 18(58.1) 门静脉浸润[例(%)] 有 22(71.0) 无 9(29.0) 肝外转移[例(%)] 有 13(41.9) 无 18(58.1) Child-Pugh分级[例(%)] A 23(74.2) B 8(25.8) BCLC分期[例(%)] B 5(16.1) C 26(83.9) ECOG评分[例(%)] 0 3(9.7) 1 22(71.0) 2 6(19.4) 既往治疗方式[例(%)] TACE 19(61.3) 手术 6(19.4) 射频消融 4(12.9) 仑伐替尼 13(41.9) 索拉非尼 9(29.0) 阿帕替尼 6(19.4) 沙利度胺 8(25.8) 无 3(9.7) PD-1抑制剂[例(%)] 卡瑞利珠单抗 18(58.1) 信迪利单抗 9(29.0) 特瑞普利单抗 4(12.9) 注:NAFLD,非酒精性脂肪性肝病;TACE,经导管动脉化疗栓塞术。 表 2 入组患者的实验室资料
Table 2. Laboratory information of enrolled patients
项目 数值 AFP[例(%)] <400 ng/mL 13(42.0) ≥400 ng/mL 18(58.0) AST(U/L) 36.87±14.64 ALT(U/L) 27.74±13.32 Alb(g/L) 39.55±5.01 TBil(μmol/L) 17.57±8.76 PT(s) 12.04±1.05 表 3 入组患者肿瘤应答情况
Table 3. Tumor response of enrolled patients
项目 数值 CR(例) 1 PR(例) 4 SD(例) 6 PD(例) 20 ORR(%) 16.1(5/31) DCR(%) 35.5(11/31) 表 4 所有患者的不良反应情况
Table 4. Incidence of adverse reactions in all patients
项目 3级不良反应 总不良反应 皮疹[例(%)] 2(6.45) 9(29.03) 腹泻[例(%)] 1(3.23) 5(16.13) 疲劳[例(%)] 1(3.23) 6(19.35) 恶心[例(%)] 0 4(12.90) 蛋白尿[例(%)] 1(3.23) 5(16.13) 甲状腺炎[例(%)] 1(3.23) 3(9.68) 感觉异常[例(%)] 0 2(6.45) 高血压[例(%)] 3(9.68) 7(22.58) 口腔溃疡[例(%)] 0 4(12.90) 胆红素升高[例(%)] 0 2(6.45) 反应性皮肤毛细血管增生症[例(%)] 0 2(6.45) ALT升高[例(%)] 0 4(12.90) AST升高[例(%)] 1(3.23) 2(6.45) 肾上腺皮质功能减退[例(%)] 0 2(6.45) -
[1] SUNG H, FERLAY J, SIEGEL RL, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries[J]. CA Cancer J Clin, 2021, 71(3): 209-249. DOI: 10.3322/caac.21660. [2] NENU I, BREABAN I, PASCALAU S, et al. The future is now: beyond first line systemic therapy in hepatocellular carcinoma[J]. Transl Cancer Res, 2019, 8(Suppl 3): S261-S274. DOI: 10.21037/tcr.2018.11.23. [3] XUE X, LIAO W, XING Y. Comparison of clinical features and outcomes between HBV-related and non-B non-C hepatocellular carcinoma[J]. Infect Agent Cancer, 2020, 15: 11. DOI: 10.1186/s13027-020-0273-2. [4] BSISU I, RMILAH AA. Global elimination of chronic hepatitis[J]. N Engl J Med, 2019, 381(6): 589. DOI: 10.1056/NEJMc1908197. [5] SEKO Y, YAMAGUCHI K, ITOH Y. The genetic backgrounds in nonalcoholic fatty liver disease[J]. Clin J Gastroenterol, 2018, 11(2): 97-102. DOI: 10.1007/s12328-018-0841-9. [6] MALUCCIO M, COVEY A. Recent progress in understanding, diagnosing, and treating hepatocellular carcinoma[J]. CA Cancer J Clin, 2012, 62(6): 394-399. DOI: 10.3322/caac.21161. [7] CHUNG SY, KIM KJ, SEONG J. Biomarkers for locally advanced hepatocellular carcinoma patients treated with liver-directed combined radiotherapy[J]. Liver Cancer, 2022, 11(3): 247-255. DOI: 10.1159/000522000. [8] FINN RS, QIN S, IKEDA M, et al. Atezolizumab plus bevacizumab in unresectable hepatocellular carcinoma[J]. N Engl J Med, 2020, 382(20): 1894-1905. DOI: 10.1056/NEJMoa1915745. [9] EL-KHOUEIRY AB, SANGRO B, YAU T, et al. Nivolumab in patients with advanced hepatocellular carcinoma (CheckMate 040): an open-label, non-comparative, phase 1/2 dose escalation and expansion trial[J]. Lancet, 2017, 389(10088): 2492-2502. DOI: 10.1016/S0140-6736(17)31046-2. [10] ZHU AX, FINN RS, EDELINE J, et al. Pembrolizumab in patients with advanced hepatocellular carcinoma previously treated with sorafenib (KEYNOTE-224): a non-randomised, open-label phase 2 trial[J]. Lancet Oncol, 2018, 19(7): 940-952. DOI: 10.1016/S1470-2045(18)30351-6. [11] PFISTER D, NÚÑEZ NG, PINYOL R, et al. NASH limits anti-tumour surveillance in immunotherapy-treated HCC[J]. Nature, 2021, 592(7854): 450-456. DOI: 10.1038/s41586-021-03362-0. [12] JI F, NGUYEN MH. Cabozantinib plus atezolizumab in advanced hepatocellular carcinoma and the role of adjuvant antiviral therapy[J]. Lancet Oncol, 2022, 23(8): 962-963. DOI: 10.1016/S1470-2045(22)00383-7. [13] KELLEY RK, RIMASSA L, CHENG AL, et al. Cabozantinib plus atezolizumab versus sorafenib for advanced hepatocellular carcinoma (COSMIC-312): a multicentre, open-label, randomised, phase 3 trial[J]. Lancet Oncol, 2022, 23(8): 995-1008. DOI: 10.1016/S1470-2045(22)00326-6. [14] LENCIONI R, LLOVET JM. Modified RECIST (mRECIST) assessment for hepatocellular carcinoma[J]. Semin Liver Dis, 2010, 30(1): 52-60. DOI: 10.1055/s-0030-1247132. [15] European Association for the Study of the Liver. Corrigendum to "EASL Clinical Practice Guidelines: Management of hepatocellular carcinoma"[J Hepatol 69 (2018) 182-236][J]. J Hepatol, 2019, 70(4): 817. DOI: 10.1016/j.jhep.2019.01.020. [16] KUDO M, MATILLA A, SANTORO A, et al. CheckMate 040 cohort 5: A phase Ⅰ/Ⅱ study of nivolumab in patients with advanced hepatocellular carcinoma and Child-Pugh B cirrhosis[J]. J Hepatol, 2021, 75(3): 600-609. DOI: 10.1016/j.jhep.2021.04.047. [17] WANG F, QIN S, SUN X, et al. Reactive cutaneous capillary endothelial proliferation in advanced hepatocellular carcinoma patients treated with camrelizumab: data derived from a multicenter phase 2 trial[J]. J Hematol Oncol, 2020, 13(1): 47. DOI: 10.1186/s13045-020-00886-2. [18] ONZI G, MORETTI F, BALBINOT S S, et al. Hepatocellular carcinoma in non-alcoholic fatty liver disease with and without cirrhosis[J]. Hepato Res, 2019, 5: 7. DOI: 10.20517/2394-5079.2018.114. [19] DEGASPERI E, COLOMBO M. Distinctive features of hepatocellular carcinoma in non-alcoholic fatty liver disease[J]. Lancet Gastroenterol Hepatol, 2016, 1(2): 156-164. DOI: 10.1016/S2468-1253(16)30018-8. [20] XU W, ZHANG X, WU JL, et al. O-GlcNAc transferase promotes fatty liver-associated liver cancer through inducing palmitic acid and activating endoplasmic reticulum stress[J]. J Hepatol, 2017, 67(2): 310-320. DOI: 10.1016/j.jhep.2017.03.017. [21] SHEN ZQ, CHEN YF, CHEN JR, et al. CISD2 haploinsufficiency disrupts calcium homeostasis, causes nonalcoholic fatty liver disease, and promotes hepatocellular carcinoma[J]. Cell Rep, 2017, 21(8): 2198-2211. DOI: 10.1016/j.celrep.2017.10.099. [22] SCHUSTER S, CABRERA D, ARRESE M, et al. Triggering and resolution of inflammation in NASH[J]. Nat Rev Gastroenterol Hepatol, 2018, 15(6): 349-364. DOI: 10.1038/s41575-018-0009-6. [23] BOLAND P, WU J. Systemic therapy for hepatocellular carcinoma: beyond sorafenib[J]. Chin Clin Oncol, 2018, 7(5): 50. DOI: 10.21037/cco.2018.10.10. [24] BENSON AB, D'ANGELICA MI, ABBOTT DE, et al. Hepatobiliary cancers, version 2.2021, NCCN clinical practice guidelines in oncology[J]. J Natl Compr Canc Netw, 2021, 19(5): 541-565. DOI: 10.6004/jnccn.2021.0022. [25] General Office of National Health Commission. Standard for diagnosis and treatment of primary liver cancer (2022 edition)[J]. J Clin Hepatol, 2022, 38(2): 288-303. DOI: 10.3969/j.issn.1001-5256.2022.02.009.国家卫生健康委办公厅. 原发性肝癌诊疗指南(2022年版)[J]. 临床肝胆病杂志, 2022, 38(2): 288-303. DOI: 10.3969/j.issn.1001-5256.2022.02.009. [26] RODERBURG C, WREE A, DEMIR M, et al. The role of the innate immune system in the development and treatment of hepatocellular carcinoma[J]. Hepat Oncol, 2020, 7(1): HEP17. DOI: 10.2217/hep-2019-0007. [27] QIN S, REN Z, MENG Z, et al. Camrelizumab in patients with previously treated advanced hepatocellular carcinoma: a multicentre, open-label, parallel-group, randomised, phase 2 trial[J]. Lancet Oncol, 2020, 21(4): 571-580. DOI: 10.1016/S1470-2045(20)30011-5. [28] CHEN J, HU X, LI Q, et al. Effectiveness and safety of toripalimab, camrelizumab, and sintilimab in a real-world cohort of hepatitis B virus associated hepatocellular carcinoma patients[J]. Ann Transl Med, 2020, 8(18): 1187. DOI: 10.21037/atm-20-6063. -



 PDF下载 ( 1945 KB)
PDF下载 ( 1945 KB)

 下载:
下载: