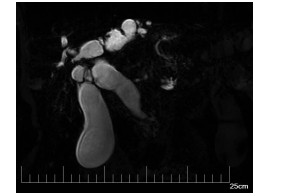
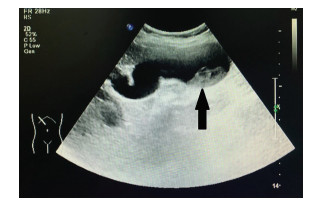
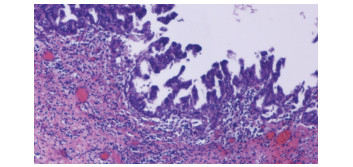
胆管内乳头状瘤合并肝左外叶萎缩1例报告
DOI: 10.3969/j.issn.1001-5256.2021.07.041
利益冲突声明:所有作者均声明不存在利益冲突。
作者贡献声明:欧阳敬中负责资料分析,撰写论文; 朱瑞利、周艳召、王征征、陈勋负责收集数据并对文字的知识性内容作批判性审阅; 周进学、李庆军负责拟定写作思路,指导撰写文章并最后定稿。
Intraductal papillary neoplasm of the bile duct with atrophy of the hepatic left lateral lobe: A case report
-
-
Key words:
- Papilloma, Intraductal /
- Bile Duct Neoplasms /
- Therapeutics
-
[1] KOHLI DR, SHAH TU. Board review vignette: Intraductal papillary neoplasm of the bile duct[J]. Am J Gastroenterol, 2018, 113(5): 639-641. DOI: 10.1038/s41395-018-0009-8. [2] CHEN TC, NAKANUMA Y, ZEN Y, et al. Intraductal papillary neoplasia of the liver associated with hepatolithiasis[J]. Hepatology, 2001, 34(4 Pt 1): 651-658. DOI: 10.1053/jhep.2001.28199. [3] NAKANUMA Y, SATO Y, HARADA K, et al. Pathological classification of intrahepatic cholangiocarcinoma based on a new concept[J]. World J Hepatol, 2010, 2(12): 419-427. DOI: 10.4254/wjh.v2.i12.419. [4] GORDON-WEEKS AN, JONES K, HARRISS E, et al. Systematic review and meta-analysis of current experience in treating IPNB: Clinical and pathological correlates[J]. Ann Surg, 2016, 263(4): 656-663. DOI: 10.1097/SLA.0000000000001426. [5] LUVIRA V, PUGKHEM A, BHUDHISAWASDI V, et al. Long-term outcome of surgical resection for intraductal papillary neoplasm of the bile duct[J]. J Gastroenterol Hepatol, 2017, 32(2): 527-533. DOI: 10.1111/jgh.13481. [6] KOMORI T, INOUE D, ZEN Y, et al. CT imaging comparison between intraductal papillary neoplasms of the bile duct and papillary cholangiocarcinomas[J]. Eur Radiol, 2019, 29(6): 3132-3140. DOI: 10.1007/s00330-018-5841-0. [7] LEE S, KIM MJ, KIM S, et al. Intraductal papillary neoplasm of the bile duct: Assessment of invasive carcinoma and long-term outcomes using MRI[J]. J Hepatol, 2019, 70(4): 692-699. DOI: 10.1016/j.jhep.2018.12.005. [8] LIU LN, XU HX, ZHENG SG, et al. Ultrasound findings of intraductal papillary neoplasm in bile duct and the added value of contrast-enhanced ultrasound[J]. Ultraschall Med, 2015, 36(6): 594-602. DOI: 10.1055/s-0034-1366672. [9] ROCHA FG, LEE H, KATABI N, et al. Intraductal papillary neoplasm of the bile duct: A biliary equivalent to intraductal papillary mucinous neoplasm of the pancreas?[J]. Hepatology, 2012, 56(4): 1352-1360. DOI: 10.1002/hep.25786. [10] SCHLITTER AM, BORN D, BETTSTETTER M, et al. Intraductal papillary neoplasms of the bile duct: Stepwise progression to carcinoma involves common molecular pathways[J]. Mod Pathol, 2014, 27(1): 73-86. DOI: 10.1038/modpathol.2013.112. [11] YING S, YING M, LIANG W, et al. Morphological classification of intraductal papillary neoplasm of the bile duct[J]. Eur Radiol, 2018, 28(4): 1568-1578. DOI: 10.1007/s00330-017-5123-2. [12] UEMURA S, HIGUCHI R, YAZAWA T, et al. Prognostic factors for surgically resected intraductal papillary neoplasm of the bile duct: A retrospective cohort study[J]. Ann Surg Oncol, 2021, 28(2): 826-834. DOI: 10.1245/s10434-020-08835-6. [13] MIURA S, ONO M, HAYASHI T, et al. EUS-guided choledochoduodenostomy for cholangitis caused by mucin derived from intraductal papillary-mucinous neoplasms penetrating the bile duct[J]. Gastrointest Endosc, 2015, 81(5): 1266-1267. DOI: 10.1016/j.gie.2014.08.036. [14] ARAI J, KATO J, TODA N, et al. Long-term survival after palliative argon plasma coagulation for intraductal papillary mucinous neoplasm of the bile duct[J]. Clin J Gastroenterol, 2021, 14(1): 314-318. DOI: 10.1007/s12328-020-01199-0. [15] NATOV NS, HORTON LC, HEGDE SR. Successful endoscopic treatment of an intraductal papillary neoplasm of the bile duct[J]. World J Gastrointest Endosc, 2017, 9(5): 238-242. DOI: 10.4253/wjge.v9.i5.238. [16] TOMINAGA K, KAMIMURA K, SAKAMAKI A, et al. Intraductal papillary neoplasm of the bile duct: A rare liver tumor complicated by malignancy[J]. Hepatology, 2017, 66(5): 1695-1697. DOI: 10.1002/hep.29266. -



 PDF下载 ( 2403 KB)
PDF下载 ( 2403 KB)

 下载:
下载: